Avoidant Insecure Attachment as a Predictive Factor for Psychological Distress in Patients with Early Breast Cancer: A Preliminary 1-Year Follow-Up Study
Article information
Abstract
Objective
To identify attachment insecurity as an associative factor with unresolved psychological distress 1 year after surgery in the early breast cancer (BC) population.
Methods
One-hundred fourteen participants completed the Hospital Anxiety and Depression Scale (HADS) and the Experiences in Close Relationship (ECR-M36) questionnaire within 1 week (baseline) and at 1-year post-surgery (follow-up). Participants were categorized into the distress and the non-distress groups based on a HADS-total score cut-off of 15. Logistic regression analysis revealed predictive factors of distress at follow-up.
Results
At baseline, 53 (46.5%) participants were found to be in the distress group. The degree of distress decreased over 1 year (p= 0.003); however, 43 (37.7%) showed significant remaining distress at follow-up. Baseline scores of the ECR-M36 avoidance [odds ratio (OR)=1.045, 95% confidence interval (CI)=1.002–1.090] and HADS-total (OR=1.138, 95% CI=1.043–1.241) were predictors of distress at follow-up.
Conclusion
A substantial proportion of early BC patients suffer distress even one-year after surgery. Avoidant attachment appeared to be an influential factor on distress in early BC patients. Moreover, the finding that initial distress level could predict one at 1-year post-operation warrant a screening and management of distress along with BC treatment.
INTRODUCTION
In struggling with breast cancer (BC), patients suffer from related adversities such as physical injury, deformity and pain (e.g., due to amputation or disfigurement of the breast, skin changes, hair loss, and lymphedema), role changes in the family and as occupational or social members, uncertainty, and existential crises [1]. In the face of these challenges, the unpleasant emotions experienced by individuals are conceptualized as ‘distress’ [2]. Distress is associated with treatment compliance and quality of life in BC patients [3,4].
The level of distress in BC patients is known to decrease with the trajectory of the cancer experience [5-8]. Despite the high degree of distress at the beginning of BC treatment, it generally decreases and stabilizes after 4 to 12 months [9,10]. However, Lam et al. [10] reported that 15.4% of patients who had undergone BC surgery continued to experience chronic distress even 8 months after the operation. Hence, cancer professionals need to address the possibility that distress early in BC treatment may indicate an enduring pathological emotional problem. We propose that the quality and outcomes of BC treatment would be improved by screening patients for chronic distress and intensively managing them from the initial stage of BC treatment.
Attachment theory could provide a useful theoretical and clinical frame to identify the nature of distress in BC patients [11-14]. Attachment theory was formed as a socioemotional developmental perspective that emphasizes the early infant-caregiver relationship within an evolutionary-ethological context of adaption and species survival [13]. Recent attachment theory has been extended in its conceptual territories to include psychopathology, affect regulation, interpersonal relationships and stress responses in adulthood as well as childhood [15,16]. Pioneering attempts have been made to establish attachment theory as a conceptual frame in which to identify the psychological aspects of cancer [12-14,17].
An infant establishes physiological, cognitive, and emotional responses as well as their processing strategies as a specific biobehavioral pattern when confronting attachment-related events (e.g., loss, abuse) [15]. The pattern is internalized as an inner resource and re-activated when confronting life adversities, such as stress or illness, in adulthood. When faced with life adversities, a person with an insecure (anxious or avoidant) attachment style is more likely than one with secure attachment to suffer from loneliness, negative affect, shame, anger, fear of negative evaluation, pathological narcissism, and emotional dysregulation [18-20]. In this way, a patient’s attachment system may be re-activated and displayed with emotional difficulty (distress) when diagnosed or treated for BC. There have been limited studies of attachment security issues in the BC population from the perspectives of quality of life [19,21], coping strategies [17,19], rapport or relationship with the surgeon and the patient’s family [22,23], immune response [24], and screening behavior [25]. However, little research has addressed the relationship of attachment insecurity with psychological distress.
This study’s aim is to identify the factors present at the initial BC treatment stage that are associated with unresolved distress at the 1-year follow-up after BC surgery, including the factor of attachment insecurity. Additionally, we investigate and compare the levels of distress at two assessment points: within 1 week after the cancer surgery and at the 1-year postsurgery follow-up.
METHODS
Participants
Newly diagnosed BC patients from Kyungpook National University Hospital (KNUH) and Kyungpook National University Medical Center (KNUMC) were approached after breast surgery, between January 2012 and June 2014. KNUH and KNUMC are the largest general hospitals in Daegu, South Korea and are referral centers for other provinces. First, the purpose and procedure of this study were explained to BC patients. Among those who agreed to participate in the study, subjects were included if they met the following criteria: female, between 18 and 80 years of age, diagnosed with early BC (TNM stage 0–II), no previous history of BC, no chemotherapy before surgery, no evidence of distant metastasis, no other significant medical or psychiatric morbidity, no past history of psychiatric illnesses, and the ability to read and write Korean. Written informed consent was obtained from all participants after a full explanation of the study. The first interview was performed during hospitalization within 7 days after the BC surgery. Follow-up was performed 1 year after the first interview. Sociodemographic information on age, marital status, education, socioeconomic status, religion, and employment was obtained via a questionnaire. Clinical data consisting of disease stage, type of breast surgery, and hormone therapy were extracted from the patients’ medical records. This study was approved by the Institutional Review Board of KNUH (KNUH IRB file no. 2012-05-008-007).
Procedures
Participants completed the Hospital Anxiety and Depression Scale (HADS) and Experiences in Close Relationship (ECR-M36) survey within 1 week after cancer surgery (baseline) and at a 1-year later (follow-up).
Hospital Anxiety and Depression Scale
The HADS comprises of a 7-item anxiety subscale (HADSA) and a 7-item depression subscale (HADS-D). Each item is rated on a 4-point Likert scale (0=not at all to 3=very much); the subscale scores range from 0 to 21, and the total scores (HADS-T) range from 0 to 42 (HADS-T) [26]. Some researchers believe that the HADS is not appropriate for discrimination of anxiety versus depression because it has a very powerful general distress factor [27]. In the oncological setting, the screening ability of HADS-T seems to be similar to that of HADS-A or HADS-D. HADS-T has been widely used as a distress-screening tool [28-30].
In the present study, we used HADS-T as a distress-screening tool with a cut-off point of 14/15 points [29,31]. The Korean version of the HADS has shown good internal consistency [26].
Modified Experiences in Close Relationships (ECR-M36)
The ECR-M36 is a modified version of the original ECR questionnaire, aimed to assess psychological attachment to other persons, rather than only attachment to romantic partners as in the original version [32]. The ECR-M36 was developed for the purpose of measuring attachment security in medically ill patients [33].
The ECR-M36 consists of 36 items with two independent dimensions, attachment anxiety (even numbered items) and attachment avoidance (odd numbered items). Each item is rated on a 7-point Likert scale ranging from 1 (strongly disagree) to 7 (strongly agree); the subscores range from 18 to 126 for each attachment style and the total scores range from 36 to 252. Higher scores on the ECR-M36 indicate greater degrees of insecure attachment (anxiety or avoidance). The Korean version of the ECR-M36 was developed for patients with BC and has shown satisfactory reliability, validity, and factor structure [33].
Analysis
We performed a paired t-test to compare the mean scores on the HADS-T and ECR-M36 (total score, anxiety subscore, and avoidance subscore) between the two assessment time points for all participants.
At both baseline and follow-up, we assigned patients with HADS-T scores of 15 or greater to the distress group and those with lower scores the non-distress group.
We conducted logistic regression analysis to determine the predictors at baseline of distress at follow-up. In pursuit of the model with the best fit to predict psychological distress at follow-up, we inserted into the models sociodemographic (age, marital status, education, socioeconomic status, religion, and employment), cancer-related (cancer stage, type of surgery, and endocrine therapy), and psychological-personal (ECR-M36 anxiety, ECR-M36 avoidance, ECR-M36 total, and HADS-T score) variables at baseline with forward selection as potential explanatory variables in the logistic regression analysis. We analyzed data using PASW Statistics version 24.0 for Windows (IBM Co., Armonk, NY, USA).
RESULTS
Participant characteristics
At baseline, 169 patients participated in this study. Of those, the 114 (58.2%) patients who also participated at follow-up were the final study sample. The sociodemographic and clinical data of the participants are given in Table 1. The average age of the BC survivors was 47.3 (SD=9.5) years with a range of 29 to 72 years.
Scores on the HADS-T and ECR-M36 and their changes over the 1 year post-surgery
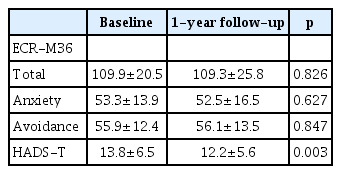
Table 2 provides the results of the paired t-tests on attachment security and HADS-T scores between the two assessment points. There was no significant change in attachment security, including the anxiety and avoidance subscales, between baseline and follow-up. However, the HADS-T scores decreased significantly.
Levels of psychological distress and its changes over the 1 year post-surgery
At baseline, 53 (46.5%) of the patients were significantly distressed, and of these, 31 (58.5%) remained in the distress group at follow-up. Of the 61 patients (19.1%) in the non-distress group at baseline, 12 developed psychological distress after 1 year. At follow-up, 43 out of 114 subjects (37.7%) exhibited psychological distress. The presence of distress at baseline was significantly associated with the presence of distress at follow-up (p<0.001) (Table 3).
Factors at baseline associated with psychological distress at the 1-year follow-up
The analysis showed that ECR-M36 avoidance and HADS-T at baseline were significant predictors of distress at follow-up. The other investigated sociodemographic and cancer-related variables were not found to be significant (Table 4).
DISCUSSION
This study found that 46.5% of the patients treated with surgery for early BC were psychologically distressed when assessed within 1 week after BC surgery (baseline). Consistent with other studies [5-8], the degree of psychological distress in these patients with early BC decreased significantly during the year after cancer surgery (Table 2). However, a substantial number of patients (n=43, 37.7%) in the present study exhibited psychological distress at the 1-year point after BC surgery (follow-up). These findings support the legitimacy of the American Society of Clinical Oncology (ASCO)’s recommendations that all cancer patients should be screened for emotional suffering beginning at their initial visit and at appropriate intervals [34].
Interpersonal relationships and emotional regulation have emerged as important distress research issues in the field of psycho-oncology [11]. Accumulated neuroscientific research has extended John Bowlby’s foundational concept of attachment into applications in the emotional regulation system [16]. Physical injury and role change experienced by BC patients can be considered to be attachment-related events (i.e., loss, separation, threat, isolation or dependency) [14,15]. Therefore, we expect that the concept of distress can be elaborated by employing attachment theory.
The present study found that early BC patients with higher ECR-M36 avoidance scores at baseline were more likely to be classified in the distress group at follow-up. Faced with illness, people with avoidant attachment styles may display deactivating strategies: not actively seeking medical help, denying attachment needs, and avoiding interdependence in relationships. Avoidant attachment strategies are sculptured in early infant-caregiver relationships that do not provide closeness or meet expressions of need [18,35]. People with an avoidant attachment style appear to be self-reliant by attempting to repress their negative emotions, but in practice, this attempt impairs the regulation of stress physiology [12,14]. Tacón et al. [12] speculated about the contribution of avoidant attachment style to emotional distress in the BC population from the perspective of neuroimmunology, interpersonal relationships and emotional regulation. Another study reported that avoidant attachment, which interacted with respiratory sinus arrhythmia (RSA), predicted quality of life in BC survivors [21]. These findings have clinical implications for managing BC patients with avoidant attachment styles. Such patients have been found to show disturbed hypothalamic-pituitary-adrenocortical (HPA) stress-regulating axis, autonomic nervous system (ANS), and immune function [13,14,36]. Therefore, psychotropic drugs like antidepressants, benzodiazepins, or corticotrophin-releasing factors, which can modulate the HPA axis, ANS, or immune system, are promising for reducing physiological distress levels [14]. In addition, patients with avoidant attachment are likely to feel unsupported or rejected by cancer professionals because of their inner working models that emphasize the threatening and untrustworthy nature of significant others and the importance of maintaining distance from attachment figures [18,22]. Considering the specific interpersonal relationships in patient with avoidant attachment, behavioral approaches performed by reliable oncologists or psycho-oncologists that respect interpersonal distance and enhance perceived personal control could strengthen cancer treatment adherence [14,16].
A number of studies have been conducted to determine the factors associated with distress in BC patients. The factors identified through the research have been diverse and can be classified as follows [11,37-39]: sociodemographic factors (e.g., age, marital status, education, socioeconomic status, social support, and past history of psychological treatment); cancer-related factors (e.g., cancer stage, type of surgery, endocrine therapy, and chemotherapy); physical/physiological factors (e.g., fatigue, pain, physical symptoms, insomnia, and menopausal syndrome); and psychological and personal factors (e.g., personality, coping strategy, and self-esteem). According to two recent systematic reviews, the main predictors can be summarized as younger age, low socio-economic status (SES), previous psychiatric history, advanced-stage diagnosis, fatigue, and pain [11,37].
This study found that HADS-T [β=0.129, odds ratio (OR)=1.138] at baseline was also predictive factors of distress at follow-up (Table 4). We emphasize that these results were derived from a population of patients with early BC who had no previous psychiatric history. Only 7.0% (n=8) of the participants in this study were categorized as having low SES (Table 1). When comparing our findings with those of other studies, the characteristics of the present study should be taken into account.
The level of distress at baseline was significantly associated with that at follow-up (Tables 3 and 4). These results are in agreement with earlier findings that psychological sufferings during the initial stage of treatment can predict continued suffering after one [9,40] or six years [41]. Unlike uncorrectable variables (e.g., age, psychiatric history and SES), emotional difficulties can be improved through psychological or psychiatric intervention. Therefore, screening and management of distress should be conducted from the start of cancer treatment.
Other variables such as age and cancer stage, were not found to be significantly associated with distress at follow-up.
Young BC patients are apt to experience rapid physical or social changes such as anticancer-treatment induced infertility, withdrawal from childrearing, and interruption to occupational career. Moreover, younger BC patients are usually submitted to more aggressive cancer treatment [11,40,42]. For these reasons, younger age has been viewed as a risk factors for emotional distress. However, older patients may be less able to cope with physical and cognitive changes caused by cancer or anticancer treatment [43]. Younger patients may better adapt to the physical or social changes despite severe emotional turmoil at the initial stage of the cancer trajectory. Brandao et al. [11] pointed out in their recent systematic review that younger age is not consistently documented as a risk factor for distress.
Advanced BC diagnosis, compared to early BC, is connected with more aggressive cancer treatment, worse physical conditions, and worse prognosis and is associated with greater levels of distress [37]. However, many studies of early BC have found that cancer-related variables were not associated with psychological distress [4,7,38]. Apart from cancer or cancer treatment-related factors, psychological/personal or physical/physiological factors like optimsm [38], availability of support system [7,11], copying strategies [11,41], fatigue and pain [6,11,37,40] are known to be more critical in the adaptation to cancer.
This study has several limitations. First, only a small cohort of BC patients participated in this study. Second, we did not consider the effects of other cancer treatments or psychiatric interventions that could aggravate or abate the level of distress during the year after surgery. Third, more extensive factors such as other physical-psychological (e.g., fatigue, pain) or psychological (e.g., personality, temperament) variables should be investigated in future research to confirm the impact of attachment style on distress in the BC population. Nevertheless, the current study provides preliminary research that highlights the promising role of attachment theory in elaborating the concept of distress.
In summary, the present study demonstrates that a substantial proportion of patients with BC surgery continued to suffer from psychological distress even 1 year after surgery. Avoidant attachment style appeared to be an influential factor of distress in early BC patients. Moreover, the finding that the level of distress at the initial stage of treatment can predict emotional difficulties 1 year after surgery warrants routine screening and management of distress along with BC treatment. Future studies should be conducted to clarify the nature of distress in the context of attachment systems with multifactorial variables (e.g., physiological markers, mediating factors) in large-scale BC population studies.