The Impact of General Medical Conditions in Obsessive-Compulsive Disorder
Article information
Abstract
Objective
The co-occurrence of general medical conditions (GMCs) and major psychiatric disorders is well documented. The aim of this study was to assess the prevalence of GMCs in patients with a primary diagnosis of obsessive-compulsive disorder (OCD) and, secondly, to investigate which clinical variables are associated with the presence of a GMC.
Methods
Subjects with a primary diagnosis of OCD were included. Socio-demographic and clinical characteristics were collected. GMCs were classified using the ICD-10 and grouped according to the Cumulative Illness Rating Scale (CIRS) in: cardiac, vascular, hematopoietic, respiratory, ear/nose/throat, upper and lower gastrointestinal, hepatic, renal, genitourinary, musculoskeletal, neurologic, endocrine/metabolic. The association between the presence of GMCs and demographic/clinical variables of OCD was investigated.
Results
A total of 162 patients with OCD were included. 78 (48.1%) patients had at least one comorbid GMC. Most frequent GMCs were endocrine/metabolic diseases (25.9%), followed by upper/lower gastrointestinal (20.5%) and cardio-vascular diseases (13.6%). The presence of a GMC was significantly associated with female gender, older age, duration of untreated illness (DUI), and absence of physical activity.
Conclusion
Patients with OCD have high rates of comorbid GMCs. A longer DUI is associated with having at least one GMCs; this might be due to the long-lasting adoption of unhealthy lifestyles, not counterbalanced by appropriate treatment and psychoeducation.
INTRODUCTION
The National Comorbidity Survey Replication (NCS-R) in the US found that at least 68% of subjects with a psychiatric disorder had at least one comorbid general medical condition (GMC), while 29% of those with a GMC had at least a comorbid psychiatric disorder [1]. A population study, conducted in Singapore, found that the rate of any physical disorder in those with psychiatric disorders was 50.6% [2]. Several other studies confirmed that psychiatric disorders frequently co-occur with GMCs [3-5] and this co-occurrence has been particularly documented in patients affected by bipolar disorder, schizophrenia and depressive disorders [6-8].
The high occurrence of GMCs in patients with mental disorders can be explained in three ways: the impact of psychopharmacological treatments (mainly second-generation antipsychotics), illness-related factors such as the adoption of unhealthy lifestyles associated with the psychiatric disorder itself (i.e., increased caloric intake, cigarette smoking, alcohol use and low physical activity), and probably inherited biological factors such as hypothalamic pituitary adrenal axis dysregulation. For example, in a recent review study, Mansur and coworkers concluded that obesity and mood disorders are intrinsically linked and share a series of clinical, neurobiological, genetic and environmental predisposing factors [9].
Several research and review studies evaluated the prevalence of GMCs in patients with bipolar disorder or schizophrenia. These patients suffer more frequently from cardiovascular diseases, hypertension, diabetes, endocrine diseases such as hypo-hyperthyroidism, respiratory diseases such as asthma or chronic obstructive pulmonary illness, liver and/or renal conditions, peptic ulcer, and arthritis [10-12].
The relationship between anxiety disorders or obsessivecompulsive spectrum disorders and GMCs is less documented. Some studies found significant associations between anxiety disorders and cardiac disorders, hypertension, gastrointestinal problems, genitourinary disorders and migraine [13-15]. On the other hand, clinical studies also suggested that anxiety disorders could be an early manifestation of GMCs [16-18]. Only few studies investigated prevalence rates of metabolic syndrome (MetS) in patients with a primary diagnosis of anxiety disorders; rates of MetS, from 21.2% to 47.8%, are higher than those in the general population [19-23]. In OCD patients, the long-term (1-year) use of antipsychotics added to SRIs has been associated with an increase in body mass index and fasting blood sugar [24]. Moreover, the use of a long-term antidepressant therapy (serotonin reuptake inhibitors) is also associated with a significant weight gain [25].
Despite the considerable body of research examining GMCs in other psychiatric disorders, there is little research examining the physical health of patients with OCD: as a result, comorbid GMCs may be underdiagnosed and undertreated in clinical practice in subjects with OCD.
The aim of this study was to assess the prevalence of GMCs in patients with a primary diagnosis of OCD and, secondly, to investigate which clinical variables are associated with the presence of a GMC.
METHODS
Subjects
The study had a naturalistic design and involved patients with a primary diagnosis of OCD consecutively admitted to the Mood and Anxiety Disorders Unit, Department of Neuroscience, University of Turin (Italy) from January 2013 to December 2015. This is a tertiary referral center mainly for patients from Piedmont and Aosta’s Valley regions, located within the University General Hospital, specialized in the treatment of patients with OCD.
Subjects with a principal diagnosis of OCD according to the DSM-IV TR, with a minimum total score of 16 on the Yale-Brown Obsessive Compulsive Scale (Y-BOCS) and with at least 18 years old were included in the study.
Exclusion criteria were: primary diagnosis of schizophrenia, schizoaffective disorder, bipolar disorder, delusional disorder, severe personality disorders (such as borderline and antisocial), substance use disorders; pregnancy or recently given birth, refusal to sign the informed consent before starting the study.
Participants expressed willingness to take part in the study by signing a written consent after the aims of the study and study procedures were thoroughly explained. All subjects were of Caucasian Italian origin. The study design was reviewed by the local ethics committee.
Assessments and procedures
Data were obtained through the administration of a semistructured interview, used in our previous studies [23,25] with a format that covered the following areas: socio-demographic data, diagnostic evaluation (by means of the Structured Clinical Interview for DSM-IV Axis I and II Disorders), age at onset of OCD, duration of untreated illness (DUI), defined as time from onset of the disorder to first correct treatment received, body mass index (BMI). Lifestyles were also investigated: information about exposure to cigarette smoking and physical exercise were obtained by directly interviewing the patients. A score was assigned to the frequency of physical exercise: absent, mild (<4 h/week), moderate (4 h/week with a tolerance of ±30 min) and intense (>4 h/week, regular).
In addition, the following rating scales were included in the assessment: Y-BOCS, Hamilton Anxiety Rating Scale (HAM-A), Hamilton Depression Rating Scale (HAM-D), Clinical Global Illness - Severity (CGI-S).
The inter-rater reliability of DSM-IV diagnoses using the SCID-I was tested before the beginning of the study (>0.80 for the presence of any lifetime Axis I disorders). Inter-rater reliabilities of the Y-BOCS, HAM-A and HAM-D total scores were also good (>0.80).
The presence of GMCs was investigated using ICD-10 diagnoses; moreover, we grouped GMCs according to the Cumulative Illness Rating Scale (CIRS) [26] as follows: cardiac, vascular, hematopoietic, respiratory, ear/nose/throat, upper and lower gastrointestinal, hepatic, renal, genitourinary, musculoskeletal, neurologic, and endocrine/metabolic.
Statistical analysis
All statistical analyses were performed using SPSS version 20.0 (IBM Corp., Armonk, NY, USA) and the value of statistical significance was set at p<0.05.
The socio-demographic and clinical characteristics of the subjects were represented as mean and standard deviation (SD) for continuous variables and in terms of frequency and percentage regarding categorical variables. GMCs according to CIRS system were summarized as percentages.
The sample was divided in two subgroups according to the presence/absence of at least one GMC. In order to analyze differences between these two subgroups, we used the Pearson χ2 test with Yates correction for the comparison of categorical variables, and t-test for independent samples for continuous variables.
A logistic regression analysis was finally used to explore the relationship between the presence of GMCs in patients with OCD (dependent variable) and each of the other independent variables previously found associated in the statistical analyses. The probability of entering the equation was set at 0.05.
RESULTS
We reported data on 162 patients with a primary diagnosis of OCD. We excluded 30 BD or schizophrenia patients with comorbid OCD. Other 12 patients were excluded because they declined to participate. Lastly, six patients showed a YBOCS total score inferior to 16 after initial assessment and therefore they were not considered for this study.
Patients had a mean age of 35.6±14.4 years; 96 (59.3%) were males. Mean age at onset of OCD was 19.3±7.3 years, with a mean DUI of 115.9±113.6 months. Socio-demographic and clinical characteristics of subjects included in the present study are summarized in Table 1.
A total of 78 (48.1%) patients had at least one comorbid GMC. Most frequent GMCs were endocrine/metabolic diseases (25.9%), followed by upper/lower gastrointestinal (20.5%) and cardio-vascular diseases (13.6%). Among endocrine/metabolic diseases, most frequent conditions were hypercholesterolemia (n=40, 24.7%), hypo/hyper-thyroidism (n=22, 13.6%), ten cases of diabetes mellitus (6.2%) (two insulin-dependent diabetes mellitus). Among upper/lower gastrointestinal diseases, most frequent conditions were gastroesophageal reflux (n=25, 15.4%), Gilbert’s syndrome (n=10, 6.2%), seven cases (4.3%) of chronic intestinal inflammatory diseases and cholelithiasis. Lastly, among cardio-vascular disease, most frequent conditions were hypertension (n=20, 12.3%), anemia (n=13, 8.0%), and eight cases (4.9%) of valvular heart diseases. According to NCEP ATP III, 32 patients (19.8%) met the criteria for metabolic syndrome.
Regarding pharmacological treatment, the vast majority of patients were taking medium-to-high doses of serotonin reuptake inhibitors (SRIs) according to International guidelines. Some patients were taking also low dosage antipsychotics (mainly aripiprazole, olanzapine or risperidone) as augmentation treatment. Table 2 shows current pharmacological treatment of subjects with or without GMC. No significant differences were found between the two groups.
When we divided our sample according to the presence/absence of at least one GMC and compared the two subgroups, patients with GMCs were more frequently females (56.4% vs. 26.2%, p=0.006), were older (42.0±15.4 vs. 29.7±10.6 years, p<0.001), had a longer DUI (153.0±134.9 vs. 77.0±80.7 months, p=0.003), and had no physical activity (51.3% vs. 76.2%, p=0.019) (Table 3).
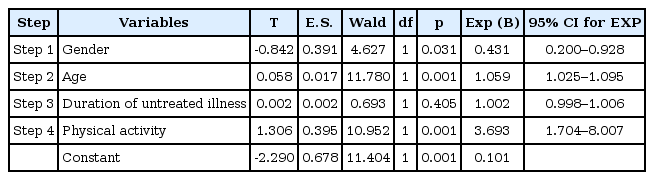
However, when we performed a stepwise logistic regression analysis, the duration of untreated illness no longer predicted the presence of a GMC (Table 4).
DISCUSSION
The primary aim of our study was to assess the prevalence of GMCs in patients with OCD. The prevalence of at least one GMC was 48.1% in our sample, demonstrating the high occurrence of physical morbidity in subjects with OCD. Different models have been proposed to explain the high co-occurrence of anxiety disorders in general and physical diseases: anxiety may be a consequent or antecedent factor of a physical illness, third variables may lead to the comorbidity or, common genetic, environmental or personality factors may contribute to the co-occurrence [27].
The most prevalent GMCs were endocrine/metabolic diseases (25.9%) while the prevalence of metabolic syndrome was 19.8%. This result is in line with our previous study in OCD subjects where the MetS prevalence was 21.2% [23]: to the best of our knowledge, no other studies on MetS in OCD patients were conducted and, although we could not perform any direct comparison, this prevalence is similar to that observed in the Italian general population (16–17.8%). However, the mean age of our sample was 35.6 years, and the result of a prevalence rate of nearly 20% of MetS in this group is of clinical relevance. The age-adjusted prevalence of MetS in the US general population is 27.0% [28], while European studies have found lower rates, between 8% and 17.8% [29-32]. A recent study, conducted on 97 patients with severe OCD, showed a similar prevalence of endocrine/metabolic diseases (23.7%) [33].
There is a strong association between weight gain, obesity or metabolic abnormalities and psychopharmacological treatments, particularly second-generation antipsychotics (i.e. olanzapine or asenapine or quetiapine) and antidepressants with high H1-histamine receptor affinity (i.e. tricyclics and mirtazapine) due to counteracting the central anorexigenic effects of histamine or increasing adipose tissue deposition [34]. A meta-analysis based on 116 studies employing most marketed antidepressants highlighted that different antidepressant medications greatly differ in affecting body weight. The authors found that tricyclics and mirtazapine were associated with the maximum weight gain, where most SSRIs, SNRIs and bupropion induced very little, if anything, weight gain [35]. On the other hand, a systematic review recently highlighted the association between use of antidepressants and new onset type 2 diabetes [36]. Together with illness-related factors such as the adoption of unhealthy lifestyles and probably inherited biological factors, specific pharmacological treatments could play a significant role in leading to the MetS [34,37-39].
Our prevalence rates of cardio-vascular and neurological diseases are comparable of those found in subjects with mental disorders by a population study conducted in Singapore [2]. Despite these similarities, we found lower prevalence rates of cardio-vascular, musculoskeletal, respiratory, genitourinary and neurological disorders compared to other studies and higher prevalence rate on gastrointestinal diseases [33,40]. This result could be explained by different methodology used and sample recruitment: for example, Drummond and coworkers considered only patients with severe OCD (subjects with severe OCD could have more physical burden).
The prevalence of any GMCs or a specific class of GMCs in a sample of subjects with a given psychiatric disorder has to be interpreted also comparing these rates with those in other psychiatric disorders.
The relationship between GMCs and major depression disorder was investigated in the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study. The prevalence of significant medical comorbidity in this population was 52.8%, similar to that found in our OCD population; concurrent GMCs appeared to influence the severity and symptom patterns in MDD [41].
Compared to depression, the link between anxiety disorders and physical health is relatively understudied. Individuals with elevated anxiety are more likely than those without anxiety to have a wide array of medical conditions, including cardiovascular, autoimmune, and neurodegenerative diseases, and are at greater risk for early mortality [42]. In a large community sample (n=42,249), people diagnosed with anxiety disorders were more likely to have a variety of medical conditions including obesity (OR 1.2), diabetes (OR 1.3), asthma (OR 1.6), hypertension (OR 1.7), arthritis (OR 1.7), ulcer (OR 1.9), back/neck problems (OR 2.0), heart disease (OR 2.0), headache (OR 2.3), and multiple pains (OR 2.3) [43].
When examining socio-demographic and clinical characteristics potentially associated with GMCs in patients with OCD, firstly we found a significant association with female gender and older age. This result was quite expected: as a matter of fact, it is obvious that older age implies higher probability of experiencing GMCs. Moreover, females patients in our sample were older than males, although this difference was not statistically significant (data not shown), and this might in part explain the association between female gender and higher rate of GMCs. As we did not include a comparison group without OCD (e.g., from the general population), we cannot conclude that OCD is per se at higher risk of having a GMC beyond the effect of age. However, we do think that clinicians should be aware that approximately half of OCD patients do display a comorbid GMC that needs careful examination and treatment.
Secondly, patients with OCD and comorbid GMCs showed a higher DUI. To the best our knowledge, this is the first study to find an association between a longer DUI and the presence of GMCs in patients with OCD. Although this issue has been adequately studied in patients with schizophrenia and bipolar disorder, to date, only few studies showed the negative impact of a longer DUI in OCD. In previous studies, a longer DUI was significantly associated with poor treatment response (DUI >24 months) [44], specific obsessive-compulsive dimensions (aggressive/checking dimension) [45], older age, early age at onset, and older age of first pharmacological treatment (DUI >4 years). A shorter DUI (<4 years) was associated with abrupt onset of OCD, precipitated by life events [46]. Although the longer DUI no longer predicted the presence of a GMC in the logistic regression analysis, we consider our results worth to be discussed; it is possible that subjects not appropriately treated for years (longer DUI) display unhealthy lifestyles, or have poor access to the healthcare system even for general medical conditions or medical complications of severe OC symptoms (e.g., excessive hand or body washing leading to dermatological problems, avoidance of medical consultations for fear of contamination leading to failure to get appropriate diagnosis and treatment of an independent medical problem). Another explanation is based on alteration of hormonal system due to higher levels of stress that lead to an increase in cortisol levels and consequently poor glucose tolerance and obesity, diabetes, and hypertension. This in turn might lead to an increased risk to develop some GMCs, especially endocrine and cardiovascular diseases.
Lastly, GMCs in patients with OCD were significantly associated with the absence of physical activity. In our sample, fifty-eight patients (35.8%) did not engage in any physical activity. It is known that a lack of physical activity is associated with anxiety disorders while physical inactivity is associated with many chronic physical diseases [47-49], It could be suggested that subjects with OCD are at increased risk to develop GMCs at least in part through physical inactivity.
The benefits of physical activity are well known and are summarized as follows: it promotes fat oxidation reducing the risk of obesity (important cardio-vascular risk factor and core component of MetS), improves insulin sensitivity thus reducing the risk of type 2 diabetes, prevents hypercholesterolemia and/or hypertension reducing the risk of heart disease or several cancers or premature death caused by heart attacks, decreases, in particular among children and young people, risky behaviors such as use of tobacco or alcohol, unhealthy diets, eases anxiety management and stressful situations, reduces the risk of osteoporosis and fractures but also musculoskeletal disorders (e.g., back pain). In the general population, physical activity has been shown to be the optimal strategy to improve both cardio-metabolic parameters and cardiorespiratory fitness levels. Psychoeducational programs are well structured in patients with bipolar disorder and schizophrenia [50-53]. The improvement of anxiety symptoms due to physical activity has been studied in patients with anxiety disorders [54]: in our opinion, these programs should be tested also in patients with OCD to see whether MetS could be prevented.
Obviously, the impact of GMCs associated with OCD is intuitively relevant for several reasons such as a worsened quality of life and functioning, an higher utilization of healthcare resources, and an increased risk of hospitalization and mortality: this supports the need for a proper functioning of healthcare integrated system. A recent population study conducted by Witthauer and coworkers on 4,181 subjects (aged 18–65), evaluated the association between GMCs and subjects with clinical and subthreshold OCD. The authors reported that subjects with both OC symptoms and GMCs reported the highest number of days of disability due to physical or psychological problems during the past 30 days compared to subjects with only OC symptoms, only GMC or neither of them [40]. Less access to care, a no integrated health care system, patient difficulties to clearly describe medical symptoms, and patient shame feelings to discuss some clinical features lead to less attention in the fully evaluation and management of GMC in patients with major psychiatric disorders such as bipolar disorder and schizophrenia [55-57].
The reader should be mindful of a number of limitations in the current study when interpreting our findings. The first one is the cross-sectional design that does not allow inferences on the temporal relationship between the variables and only shows measures of association. Secondly, the lack of a control group from another psychiatric population or the general Italian population. Another limitation is the small sample size recruited for the present study. However, our aim was to look for significant correlations between the presence of GMCs and clinical variables in patients with OCD, and therefore, an healthy group was not needed.
In conclusion, this study emphasizes the need to ensure that GMCs are not overlooked in psychiatric patients in general and in subjects with OCD in particular. We cannot conclude that the prevalence of GMCs is higher in OCD patients as compared to the Italian general population, but the rate of 48.1% in a sample with a mean age of 35.6 years is, to our opinion, clinically relevant. Assessment plus management of GMCs in patients with OCD are basic clinical factors in achieving satisfactory medical and psychiatric outcomes, in terms of stability, treatment adherence, life expectancy as well as quality of life, of these generally disadvantaged populations worldwide. Therefore, all patients should receive adequate evaluation and surveillance of GMCs and this process should be particularly made when patients with OCD are treated with second-generation antipsychotics as augmentation to antiobsessive medications. It might help clinicians and general practitioners to be sensitized for a better dissemination of integrated care system in order to recognize and to accomplish secondary prevention of potentially severe medical complications.