Mental-Physical Comorbidity in Korean Adults: Results from a Nationwide General Population Survey in Korea
Article information
Abstract
Objective
The aims of this study were to estimate the prevalence of mental-physical comorbidity and health-threatening risk factors in subjects with mental disorders, and the risks of mental disorders in those with physical diseases for the last 12 months in the general Korean population.
Methods
Korean Epidemiologic Catchment Area study replication (KECA-R) was conducted for 6,510 adults between August 2006 and April 2007. The Korean version of Composite International Diagnostic Interview 2.1 (K-CIDI) was used in the survey. Prevalence of mental and physical disorders, and risk factors for physical health were calculated, and their associations were evaluated with adjustment for age and sex.
Results
Subjects with any mental disorder showed significantly higher prevalence of chronic physical conditions (adjusted odds ratio, AOR=1.5 to 2.8, p<0.001) and medical risk factors including smoking, heavy drinking, overweight, and hypertension (AOR=1.5 to 4.0, p<0.001). Of those with chronic physical conditions, 21.6% had one or more comorbid mental disorder compared with 10.5% of the subjects without chronic physical disorders (AOR=2.6, p<0.001). Contrary to expectations, depressive disorders did not show significant association with hypertension and prevalence of obesity was not influenced by presence of mental disorders. Further studies should assess these findings.
Conclusion
This is the first identification of significant mental-physical comorbidity in the general Korean population. Clinicians and health care officials should keep in mind of its potential adverse effects on treatment outcome and aggravated disease-related socioeconomic burden.
INTRODUCTION
A substantial body of literature has demonstrated significant comorbidity rate of mental and chronic physical conditions.1 Patients with mental disorders and psychological stress are at greater risk of various physical conditions including cardiovascular disease,2 diabetes mellitus,3 asthma,4 peptic ulcer,5 chronic pain and musculoskeletal disease.67 Conversely, chronic physical disorders have been reported to be associated with higher prevalence of psychological distress and mental disorders.8 It may be that mental and physical disorders are associated in bidirectional manners, in which physical disorders increase risks of mental disorders and vice versa.9 Furthermore, mental-physical comorbidity might reflect an integrated pathophysiologic mechanism involving the central nervous, neuroendocrine, and immune systems.10
Socioeconomic burden of mental and chronic physical disorders has been growing despite the remarkable progress in public health management during the last century.1112 In 1977, Gruenberg proposed the concept of "the failure of success", asserting that the technological success in reduction of mortality rate not only extended the life expectancy, but also increased average duration of chronic physical and mental conditions.13 Consequently, comorbidity of mental and physical disorders has become a major challenge to medicine and public health.14 It is related with greater socioeconomic burden than simple sum of each condition's adverse effects on role impairment,15 health care costs,16 premature mortality risk,14 and global score of disability.17 In this regard, it can be postulated that mental-physical comorbidity is a significant threat to individual and public health in Korea because the nation has been one of the most rapidly developing countries for the past decades. Therefore, it is essential to identify the reality of mental-physical comorbidity among the representative general population of Korea to establish national health policies.
The aims of present study were to estimate the prevalence of mental-physical comorbidity, clarify the risk factors for those conditions among subjects with 12-month major mental disorders, and ascertain the prevalence of 12-month major mental disorders among those with chronic physical conditions in the general Korean population.
METHODS
Data acquisition
Data were derived from Korean Epidemiologic Catchment Area study replication (KECA-R),18 a nationally representative survey based on DSM-IV.19 The survey was conducted from August 1, 2006 through April 30, 2007. The target population included all eligible residents aged 18–64 years listed in the updated 2005 population census at community registry offices.20 A multistage, cluster sampling of the subjects was carried out across 12 catchment areas, with selection according to the population size of each division and accessibility to research centers. A total of 6,510 respondents completed the diagnostic interviews. Detailed information on the sampling process are described elsewhere.18
Assessment of psychiatric disorders
The Korean version of Composite International Diagnostic Interview 2.1 (K-CIDI) was administered to all eligible subjects by trained interviewers. K-CIDI is a fully structured and validated diagnostic interview21 following the guidelines of the World Health Organization.22 Psychiatric diagnoses in the past 12 months were identified using the definition and criteria of DSM-IV.19 Twelve-month depressive disorders (major depressive disorder and dysthymic disorder), anxiety disorders (obsessive-compulsive disorder, posttraumatic stress disorder, panic disorder, agoraphobia, social phobia, generalized anxiety disorder, and specific phobias), and substance use disorders (alcohol and nicotine use disorders) were included in the analyses. Psychotic and bipolar disorders were not included because the numbers of the subjects were too small for the analyses (19 and 17 out of 6,510 participants for psychotic and bipolar disorders, respectively).
Assessment of chronic physical conditions
Chronic physical conditions were assessed using the modified Cumulative Illness Rating Scale (CIRS)23 and K-CIDI questions on chronic pain. Physical disorders in the last 12 months were grouped into 9 categories: chronic pain and musculoskeletal disease (e.g., headache, arthritis, neck and back pain), hypertension, cardiovascular disease (heart and vascular disease), respiratory disease (lung, bronchi and tracheal disease), gastrointestinal disease (upper and lower gastrointestinal tract, and hepatic disease), renal and genitourinary disease (kidney, uterus, bladder, urethra, prostate and genital disease), neurological disease (brain, spinal cord and peripheral nerve disease), endocrine-metabolic disease (diabetes, infections, and toxicity), and disease of eye, ear, nose, and throat. A recent study revealed high agreement of case ascertainment between self-report and physician's diagnosis of physical disorders.24
Assessment of medical risk factors
We additionally assessed major health risk factors in subjects with 12-month mental disorders. Derived from a recent report of The Global Burden of Disease Study (GBD) 2010,25 we could identify and estimate 4 leading risk factors in Korea using K-CIDI and CIRS: current smoking, heavy drinking, overweight (Body Mass Index, BMI ≥25 kg/m2), and hypertension.
Statistical analyses
Stata Statistical Software for Windows, Release 12.1 (StataCorp LP. 2011., College Station, TX, USA) was used to perform the analyses. Survey weights were calculated for the participants and used to adjust the data to approximate the national age and sex distributions according to 2005 Korea census.20 Weighted prevalence with 95% confidential intervals were calculated, and logistic regression analyses were conducted among the diagnostic groups with controlling for age and sex. Adjusted odds ratios (AORs) for each mental and physical condition groups were calculated compared to with participants with no identified disorders. A p-value≤0.05 was considered to be significant.
Ethics statement
The Institutional Review Board of Seoul National University College of Medicine approved this study (C-0607-009-177). All subjects were fully informed about the aims and methods of the study, and written informed consent was obtained prior to participation.
RESULTS
Chronic physical disorders of subjects with mental disorders
As shown in Table 1, participants with any mental disorder, compared with those with no mental disorder, had significantly higher 12-month prevalence of chronic physical disorders, apparently in chronic pain and musculoskeletal disease (31.7% vs. 19.4%), hypertension (11.2% vs. 8.5%), cardiovascular disease (10.0% vs 6.0%), respiratory disease (13.3% vs. 5.9%), gastrointestinal disease (30.4% vs. 14.1%), renal and genitourinary disease (9.1% vs. 5.7%), neurological disease (4.2% vs. 1.7%), endocrine-metabolic disease (5.3% vs 3.3%), and eye, ear, nose, and throat disease (19.2% vs. 10.6%) (All p<0.001). Similar trends were observed when the risks of physical conditions were analyzed for depressive, anxiety and substance use disorders, although depressive disorders did not show significantly higher odds of hypertension (11.6% vs. 8.5%; AOR=1.4, p=0.186) and endocrine-metabolic disease (5.5% vs. 3.3%; AOR=1.6, p=0.208). Overall, subjects with any mental disorder showed significantly higher risks of chronic physical condition than those without mental disorders (67.9% vs. 47.9%; AOR=2.7, p<0.001).
Key risk factors for chronic physical disorders in subjects with mental disorders
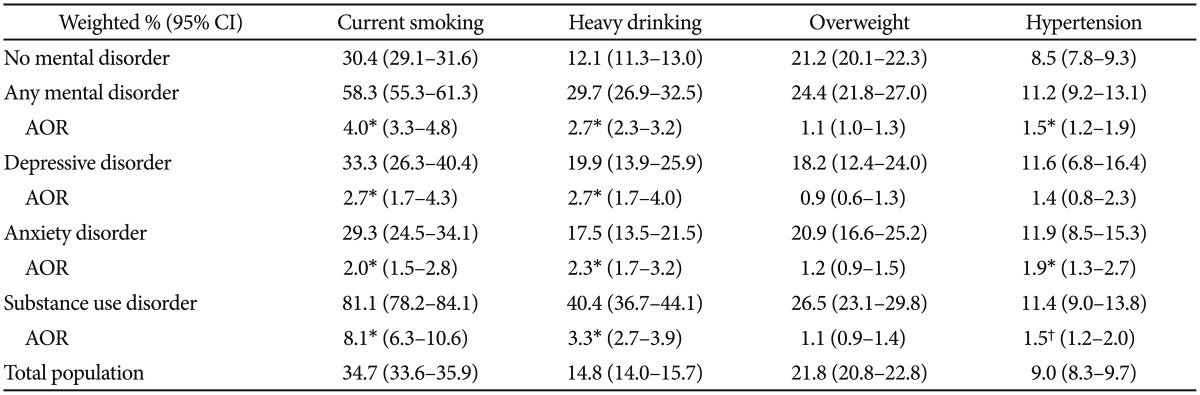
Any mental disorder was related with greater risk factors for physical health (Table 2). Significantly higher 12-month prevalence of current smoking (58.3% vs. 30.4%), heavy drinking (29.7% vs. 12.1%), and hypertension (11.2% vs. 8.5%) were observed among subjects with any mental disorder compared with those without mental disorders (p<0.001 for all comparisons). As expected, prevalence of current smoking (81.1%) and heavy drinking (40.4%) were higher in respondents with substance use disorder comprising nicotine and alcohol use disorders (both p<0.001). Subjects with depressive and anxiety disorders also showed significantly higher prevalence of current smoking (33.3% and 29.3% respectively) and heavy drinking (19.9% and 17.5%, respectively) than those without mental disorders (p<0.001 for all comparisons). Prevalence of overweight was not significantly different between participants with and without any mental disorder (24.4% vs. 21.2%, p=0.116), and this trend was replicated in the analyses for separate mental disorder categories. Additionally, difference in prevalence of class I (BMI ≥30 kg/m2) and II (BMI ≥35 kg/m2) obesity also did not reach the level of significance for all comparisons (data not shown).
Mental disorders of people with chronic physical disorders
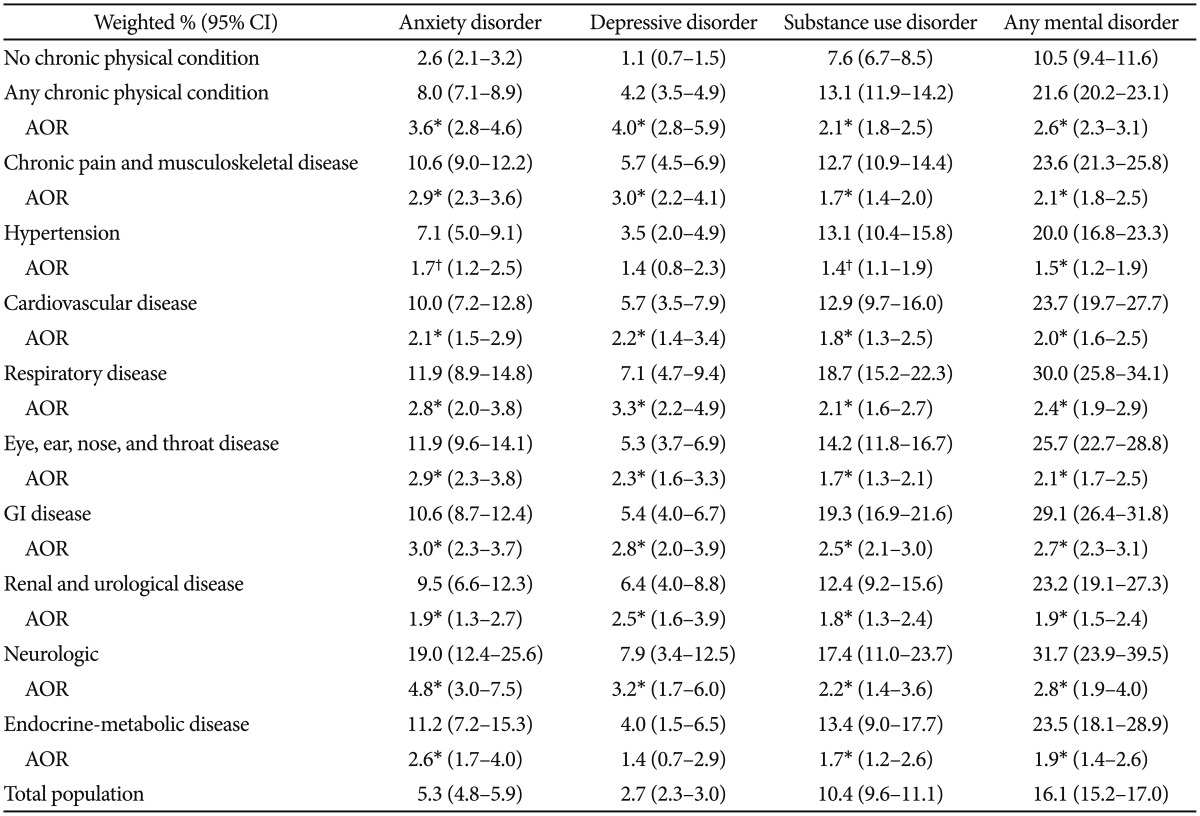
Table 3 shows the 12-month prevalence and AORs of each mental disorder in subjects with chronic physical disorders. Any chronic physical disorder was associated with significantly high risk of mental disorders (21.6% vs. 10.5%; AOR=2.6, p<0.001). Substance use disorders were the most prevalent mental disorders among the respondents with chronic physical disorders (13.1%), nevertheless the AORs for depressive and anxiety disorders (AOR=4.0 and 3.6, respectively, p<0.001) were higher than that of substance use disorders (AOR=2.1, p<0.001). However, prevalence of depressive disorders appeared not to be significantly higher for subjects with hypertension (3.5%; AOR=1.4, p=0.22) and endocrine-metabolic disease (4.0%; AOR=1.4, p=0.29) than for those without any identified chronic physical disorder (1.1%).
DISCUSSION
In the present study, subjects with major mental disorders presented significantly higher risks of chronic physical disorders than those without any mental disorder. The prevalence of one or more chronic physical disorders was approximately two-thirds among the subjects with major mental disorders (67.9%) and about half (47.9%) among those without mental disorders. In addition to physical disorders, risk factors for physical health were more prevalent among the subjects with mental disorders, except overweight and obesity. The results also corroborate previous findings that chronic physical disorders are associated with more than twice the risk of any mental disorder.14 In summary, mental and physical disorders are significantly correlated with higher prevalence of each other in a representative general population of Koreans.
To our knowledge, this is the first report concerning the epidemiology of mental-physical comorbidity in a nationwide general Korean population. The strength of this paper is that we surveyed for major mental disorders and wide range of chronic physical conditions. Finding of significant mental-physical comorbidity in the present study is consistent with previous reports.14 This could reflect an integrated pathophysiologic mechanism, which would be counter to the traditional "mind-body dualism" in terms of psychiatry vs. bodily medicine.2627 Depressive and anxiety disorders predict development of coronary heart disease,2 stroke,28 type 2 diabetes mellitus,29 asthma,4 gastrointestinal disease,30 and chronic pain.6 It has been postulated that disturbances in the stress management system involving catecholamines and glucocorticoids are associated with development of depressive and anxiety disorders.10 Dysregulation of these hormones also has been related with various adverse effects including higher risks of atherosclerosis, elevated blood glucose levels, insulin resistance, obesity, and increases in inflammatory response and immunosuppression.14 In addition, mental disorders could contribute to development of physical disorders through behavioral risk factors, such as lack of exercise, and as replicated in this study, smoking and heavy alcohol drinking.931 Conversely, various physical disorders are reportedly related with greater risks of developing mental disorders.14 Researchers suggested that physical disability,32 and changes in behaviors and social relations33 would promote subsequent development of mental disorders. Biological mechanisms from physical to affective disturbances have been also implicated, including direct (e.g., endocrine, neurochemical, and metabolic disturbances) and indirect (e.g., medications and cranial irradiation) pathways.33 The collective present and prior data support the view that the relationship between mental and physical disorders might be bidirectional, in which they simultaneously precipitate and exacerbate each other in a vicious cycle.33 Mental and physical disorders might have an integrated neurobiological basis.10 From this point of view, the brain is the key organ in adaptation to acute and chronic stress of life experiences with genetic variations, epigenetic modifications, behavioral changes, and regulation of physiological responses. If the burden of stress causes overload in the brain and body, it could lead to either mental or physical disorders.10
The current findings support a mental-physical bidirectionality or integrated pathophysiology of mind and body. However, the present study did not identify the relevance of depression to hypertension and endocrine-metabolic disease, and significant difference in prevalence of overweight and obesity between subjects with and without mental disorders. Implications of these findings are discussed below.
The relationship between depression and hypertension has been controversial. Depression has been reported to be a predictor of later development of hypertension,34 and a recent meta-analysis study suggested that depression is an independent risk factor for development of hypertension.35 Contrarily, depression may not be related with hypertension when blood pressure is more precisely evaluated.36 Additionally, another result of recent meta-analysis did not support the hypothesis that hypertension is a probable risk factor of depression.37 Furthermore, low blood pressure was associated with depressive symptoms among older subjects whether or not they were treated for hypertension.38 These contradictory findings might have been resulted from complex bio-psycho-social interactions. Chronic stress and the non-adaptive response to it might elevate blood pressure, rather than acute stress.39 On the other hand, comorbidity of low blood pressure and depression might arise through impaired cardiovascular control and subsequent reduced cerebral perfusion, and monoamine hypoactivity.38 Future studies will be needed to provide clarification.
Although this study did not reveal the significant association between depression and endocrine-metabolic disease, depression is well-known to be in bidirectional association with diabetes29 and metabolic syndrome.40 Therefore, any premature assumption should not be inferred from the present results. Because the "endocrine-metabolic disease" category of CIRS does not assess diabetes and other endocrine or metabolic diseases as separate diagnoses and does include other conditions (e.g., infections, poisonings and breast pathology), it might have made the associations equivocal.
Contrary to previous studies from the Western countries,9314142 overweight and obesity were not more prevalent among people with depressive and anxiety disorders than normal population in this study. This finding is consistent with a previous result in which the authors reported no significant association between obesity and depressive disorders.43 Obesity can be resulted from interactions of genetic, behavioral, and environmental factors,44 and it might have shared genetic susceptibility with depression.45 A recent meta-analysis revealed that overweight and obesity predicts future development of depression, and depression increases the odds for obesity over time but not for overweight.46 In the present study, we did not identify this reciprocal relationship between any major mental disorders and obesity. This difference could be accounted for by several reasons. First, our study is a cross-sectional survey that might have been inappropriate to observe the cumulative effect of time and environmental factors. Second, relatively low prevalence of mental disorders18 and obesity47 in Korea might have attenuated the manifestation of multifactorial association among bio-psycho-social factors. In this regard, cross-cultural and symptomatological differences could attribute to higher diagnostic threshold of mental disorders in Korea,4849 which might have caused selection biases. Additionally, comparatively low prevalence of overweight and obesity in Korea47 might reflect ethnic differences in metabolic control mechanisms. Third, overweight might not be a noteworthy risk factor for mental and physical health in Korea. A recent international study carried out on more than 1 million participants revealed that East Asians (Chinese, Japanese, and Koreans) with BMI of 22.6 to 27.5 kg/m2 showed the lowest risk of death.50 As mentioned earlier, another previous investigation reported that higher prevalence of depressive disorder was significantly associated with underweight (BMI ≤18.5 kg/m2), not with overweight (BMI ≥25 kg/m2) in a general Korean population.43 Instead, overweight was rather found to be related with lower prevalence of depressive disorder in male participants in the study. The researchers suggested that cultural differences (e.g., collectivism vs. individualism) and ethnicity might account for this phenomenon, but there has not been a clear explanation. Fourth, to clarify the adverse effects of obesity on mental health in detail, it might be necessary to estimate the relationship between various measures of obesity besides BMI (e.g., waist circumference, waist-to-hip ratio and waist-to-height ratio) and mental symptom dimensions as investigated in an earlier study.51 Conclusively, shared neurobiological substrate among various mental and physical disorders, eating behaviors, and metabolic control should be elucidated in future investigations.
Mental-physical comorbidity increases personal and socioeconomic burden in terms of more severe symptoms, poor self-management, poorer disease prognosis, higher health care costs, and premature mortality.14 Futhermore, role impairment and global disability are more severely deteriorated by mental-physical comorbidity than simple sum of the adverse effects.1517 Therefore, it should be considered in both clinical settings and the policy-making process to promote more efficacious treatment and improve the health care system simultaneously.
Limitations
The present study has several limitations. First, the results should be interpreted cautiously because of its retrospective and cross-sectional design. There might have been recall bias affecting the prevalence of wide range of mental and physical disorders, and the results indicate association, not causality. Second, non-response to the survey might have been related with possible false negative results, because subjects with severe psychiatric symptoms or cognitive impairment might have difficulties in completing the questionnaires.5253 Thus, there might have been paradoxical under-diagnosis of severe psychiatric disorders. Third, the possibility of false negative also might have been attributable to the household-based sampling design, because institutionalized or homeless individuals were not included. Fourth, Diagnostic reliability of physical disorders could have been insufficient, because it was based on self-report not on precise medical assessment. However, a high degree of agreement in the diagnosis between self-report and physician's diagnosis has been reported.24 Fifth, we did not separately assess diabetes mellitus which is one of most prevalent chronic illness. It is due to that we used CIRS which measures chronic medical illnesses as categorized groups rather than separate diagnoses. Considering that 46.3% of diabetic patients are assumed to be undiagnosed,54 it is possible that the prevalence of endocrine-metabolic disease category in CIRS and its comorbidity with mental disorders might have been underrated. Sixth, we could not identify the correlation between symptom severities of mental disorders and physical disorders, because we used K-CIDI which had been developed to make diagnosis of mental disorders, not to rate the severity. Finally, despite we administered a completely structured diagnostic tool for mental disorders, the possibility of interviewer-respondent interaction cannot be excluded.
Conclusion
This study examined the prevalence of mental-physical comorbidity, the risk factors for those conditions among those with 12-month major mental disorders, and the prevalence of 12-month major mental disorders among those with chronic physical conditions in the general Korean population. A significant mental-physical comorbidity rate and higher prevalence of risk factors for chronic medical disorders were evident among subjects with mental disorders. Conversely, existence of chronic physical disorders was associated with higher rate of mental disorders. These results are comparable to those of previous reports and support a mental-physical bidirectionality. Considering its potential threat to public health and psychosocial burden, mental-physical comorbidity should be comprehensively dealt with not only in individual treatment but also in process of health care policy-making.
Acknowledgments
This study was funded by the Korean Ministry of Health and Welfare, which had no role in study design; the collection, analysis, and interpretation of data; the writing of the report; or the decision to submit the paper for publication. The authors thank the interviewers and the Korean Ministry of Health and Welfare for their cooperation and help.