 |
 |
- Search
| Psychiatry Investig > Volume 15(8); 2018 > Article |
|
Abstract
Objective
This study aimed to evaluate psychometric properties of the Munich ChronoType Questionnaire (MCTQ) in a sample of Korean older adults.
Methods
One-hundred ninety two participants aged 65 and over completed interview-based questionnaires about chronotype, insomnia, depression, and anxiety. Additionally, a small subset of subjects completed a 7-day sleep diary and actigraphy measurements.
Results
Morningness-Eveningness Questionnaire (MEQ) scores were significantly negatively correlated with Midpoint of sleep on free days corrected for sleep debt accumulated through weekdays (MSFsc) (r=-0.45, p<0.01) assessed by the MCTQ. MSFsc using the MCTQ was significantly positively correlated with MSFsc assessed by both the sleep diary (r=0.74, p<0.05) and actigraphy (r=0.76, p<0.05). Additionally, MSFsc assessed by the MCTQ was significantly positively correlated with insomnia (r=0.26, p<0.01), depression (r=0.25, p<0.01), and anxiety (r=0.18, p<0.05). Finally, based on MEQ scores, we derived a cut-off score for the MCTQ that distinguishes morning type and other types (intermediate/evening types) in older adults.
Sleep disorders in Korea have been steadily increasing [1]. Although sleep disturbances are present in all age groups, the prevalence of sleep disorders in the elderly is high due to the normal aging process as well as comorbidity with various physical and mental disorders [2-9]. Advances in the circadian rhythm due to aging affects sleep in the elderly, usually characterized by waking up early and feeling excessively sleepy in the afternoon. Changes in circadian rhythm are a direct cause of sleep disturbance [3,10], and are associated with circadian rhythm sleep disorders, especially advanced sleep phase type (ASPS) in the elderly [11].
Chronotype is defined as the sleep-wake time preference based on the individual’s circadian rhythm. Previous studies have found that an overall strong preference for eveningness tendencies is associated with higher severity of depression, insomnia and anxiety in all age groups [12-14]. Consistent findings were also reported in the elderly group, despite having a large proportion of advanced circadian rhythm [9,15,16]. Thus, chronotype appears to be an important factor to consider in the elderly in the context of sleep disturbances and psychological factors.
Assessment tools for measuring chronotype include self-report questionnaires such as the Morningness-Eveningness Questionnaire (MEQ) and physiological tools such as Dim Light Melatonin Onset (DLMO) and polysomnography (PSG) [17]. Although physiological tools may provide more biologically accurate information in assessing chronotype, they are time-consuming, and costly. Currently, the MEQ is the most widely used measure to assess chronotype [18]. However, it does not measure actual sleep times and doesn’t consider important indicators such as weekday-weekend differences in sleep time, which is characteristic of individuals with eveningness tendencies.
The Munich ChronoType Questionnaire (MCTQ), developed by Roenneberg et al. [19], complements the limitations of MEQ and measures actual sleep time by distinguishing weekdays and free days. The MCTQ parameters are midsleep on weekdays (MSW), mid-sleep on free days (MSF), and mid-sleep on free days corrected for sleep debt on weekdays (MSFsc). The MSW and MSF can be calculated through the MCTQ responses, and the MSFsc can be calculated through the MSW and MSF. The MCTQ uses MSFsc as a chronotype indicator, with higher MSFsc reflecting stronger eveningness tendency. Previous studies have found that MSFsc is associated with DLMO [20,21], the melatonin secretion cycle [22], and MEQ scores [21,23,24]. In particular, Zavada et al. [23] found that the MCTQ is more accurate in examining the sleep-wake cycle than the MEQ, and MSFsc is a strong predictor of chronotype.
Previous studies using MCTQ have been conducted on a broad range of age groups mixed together, rather than only on the elderly [25,26]. Many studies using MEQ have been conducted on elderly groups [27-30] and have been validated for the middle-aged (44-58 years) group specifically, highlighting the need to propose new cut-off scores that reflect changes in circadian rhythm that vary with age [31]. There have been various cut-off criteria for establishing chronotype in the MCTQ that have been used in previous studies, using 2.5%, 15%, and 20% of extreme scores of the sample [32,33]. However, previous studies using MCTQ for all age groups have been limited in that they do not reflect the characteristics of the elderly, who tend to have advanced sleep schedule [12,25,34].
Considering that older adults have circadian rhythm changes and situational factors (i.e., retirement) that are quite different from young adults, it is necessary to consider chronotype in elderly individuals. In this study, we aimed to validate the MCTQ to assess chronotype in Korean older adults and suggest cut-off scores in classifying chronotype in this age group.
A total of 211 participants aged 65 and over were recruited. The subjects were recruited from elderly welfare centers and elderly centers in Seoul and Gyenggi-do, Korea, and only those who agreed to participate in this study were included. Nineteen subjects with possible cognitive impairment based on the MMSE-DS scores [35] and 15 subjects who reported using an alarm clock on free days were excluded. Thus, 177 participants were used for final analyses. Additionally, a small subset of participants (n=8) agreed to also complete sleep diaries and wear the actigraph for 7 days.
Prior to the study, all participants completed informed consent. All questionnaires were interview-based, administered by trained research assistants following a standardized protocol. Participants were administered the Korean version of Mini-Mental State Examination for Dementia Screening (MMSE-DS) [35] to screen for cognitive impairment. This study was approved by the Institutional Review Board of the institute where the research was conducted.
All subjects answered a questionnaire to provide basic information such as age, gender, education years, subjective health status, and medical illness status. The subjective health status was scored from 1 (very healthy) to 5 points (very unhealthy), and the medical illness status was answered with disease or no disease.
The MCTQ was developed by Roenneberg et al. [19] and estimates chronotype by measuring actual sleep timing, distinguishing work and free days. We used the Korean MCTQ, which has been validated for young adults in their 20s and 30s (under review) [36]. The MCTQ measures various sleep parameters such as bed time (BT) and lights off (LO) on weekdays and free days, respectively. MSFsc was used as a marker of chronotype in this study. For the purposes of this study, we modified the first question (i.e. “Do you have a regular working schedule?”) into “Do you sleep differently on weekdays and free days?” because Korean older adults aged 65 and over may not have different sleep schedules on weekdays and free days. Participants who answered “no” to this question completed only to the free days portion on the MCTQ.
The MEQ was developed by Horne and Ostberg [18] and has been validated in Korean [37]. It is a 19-item self-report questionnaire and measures individual’s chronotypes based on sleep preference and individuals are classified as morning, intermediate or evening type. Lower scores reflect stronger eveningness tendencies. Total score ranges from 16 to 86, with 16 to 41 being the eveningness type, 42 to 58 being the intermediate type, and 59 to 86 being the morningness type. Internal consistency was 0.60 in this study.
The ISI is a 7-item index developed by Bastien et al. [38] and assesses the severity of insomnia, satisfaction with current sleep, and worries about sleep problems during the last two weeks. The ISI total score ranges from 0 to 28, with higher scores reflecting higher severity of insomnia symptoms. A Korean version of the ISI has been validated in Korean samples [39]. The internal consistency was 0.83 in this sample.
The SGDS, developed by Yesavage and Sheikh [40], is a 15-item questionnaire that measures depressive symptoms in the elderly. Total scores range from 0 to 15 and higher scores reflect higher depression severity. The SGDS has previously been validated in Korean samples [41]. Internal consistency in this sample was 0.83.
A small subset of participants (n=8) completed a 7-day sleep diary, which consisted of standard sleep parameters such as bedtime (BT), sleep onset latency (SOL), rise time (RT) and wake after sleep onset (WASO).
Actigraphy measurements were obtained in a small subset of participants (n=8). Sleep-wake cycle, activity, and light exposure for 7 days were measured (Actiwatch2; Respironics, Murrysville, PA, USA). All times measured by the Actiwatch2 were recorded in 2-minute epochs and data was processed automatically by Philips Actiware 6.0.5 (Philips Healthcare, Bend, OR, USA) software program.
Characteristics of demographic and clinical variables were analyzed using descriptive statistics and Mann-Whitney U test. Pearson correlation analysis between MEQ, ISI, SGDS, STAI-S scores and MCTQ parameters were conducted for evaluating the validity of MCTQ. To establish convergent validity, Spearman correlation analysis was performed between MCTQ parameters (MSW, MSF, and MSFsc) and sleep diary and actigraphy parameters. Finally, receiver operating characteristic (ROC) curve analysis was conducted to propose a cut-off score for the MCTQ using MEQ scores. We used SPSS software version 21.0 (IBM Corp., Armonk, NY, USA) and MedCalc (MedCalc Software, Mariakerke, Belgium) for data analysis.
The mean age of participants was 72.31±4.58 (age range 65-88) years, with 75.1% (n=133) of the sample being female. We classified chronotype in our sample into either “morning” or “other” types using original MEQ criteria used in previous studies for the elderly [29,30,44]. This was based on recommendations by Monk and Buysse [45] indicating that eveningness tendencies were hardly reported in the elderly due to aging. Based on MEQ scores, there were 83.6% morning types (n=148) and 16.4% other types (n=29) in the current sample. There were no significant differences in gender, age groups, MMSE-DS total score, subjective health status, medical illness status, BMI, and depression between the chronotype groups. However, education years, MSFsc using MCTQ, insomnia, and anxiety were significantly higher scores in Other types compared to morning types (Table 1).
Distributions of MEQ, MSW, MSF, and MSFsc are shown in Figure 1. Pearson correlation analyses were conducted between MEQ scores and MCTQ parameters. MEQ scores were significantly negatively correlated with MCTQ parameters, MSF (r=-0.49, p<0.01) and MSFsc (r=-0.45, p<0.01), but not for MSW (r=-0.22, p=200). Results can be found in Table 2.
In a small group of participants (n=8), mid-sleep time on weekdays and free days (MSW, MSF), and MSFsc were calculated using sleep diaries and actigraphy. Results indicated that MCTQ parameters were correlated with MSFsc of sleep diaries and actigraphy parameters (rs=0.74, p<0.05 and rs=0.76, p<0.05, respectively). Results can be found in Figure 2.
Both MSF and MSFsc scores from the MCTQ were positively correlated with insomnia, depression, and anxiety. MSF was significantly correlated with ISI (r=0.27, p<0.01), SGDS (r=0.27, p<0.01), and STAI-S (r=0.23, p<0.01) scores. MSFsc using MCTQ was correlated with ISI (r=0.26, p<0.01), SGDS (r=0.25, p<0.01), and STAI-S (r=0.18, p<0.05) scores (Table 3).
Based on MEQ criteria, we conducted ROC curve analysis for MSF and MSFsc of the MCTQ to distinguish between morning type and other types in the elderly group. The area under the curve (AUC) of the MSF was 0.75 and the MSFsc was 0.76, indicating a reasonable level of accuracy [46].
The MSFsc with higher AUC was a more accurate parameter in this sample, but the difference of AUC between MSF and MSFsc was subtle. Thus, we used MSF and MSFsc in ROC analysis to suggest a cut-off score of the MCTQ for the elderly. The optimal score of MSF and MSFsc was 2.83, the Youden’s index of MSF was 0.44 (sensitivity=62.07%, specificity=82.43%), and the Youden’s index of MSFsc was 0.45, with 62.07% sensitivity and 83.11% specificity (Table 4).
In this study, we examined the psychometric properties of the MCTQ in Korean older adults and proposed cut-off scores for classifying chronotype in this population. The main results and implications of this study are as follows.
In our study, there was a high proportion of morning types in our sample. This is consistent with previous studies that show that while evening types are more common in younger adults, there is a larger proportion of morning types in the elderly as sleep patterns are advanced with aging [26,47,48]. Specifically, decreased sensitivity of the retina and weakening of the suprachiasmatic nucleus (SCN) lead to a decrease in light acceptance and changes in circadian rhythm [10,49,50], and as melatonin secretion and the amplitude of circadian rhythm decrease, many elderly report various sleep problems [11,51-53]. Because such changes in sleep caused by aging lead to advanced sleep time, Monk and Buysse [45]. suggested that it may be more appropriate to divide elderly populations into two groups, morning type and other types (intermediate/evening type).
Previous studies using MCTQ in the elderly reported that the MSFsc of 20-40 years old (young adult), was 4.42, while the MSFsc of 60 years over was advanced to 3.28 [25], and 3.17 [54]. The MSFsc in this study was 2.23, which was more advanced compared to previous studies. The difference of MSFsc in this study across studies compared to our sample may be due to the high proportion of females in our sample. Cain et al. [55] found that the time of body temperature and melatonin secretion was earlier in women than in men, indicating an earlier circadian rhythm in females compared to males.
Another aim of the study was to establish the validity of the MCTQ in an elderly sample. We verified a strong association between MCTQ parameters and MEQ scores, sleep diary and actigraphy parameters in Korean older adults. These results support convergent validity of the MCTQ and are consistent with previous studies [21,23,56]. Specifically, Zavada et al. [23] found that MEQ was negatively correlated with MSW and MSF, and Roenneberg et al. [26] also found similar results. However, in this study, the correlation between the MEQ and MSW was not significant in the MCTQ for Korean older adults, which may be explained by the small sample size of subjects (n=34) responding to the MCTQ’s weekdays items.
We also sought to evaluate construct validity of the MCTQ with insomnia, depression, and anxiety. Our results revealed that the participants who reported stronger eveningness tendencies had higher levels of insomnia, depression, and anxiety, which was consistent with previous studies [14-16,57,58]. Our results suggest that while there may be a smaller proportion of eveningness tendencies in older adults, eveningness tendencies are still important and indicative of sleep and psychological disturbance.
Finally, we proposed a cut-off score of the MCTQ in Korean older adults, yielding an MSFsc score of 2.83 as the optimal score in distinguishing between morning and other types in elderly samples. Only the MSFsc was significant in the correlation between MCTQ and objective measures (sleep diary and actigraphy) in this study. Therefore, it may be more desirable to use the MSFsc proposed by Roenneberg et al. [19] as a marker of the chronotype in the MCTQ for the elderly.
Our results indicate that other types (intermediate/evening) had more insomnia and anxiety than morning types. These results are similar to evening types in younger age groups in previous studies [16,19,58-60]. While our study categorized our sample into morning types and other types, this categorization is arbitrary as people fall on the spectrum of eveningness and morningness. Considering this continuum, our results suggest that some individuals grouped into other types in our study may have more eveningness tendencies than their counterparts of similar age, but display advanced sleep patterns due to sleep changes with aging. Although elderly participants with other types had a higher depression score than their counterparts with morning type, this difference was not statistically significant. This may be due to the fact that the current sample included the elderly who visit local community elderly centres. They engage in daily activities and have more social support, which may serve as a buffer against depression. Additionally, the sample size for other types was small. Taken together, our results suggest that the elderly group requires clinical interventions for other types (intermediate and evening) compared to morning types. Further studies should investigate whether being an intermediate and evening type may warrant interventions that are similar to evening types in younger age groups, as evening types are rare in elderly populations.
This study has several limitations. First, the sample sizes were small, especially in the comparison MCTQ with sleep diary and actigraphy parameters. Thus, it is necessary to increase the number of cases to validate the MCTQ with objective measures in future studies. Second, there was no biological measure for circadian rhythm in this study. Therefore, there is a need to use biological measure such as DLMO to measure more accurate circadian rhythms. Third, in this study, the proportion of elderly women was high and may have contributed to a high proportion of morningness type in this study.
Despite these limitations, this study validated the MCTQ in Korean older adults. In addition, we proposed a cut-off score for the MCTQ that distinguishes between morning type and other types in the elderly. Considering the small proportion of evening types in elder adults, it should be further investigated whether intermediate and evening types in older adults may warrant additional clinical attention.
ACKNOWLEDGEMENTS
This work was supported by the National Research Foundation of Korea(NRF) grant funded by the Korea government(MSIT) (NRF-2017R1C1B1008002).
Figure 1.
Distribution of MCTQ parameters and MEQ in a general sample of older adults. The Kolmogorov-Smirnov test was used to examine test of normality. (A) MEQ_total (63.90±6.59), (C) MSF (2.28±1.09), and (D) MSFsc (2.23±1.11) variables for 177 subjects who answered that they did not use the alarm on freedays and only 33 subjects who responded that they have a regular schedule on weekdays were analyzed in (B) MSW (2.53±0.75). Distributions were normal in all variables, (A) MEQ_total (Z=1.153, p=0.140), (B) MSW (Z=0.842, p=0.478), (C) MSF (Z=0.896, p=0.398), and (D) MSFsc (Z=1.067, p=0.205), respectively. MEQ: Morningness-Eveningness Questionnaire, MSW: mid-sleep on weekdays, MSF: mid-sleep on free days, MSFsc: midpoint of sleep on free days corrected for sleep debt accumulated through weekdays.

Figure 2.
Correlation between the MCTQ-derived mid-sleep time (MSFsc) with MSFsc parameters calculated from sleep diaries (black circles and solid line, N=8) and actigraphy (open circles and dotted line, N=8). Because of the small sample size, we used Spearman correlation, and there was a significant positive correlation between MSFsc in the MCTQ and MSFsc in the sleep diary and actigraphy (rs=0.74, p<0.05 and rs=0.76, p<0.05, respectively). MCTQ: Munich ChronoType Questionnaire, MSFsc: midpoint of sleep on free days corrected for sleep debt accumulated through weekdays.
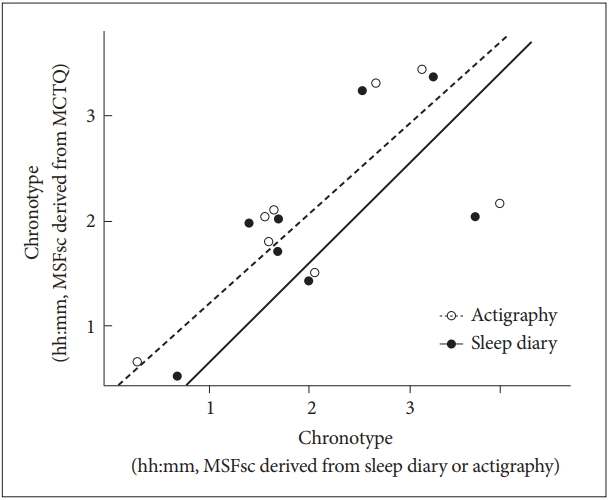
Table 1.
Demographic and clinical characteristics by chronotype (N=177)
| Morning type (N=148) | Other types (N=29) | χ2/ Z | |
|---|---|---|---|
| N (%) / mean±SD | N (%) / mean±SD | ||
| Gender (Male) | 40 (22.6) | 4 (2.3) | 2.274 |
| Age (years) | 72.39±4.36 | 71.86±5.64 | -1.097 |
| 65-75 years | 99 (55.9) | 22 (12.4) | 0.902 |
| 75 years over | 49 (27.7) | 7 (4.0) | |
| MMSE-DS | 26.77±2.32 | 27.39±2.41 | -1.582 |
| Education (years) | 9.21±4.55 | 11.20±3.86 | -2.339* |
| Subjective health status | 2.58±0.98 | 2.72 ±0.79 | -0.897 |
| Medical illness status | |||
| Yes | 115 (65.7) | 25 (14.3) | 0.837 |
| No | 31 (17.7) | 4 (2.3) | |
| BMI | 23.33±2.79 | 23.03±2.77 | -0.459 |
| MSFsc | 2.08±1.03 | 2.96±1.21 | -4.335† |
| ISI | 5.82±5.02 | 8.93±4.60 | -3.474* |
| SGDS | 3.21±3.23 | 3.89±3.39 | -1.214 |
| STAI-S | 32.69±9.48 | 36.06±8.89 | -2.246* |
Table 2.
Correlation between MEQ scores and MCTQ parameters (N=177)
| MEQ | MSW | MSF | MSFsc | |
|---|---|---|---|---|
| MEQ | 1 | |||
| MSW | -0.229 | 1 | ||
| MSF | -0.495* | 0.758* | 1 | |
| MSFsc | -0.451* | 0.814* | 0.955* | 1 |
Table 3.
Associations between MCTQ parameters and variables (N=177)
| MSW | MSF | MSFsc | ISI | SGDS | STAI-S | |
|---|---|---|---|---|---|---|
| MSW | 1 | |||||
| MSF | 0.758† | 1 | ||||
| MSFsc | 0.814† | 0.828† | 1 | |||
| ISI | 0.088 | 0.271† | 0.261† | 1 | ||
| SGDS | -0.288 | 0.272† | 0.252† | 0.337† | 1 | |
| STAI-S | -0.200 | 0.237† | 0.187* | 0.491† | 0.692† | 1 |
|
|
||||||
| M | 2.53 | 2.28 | 2.23 | 6.33 | 3.32 | 33.25 |
| (SD) | 0.75 | 1.09 | 1.11 | 5.08 | 3.26 | 9.44 |
Table 4.
Sensitivity and specificity of MSFsc in Korean older adults based on MEQ cut-offs
REFERENCES
1. The annual average growth rate per 100,000 people with sleep disorder is the highest in their 30s. Available at: http://www.nhis.or.kr/bbs7/boards/B0039/15234?boardKey=14&sort=sequence&order=desc&rows=10&messageCategoryKey=&pageNumber=1&viewType=generic&targetType=12&targetKey=14&status=&period=&startdt=&enddt=&queryField=&query=. Accessed October 5, 2015.
2. Ancoli-Israel S. Sleep and its disorders in aging populations. Sleep Med 2009;10(Suppl 1):S7-S11.


3. Curran H, Collins R, Fletcher S, Kee S, Woods B, Iliffe S. Older adults and withdrawal from benzodiazepine hypnotics in general practice: effects on cognitive function, sleep, mood and quality of life. Psychol Med 2003;33:1223-1237.


4. Foley DJ, Ancoli-Israel S, Britz P, Walsh J. Sleep disturbances and chronic disease in older adults: results of the 2003 National Sleep Foundation Sleep in America Survey. J Psychosom Res 2004;56:497-502.


5. Taylor DJ, Mallory LJ, Lichstein KL, Durrence H, Riedel BW, Bush AJ. Comorbidity of chronic insomnia with medical problems. Sleep 2007;30:213-218.



6. Vitiello MV. Sleep disorders and aging: understanding the causes. J Gerontol A Biol Sci Med Sci 1997;52:M189-M191.



7. Wolkove N, Elkholy O, Baltzan M, Palayew M. Sleep and aging: 1. Sleep disorders commonly found in older people. CMAJ 2007;176:1299-1304.



9. Kim SJ, Lee YJ, Kim H, Cho IH, Lee JY, Cho SJ. Age as a moderator of the association between depressive symptoms and morningness-eveningness. J Psychosom Res 2010;68:159-164.


10. Sok SR, Choi JY. Factors influencing sleep of elderly women. J Korean Acad Nurs 2010;40:119-126.


11. Cooke JR, Ancoli-Israel S. Normal and abnormal sleep in the elderly. Hand Clin Neurol 2011;98:653-665.

12. Levandovski R, Dantas G, Fernandes LC, Caumo W, Torres I, Roenneberg T, et al. Depression scores associate with chronotype and social jetlag in a rural population. Chronobiol Int 2011;28:771-778.


13. Chelminski I, Ferraro FR, Petros TV, Plaud JJ. An analysis of the “eveningness-morningness” dimension in “depressive” college students. J Affect Disord 1999;52:19-29.


14. Boivin DB. Influence of sleep-wake and circadian rhythm disturbances in psychiatric disorders. J Psychiatry Neurosci 2000;25:446-458.


15. Hidalgo MP, Caumo W, Posser M, Coccaro SB, Camozzato AL, Chaves MLF. Relationship between depressive mood and chronotype in healthy subjects. Psychiatry Clin Neurosci 2009;63:283-290.


16. Díaz-Morales JF, Sanchez-Lopez MP. Morningness-eveningness and anxiety among adults: a matter of sex/gender? Pers Individ Dif 2008;44:1391-1401.

17. Hofstra WA, de Weerd AW. How to assess circadian rhythm in humans: a review of literature. Epilepsy Behav 2008;13:438-444.


18. Horne JA, Ostberg O. A self-assessment questionnaire to determine morningness-eveningness in human circadian rhythms. Int J Chronobiol 1975;4:97-110.
19. Roenneberg T, Wirz-Justice A, Merrow M. Life between clocks: daily temporal patterns of human chronotypes. J Biol Rhythms 2003;18:80-90.


20. Burgess HJ, Savic N, Sletten T, Roach G, Gilbert SS, Dawson D. The relationship between the dim light melatonin onset and sleep on a regular schedule in young healthy adults. Behav Sleep Med 2003;1:102-114.


21. Kitamura S, Hida A, Aritake S, Higuchi S, Enomoto M, Kato M, et al. Validity of the Japanese version of the Munich ChronoType Questionnaire. Chronobiol Int 2014;31:845-850.


23. Zavada A, Gordijn MC, Beersma DG, Daan S, Roenneberg T. Comparison of the Munich Chronotype Questionnaire with the Horne-Östberg’s morningness-eveningness score. Chronobiol Int 2005;22:267-278.


24. Kantermann T, Sung H, Burgess HJ. Comparing the morningnesseveningness questionnaire and munich chronotype questionnaire to the dim light melatonin onset. J Biol Rhythms 2015;30:449-453.



25. Wittmann M, Dinich J, Merrow M, Roenneberg T. Social jetlag: misalignment of biological and social time. Chronobiol Int 2006;23:497-509.


26. Roenneberg T, Kuehnle T, Juda M, Kantermann T, Allebrandt K, Gordijn M, et al. Epidemiology of the human circadian clock. Sleep Med Rev 2007;11:429-438.


27. Costa G, Lievore F, Ferrari P, Gaffuri E. Usual meal times in relation to age, sex, work activity and morningness-eveningness. Chronobiologia 1986;14:383-391.
28. Ishihara K, Miyake S, Miyasita A, Miyata Y. Morningness-eveningness preference and sleep habits in Japanese office workers of different ages. Chronobiologia 1991;19:9-16.
29. Biss RK, Hasher L. Happy as a lark: morning-type younger and older adults are higher in positive affect. Emotion 2012;12:437-441.




30. Senol V, Soyuer F, Nar Senol P. Assessment of sleep quality with pittsburgh, epworth and morningness eveningness questionnaire scales in the elderly at nursing home. Turk J Geriatr 2013;16:60-68.
31. Taillard J, Philip P, Chastang JF, Bioulac B. Validation of Horne and Ostberg morningness-eveningness questionnaire in a middle-aged population of French workers. J Biol Rhythms 2004;19:76-86.


32. Kühnle T. Quantitative analysis of human chronotypes. Available at: https://edoc.ub.uni-muenchen.de/5168/1/Kuehnle_Tim.pdf.
33. Roenneberg T, Keller LK, Fischer D, Matera JL, Vetter C, Winnebeck EC. Human activity and rest in situ. Methods Enzymol 2015;552:257-283.


34. Kuehnle T, Juda M, Kantermann T, Allebrandt K, Gordijn M, et al. Epidemiology of the human circadian clock. Sleep Med Rev 2007;11:429-438.


35. Suh S, Kim SH, Ryu H, Choi SJ, Joo EY, et al. Validation of the Korean Munich Chronotype Questionnaire. Sleep Breath doi: 10.1007/s11325-017-1609-z. [Epub ahead of print].


36. Suh S, Kim SH, Ryu H, Choi SJ, Joo EY, et al. Validation of the Korean Munich Chronotype Questionnaire. Sleep and Breathing 2018;1-7. doi: 10.1007/s11325-017-1609-z. [Epub ahead of print].



37. Yu NJ, Shin SC, Wang SK. A study on the standardization of the Korean version of JA Horne and O. Ostbergs’ Morningness-Eveningness Questionnaire and on the sleep pattern. J Korean Neuropsychiatr Assoc 1995;34:642-656.
38. Bastien CH, Vallieres A, Morin CM. Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med 2001;2:297-307.


39. Cho YW, Song ML, Morin CM. Validation of a Korean version of the insomnia severity index. J Clin Neurol 2014;10:210-215.



40. Yesavage JA, Sheikh JI. Geriatric depression scale (GDS) recent evidence and development of a shorter version. Clin Gerontol 1986;5:165-173.

41. Kee BS. A preliminary study for the standardization of geriatric depression scale short form-Korea version. J Korean Neuropsychiatr Assoc 1996;35:298-307.
42. Spielberger CD, Gorsuch RL, Lushene RE. Manual for the State-Trait Anxiety Inventory. Palo Alto: Consulting Psychologists Press; 1970.
43. Kim J, Shin D. A study based on the standardization of the STAI for Korea. New Med J 1978;21:69-75.
44. Carciofo R, Du F, Song N, Qi Y, Zhang K. Age-related chronotype differences in Chinese, and reliability assessment of a reduced version of the Chinese Morningness-Eveningness Questionnaire. Sleep Biol Rhythms 2012;10:310-318.

45. Monk TH, Buysse DJ. Chronotype, bed timing and total sleep time in seniors. Chronobiol Int 2014;31:655-659.



46. Muller MP, Tomlinson G, Marrie TJ, Tang P, McGeer A, Low DE, et al. Can routine laboratory tests discriminate between severe acute respiratory syndrome and other causes of community-acquired pneumonia? Clin Infect Dis 2005;40:1079-1086.



47. Duffy JF, Czeisler CA. Age-related change in the relationship between circadian period, circadian phase, and diurnal preference in humans. Neurosci Lett 2002;318:117-120.


48. Gaspar-Barba E, Calati R, Cruz-Fuentes CS, Ontiveros-Uribe MP, Natale V, De Ronchi D, et al. Depressive symptomatology is influenced by chronotypes. J Affect Disord 2009;119:100-106.


49. Bliwise D. Sleep and circadian rhythm disorders in aging and dementia. Lung Biol Health Disease 1999;133:487-525.
50. Farajnia S, Michel S, Deboer T, Tjebbe vanderLeest H, Houben T, Rohling JH, et al. Evidence for neuronal desynchrony in the aged suprachiasmatic nucleus clock. J Neurosci 2012;32:5891-5899.



51. Van Coevorden A, Mockel J, Laurent E, Kerkhofs M, L’Hermite-Baleriaux M, Decoster C, et al. Neuroendocrine rhythms and sleep in aging men. Am J Physiol 1991;260:E651-E661.


53. Myers BL, Badia P. Changes in circadian rhythms and sleep quality with aging: mechanisms and interventions. Neurosci Biobehav Rev 1996;19:553-571.

54. Giménez M, Beersma D, Daan S, Pol Bvd, Kanis M, van Norren D, et al. Melatonin and sleep-wake rhythms before and after ocular lens replacement in elderly humans. Biology (Basel) 2016;5:pii: E12.

55. Cain SW, Dennison CF, Zeitzer JM, Guzik AM, Khalsa SBS, Santhi N, et al. Sex differences in phase angle of entrainment and melatonin amplitude in humans. J Biol Rhythms 2010;25:288-296.



56. Roenneberg T, Merrow M. Entrainment of the human circadi an clock. Cold Spring Harb Symp Quant Biol 2007;72:293-299.


57. Chan J, Lam SP, Li SX, Yu M, Chan NY, Zhang J, et al. Eveningness and insomnia: independent risk factors of nonremission in major depressive disorder. Sleep 2014;37:911-917.




58. Ong JC, Huang JS, Kuo TF, Manber R. Characteristics of insomniacs with self-reported morning and evening chronotypes. J Clin Sleep Med 2007;3:289-294.









