 |
 |
- Search
| Psychiatry Investig > Volume 11(3); 2014 > Article |
Abstract
Objective
Previous studies have reported comorbidity of attention deficit and hyperactivity disorder (ADHD) and allergic diseases. The current study investigated ADHD like behavioral symptoms and parenting stress in pediatric allergic rhinitis.
Methods
Eighty-seven children (6-13 years old) with allergic rhinitis and 73 age- and sex-matched children of control group were recruited. Diagnosis and severity assessments of allergic rhinitis were determined by a pediatric allergist. The Parenting Stress Index-Short Form (PSI-SF), ADHD Rating Scale (ARS), and Child Behavior Checklist (CBCL) were completed by their mothers.
Results
In the allergic rhinitis group, the total PSI-SF score (p<0.01), ARS score (p<0.01), the subscale scores of the CBCL including somatization, attentional problems and emotional instability (p=0.01; p<0.01; p<0.01) and prevalence of ADHD (p=0.03) were significantly higher than those of the control group. Among mothers of children with allergic rhinitis, those of children with comorbid ADHD demonstrated significantly higher parenting stress than those without comorbid ADHD (p<0.01). Parenting stress was correlated with severity of child's allergic symptoms and the ARS total score (beta=0.50, p<0.01; beta=0.39, p<0.01). There was a significant correlation between allergic symptom severity and the ARS total score (B=8.4, SD=2.5, t=3.3, p<0.01).
Conclusion
This study demonstrated that ADHD symptoms were common in children with allergic rhinitis, and this factor increased parenting stress and disrupted the parent-child relationship. Routine evaluation and early management of ADHD symptoms in pediatric allergic rhinitis may benefit families of children with allergic rhinitis.
Parents' stress and coping strategies in response to their child's chronic illnesses may modulate the child's clinical symptoms, behavioral characteristics and quality of life.1,2 Of several chronic medical diseases, allergic diseases have been thought to be closely associated with parenting stress and the relationships between mothers and their children.3,4 Mothers of children with allergic diseases are more anxious, psychologically unstable, overprotective, and often demonstrate negative emotions toward their children.5,6 There are significant correlations between a caregiver's quality of life and the severity of children's allergic symptoms and with the quality of life of the child.7,8
Allergic diseases, including atopic dermatitis, allergic rhinitis and asthma, progress under the allergic march. Prevalence and symptoms of allergic diseases differ by age.9 Atopic dermatitis usually emerges within the first two years of life, and half of children with atopic dermatitis tend to have allergic rhinitis or asthma later in life.10 Allergic rhinitis is most prevalent during elementary school and affects children's daily lives.11 Prevalence of global childhood allergic rhinitis has been reported to be as high as 39.7%.12 Although the methods for preventing and treating allergic diseases have progressed, the prevalence of allergic rhinitis has increased over the last several decades and is expected to continue to increase due to environmental influences.13,14
It is interesting that the age of incidence of allergic rhinitis is similar to that of ADHD.15,16 Symptoms of allergic rhinitis (sneezing, pruritus, nasal congestion and rhinorrhea) disturb daily activities and sleep patterns. This can lead to daytime inattention, irritability and hyperactivity. These behaviors are also frequently observed in children with ADHD.17
ADHD is the most common worldwide neurodevelopmental disorder. Depending on the diagnostic criteria used, the prevalence rate of ADHD in children ranges from 2% to 10%.18 Its primary symptoms are inattention, hyperactivity and impulsive behavior.19 Parents of ADHD children report high parenting stress due to their children's maladaptive behaviors and disruptions in the parent-child relationship.20,21,22 Stressful parenting may contribute to the aggravation of clinical symptoms, confounding problems for children with ADHD.23
Worldwide, the increasing prevalence rate of allergic disease parallels the increasing prevalence of ADHD.10
Several clinical studies have investigated the co-existence of allergic diseases and ADHD. ADHD symptoms among children with allergic diseases including allergic rhinitis and atopic dermatitis have been reported.24,25 Conversely, allergic symptoms in children with ADHD have also been reported.17,26 However, previous studies have been limited in the methods used to diagnose ADHD or in selecting the controlled comparison group.
Among pediatric allergic diseases, high levels of parenting stress have been reported in association with asthma and atopic dermatitis.27,28 However, to the best of our knowledge, there have been few studies examining allergic rhinitis and parenting stress. Accordingly, we investigated ADHD behavioral problems in children with allergic rhinitis and their effect on parenting stress.
Eighty seven children (38 boys and 49 girls) aged 6 to 13 years with allergic rhinitis were recruited from an outpatient pediatric clinic of Chung-Ang University Hospital in Seoul. Seventy three age- and sex-matched children (25 boys and 48 girls) of control group were randomly selected (Table 1). Inclusion criteria were based on a diagnosis determined by a pediatric allergist. For the allergic rhinitis group, children had a diagnosis of allergic rhinitis. For the control group, children had no allergic symptoms or history of allergic disease including allergic rhinitis, asthma or atopic dermatitis. Exclusion criterion was any developmental disorder including mental retardation, physical illness or mental disorder other than ADHD.
The Parenting Stress Index-Short Form (PSI-SF) measures parenting stress, general parent distress and parental ratings of child adjustment.29,30 The PSI-SF consists of 36 items using a five-point response scale and three subscales: parental distress, parent-child dysfunctional interaction and child difficulty. We used a standardized Korean version of the PSI-SF, which has demonstrated high validity and reliability.31
The Child Behavior Checklist (CBCL) consists of 119 items that assess a child's behavioral problems over the previous six months. Parents respond using a three-point scale. This measure is composed of 12 subscales assessing the following domains: withdrawal, somatic complaints, anxiety/depression, social problems, thought problems, attentional problems, delinquent behavior, aggressive behavior, internalizing symptoms, externalizing symptoms and emotional instability. We used the Korean version of the CBCL. This scale has demonstrated good reliability and discriminative validity in a crosscultural population.32,33
The ADHD Rating Scale (ARS) consists of 18 items: nine inattention items and nine hyperactive/impulsivity items, based on DSM-IV criteria of ADHD.34 Parents responded using a four-point scale ranging from 0 to 3 points. The ARS provides a total score and subscale scores for inattention and hyperactivity/impulsivity. The Korean version of the ARS has demonstrated high validity and reliability in assessing ADHD.35,36
The Comprehensive Attention Test (CAT) is a computerized continuous performance test to assess attention and the ability to control impulsivity and it has been used as a reliable and valid tool for evaluating ADHD symptoms in children and adolescents. The CAT consists of the selective attention task of auditory attention and visual attention, the sustained attention to response task, the flanker task, the divided attention task, and the spatial working memory task. The results of the CAT consists of T scores for omission errors (reflecting inattention), commission errors (reflecting impulsivity), response time (reflecting speed of information processing and motor response), and variability of response time (reflecting consistency of attention).37 The reported mean of the correlation coefficient for test-retest scores is 0.715.37
Informed consent from children and their mothers was obtained in accordance with local Institutional Review Board guidelines. Severity of allergic rhinitis was assessed by a pediatric allergist using the Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines.38 Based on the frequency and intensity of allergic rhinitis symptoms, severity level was used to classify the patients into four groups: intermittent and mild, intermittent and moderate-severe, persistent and mild, and persistent and moderate-severe.
Mothers of participated children completed the PSI-SF, CBCL and ARS. In cases where the ARS score was greater than 16 points suggesting the probable ADHD,39 children completed the CAT, and children and their mothers completed a psychiatric structured interview to evaluate ADHD like symptoms based on criteria of the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV).40
An independent t-test was used to assess group differences across measures between the allergic rhinitis and URI groups. A Chi-square test was used to analyze the difference in ADHD prevalence between the two groups. A one-way analysis of variance (ANOVA) was used to compare group differences in PSI-SF and CBCL scores. A Pearson correlation was used to assess the relationships between allergic rhinitis symptoms and PSI-SF and ARS scores. All results were considered statistically significant at a p-value<0.05. All analyses were performed using SPSS 11.0.
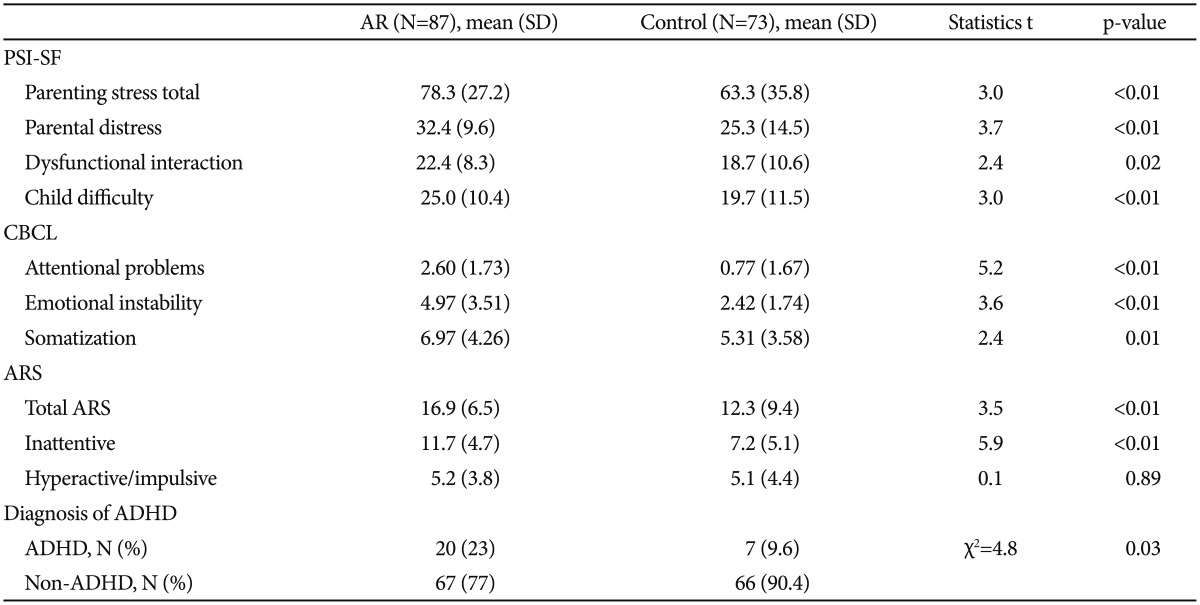
Parenting stress in mothers of children with allergic rhinitis was higher than in mothers of children of control group. The PSI-SF total score was higher in the allergic rhinitis group compared to the control group (t=3.0, p<0.01). The three subscores of the PSI-SF including parental distress (t=3.7, p<0.01), parent-child dysfunctional interaction (t=2.4, p<0.01) and child difficulty (t=3.0, p<0.01) were also higher in the allergic rhinitis group than in the control group (Table 2).
There were also more emotional and behavioral problems in children with allergic rhinitis than those with the control group. The three CBCL subscales, somatization (t=5.2, p<0.01), emotional instability (t=3.6, p<0.01), and attentional problems (t=2.4, p<0.01), were higher in the allergic rhinitis group in the control group (Table 2). The ARS total score (t=3.5, p<0.01) and inattentive subscore (t=5.9, p<0.01) were also higher in the allergic rhinitis group than in the control group, whereas there was no difference with hyperactive/impulsive subscore.
Children with an ARS total score Ōēź16, 25 children with allergic rhinitis and 13 children of control group, took the CAT and completed an ADHD diagnostic interview administered by a child psychiatrist. There was no significant correlation between the omission errors in CAT and the severity of allergic rhinitis (B=-0.2, SD=0.88, t=0.3, p=0.84). Twenty children (23%) from the allergic rhinitis group and seven children (9.6%) from the control group met criteria for probable ADHD. There were significantly more ADHD in the allergic rhinitis group than in the control group (Žć2=4.8, p=0.03) (Table 2).
There was a significant relationship between the severity of allergic rhinitis and the total ARS score in ordinary regression analysis (B=8.4, SD=2.5, t=3.3, p<0.01).
In the stepwise logistic regression analysis, the total PSI-SF score was correlated with severity of allergic rhinitis symptoms (beta=0.50, p<0.01) and the total ARS score (beta=0.39, p<0.01) (Table 3).
In addition, in the allergic rhinitis and ADHD group, the PSI-SF parent-child dysfunctional interaction subscale score was correlated with the ARS subscales of impulsivity and hyperactivity (r=0.41, p=0.01).
There were significant positive correlations between the total PSI-SF score and each subscale of the CBCL, including somatization (r=0.39, p<0.01), emotional instability (r=0.45, p<0.01) and attentional problems (r=0.38, p<0.01). There were also correlations between the PSI-SF parental distress subscale and each subscale of the CBCL, somatization (r=0.31, p<0.01), emotional instability (r=0.36, p<0.01) and attentional problems (r=0.31, p<0.01). There also were significant correlations between the PSI-SF parent-child dysfunctional interaction subscale and the CBCL somatization (r=0.39, p<0.01), emotional instability (r=0.45, p<0.01) and attentional problems (r=0.38, p<0.01) subscales. Finally, there were significant correlations between the PSI-SF child difficulty subscale and the CBCL somatization (r=0.43, p<0.01), emotional instability (r=0.52, p<0.01) and attentional problems subscales (r=0.41, p<0.01) (Table 4).
ADHD symptoms were associated with allergic rhinitis symptoms. Many epidemiological studies support the co-existence of ADHD in allergic diseases, including atopic dermatitis, asthma and allergic rhinitis.24,41,42 The coexistence of allergic symptoms in children with ADHD has been also reported.17,26
Although the patho-physiological mechanisms of the comorbidity of pediatric allergic disease and ADHD have not been definitively revealed, several models suggest that they are highly correlated. The primary aim of the present study was to investigate the co-existence of behavior problems, especially ADHD behavior symptoms, in children with allergic rhinitis. We found that children with allergic rhinitis versus those with control group had significantly more ADHD-related behavioral problems across all aspects of behavior based on the CBCL (emotional instability and attentional problems), the ARS, and the diagnostic rate of ADHD. Even in children with a subthreshold diagnosis of ADHD, behavioral symptoms were higher in the allergic rhinitis group than in the control group.
However, there was no difference between children with allergic rhinitis and control group with respect to hyperactive/impulsive subscore of ARS. Interestingly, only inattention symptoms (not hyperactivity symptoms) were associated with allergic rhinitis in current research. This finding could be investigated and explained more through further study. Recent studies reported the correlation between cognitive symptoms and allergic rhinitis.11,43 The symptoms of allergic rhinitis like nasal obstruction, itching, rhinorrhoea and sneezing cause cognitive distraction and inattention.11 The symptoms of allergic rhinitis also affects quality of sleep and it results in day time fatigue and impairment of cognition and memory.11,43 Complications of allergic rhinitis like sinusitis, eustachian dysfunction and associated conductive hearing loss may enhance the learning dysfunction.11 Although the exact mechanism was not revealed, inattention symptom is seemed to be more correlated with allergic rhinitis than hyperactivity/impulsivity symptom.
In this study, we used a comprehensive diagnostic process for determining ADHD and allergic rhinitis in collaboration with a pediatric allergist and child psychiatrist. The child and adolescent psychiatrists evaluated the ADHD symptoms through the interview based on DSMD-IV criteria, ARS, and a computerized continuous performance test. These systemized methodologies increased the accuracy of our results.
We also examined how comorbid ADHD and allergic rhinitis affect parenting stress. This study showed that parenting stress was higher in mothers of children with allergic rhinitis than in those of control group. Additionally, among children with allergic rhinitis, the co-existence of ADHD significantly increased parenting stress and children's emotional and behavioral problems.
The psychoendocrine and psychoneuroimmunological model of comorbidity of atopic dermatitis and ADHD posits that increased stress levels due to daily adverse experiences in ADHD children may trigger atopic dermatitis via neuroimmunological mechanisms.44 It has been suggested that prenatal and early childhood exposure to psychosocial stress factors can predispose children toward allergic diseases.45,46
The results of this present study support this theory. Parenting distress, parent-child dysfunctional interaction, and the child difficulty subscales of the PSI-SF were associated with somatization, emotional instability, and attentional problems in children with allergic rhinitis.
The results of this study indicate that management of comorbid ADHD symptoms in children with allergic rhinitis is very important for reducing parenting stress and improving children's ADHD behavioral symptoms.47
Thus, in the case of pediatric allergic rhinitis with ADHD, screening and early intervention for ADHD are crucial for reducing parenting stress, which will, in turn, have a positive effect on the progress of their children's diseases and their overall quality of life.
There were several methodological limitations in this study. First, the results of this study are cross sectional in regard to an active allergic rhinitis state. More studies are needed to compare parental stress and children's ADHD behaviors between an active allergic rhinitis state and an allergic symptomfree state. Second, though we tried to diagnose ADHD using comprehensive methods including the ARS, CAT, and a child psychiatrist's interview, our diagnostic process is still limited due to the absence of a follow-up meeting with parents and their children for a confirmed diagnosis. An additional weakness is that we could not exclude the comorbid state of allergic conjunctivitis, asthma or atopic dermatitis, even if the symptoms were not severe.
In a nationwide population-based study in Taiwan, Tsai et al.42 reported an increased rate of ADHD among allergic rhinitis patients, but comorbidity of neither atopic dermatitis nor bronchial asthma carried a high risk for ADHD in allergic rhinitis patients.
Future studies should recruit a larger number of subjects for each allergic disease (atopic dermatitis, asthma and allergic rhinitis), along with an appropriate control group for further study.
In summary, this study demonstrated that ADHD symptoms were common in children with allergic rhinitis, and this factor could alter parenting stress and disrupt the parent-child relationship. Even behavioral symptoms that were not severe enough to meet DSM-IV criteria for diagnosing ADHD might disturb the interaction between a child and his/her parents. Therefore, early evaluation and treatment of ADHD may benefit children with allergic rhinitis and their parents by improving behavioral symptoms and reducing factors that aggravate parenting stress. More studies are needed to evaluate the effect of managing comorbid ADHD with medication or psychosocial treatment in children.
Acknowledgments
This work was supported by a grant of the Korean Health Technology R&D Project, Ministry of Health & Welfare, Republic of Korea (A120013).
References
1. Fedele DA, Grant DM, Wolfe-Christensen C, Mullins LL, Ryan JL. An examination of the factor structure of parenting capacity measures in chronic illness populations. J Pediatr Psychol 2010;35:1083-1092. PMID: 20484329.


2. Hilliard ME, Monaghan M, Cogen FR, Streisand R. Parent stress and child behaviour among young children with type 1 diabetes. Child Care Health Dev 2011;37:224-232. PMID: 21083686.


3. Rabung S, Ubbelohde A, Kiefer E, Schauenburg H. Attachment security and quality of life in atopic dermatitis. Psychother Psychosom Med Psychol 2004;54:330-338. PMID: 15284944.


4. Walker LO, Cheng CY. Maternal empathy, self-confidence, and stress as antecedents of preschool children's behavior problems. J Spec Pediatr Nurs 2007;12:93-104. PMID: 17371553.


5. Shalowitz MU, Berry CA, Quinn KA, Wolf RL. The relationship of life stressors and maternal depression to pediatric asthma morbidity in a subspecialty practice. Ambul Pediatr 2001;1:185-193. PMID: 11888399.


6. Pauli-Pott U, Darui A, Beckmann D. Infants with atopic dermatitis: maternal hopelessness, child-rearing attitudes and perceived infant temperament. Psychother Psychosom 1999;68:39-45. PMID: 9873241.


7. Halterman JS, Yoos HL, Conn KM, Callahan PM, Montes G, Neely TL, et al. The impact of childhood asthma on parental quality of life. J Asthma 2004;41:645-653. PMID: 15584314.


8. Williams S, Sehgal M, Falter K, Dennis R, Jones D, Boudreaux J, et al. Effect of asthma on the quality of life among children and their caregivers in the Atlanta Empowerment Zone. J Urban Health 2000;77:268-279. PMID: 10856008.



9. Shen CY, Lin MC, Lin HK, Lin CH, Fu LS, Fu YC. The natural course of eczema from birth to age 7 years and the association with asthma and allergic rhinitis: a population-based birth cohort study. Allergy Asthma Proc 2013;34:78-83. PMID: 23406940.


10. Schmitt J, Buske-Kirschbaum A, Roessner V. Is atopic disease a risk factor for attention-deficit/hyperactivity disorder? A systematic review. Allergy 2010;65:1506-1524. PMID: 20716320.


11. Mir E, Panjabi C, Shah A. Impact of allergic rhinitis in school going children. Asia Pac Allergy 2012;2:93-100. PMID: 22701858.



12. Sly RM. Changing prevalence of allergic rhinitis and asthma. Ann Allergy Asthma Immunol 1999;82:233-248. PMID: 10094214.


13. Stipic-Markovic A, Pevec B, Pevec MR, Custovic A. Prevalence of symptoms of asthma, allergic rhinitis, conjunctivitis and atopic eczema: ISAAC (International Study of Asthma and Allergies in Childhood) in a population of schoolchildren in Zagreb. Acta Med Croatica 2003;57:281-285. PMID: 14639862.

14. Bjorksten B, Clayton T, Ellwood P, Stewart A, Strachan D. ISAAC Phase III Study Group. Worldwide time trends for symptoms of rhinitis and conjunctivitis. Phase III of the International Study of Asthma and Allergies in Childhood. Pediatr Allergy Immunol 2008;19:110-124. PMID: 17651373.


15. Hong S, Son DK, Lim WR, Kim SH, Kim H, Yum HY, et al. The prevalence of atopic dermatitis, asthma, and allergic rhinitis and the comorbidity of allergic diseases in children. Environ Health Toxicol 2012;27:e2012006PMID: 22359737.



16. Spencer TJ, Biederman J, Mick E. Attention-deficit/hyperactivity disorder: diagnosis, lifespan, comorbidities, and neurobiology. J Pediatr Psychol 2007;32:631-642. PMID: 17556405.


17. Brawley A, Silverman B, Kearney S, Guanzon D, Owens M, Bennett H, et al. Allergic rhinitis in children with attention-deficit/hyperactivity disorder. Ann Allergy Asthma Immunol 2004;92:663-667. PMID: 15237769.


18. Polanczyk G, de Lima MS, Horta BL, Biederman J, Rohde LA. The worldwide prevalence of ADHD: a systematic review and metaregression analysis. Am J Psychiatry 2007;164:942-948. PMID: 17541055.


19. Biederman J, Faraone SV. Attention-deficit hyperactivity disorder. Lancet 2005;366:237-248. PMID: 16023516.


20. Mash EJ, Johnston C. Parental perceptions of child behavior problems, parenting self-esteem, and mothers' reported stress in younger and older hyperactive and normal children. J Consult Clin Psychol 1983;51:86-99. PMID: 6826870.


21. Harvey E, Danforth JS, McKee TE, Ulaszek WR, Friedman JL. Parenting of children with attention-defecit/hyperactivity disorder (ADHD): the role of parental ADHD symptomatology. J Atten Disord 2003;7:31-42. PMID: 14738179.


22. Lee PC, Lin KC, Robson D, Yang HJ, Chen VC, Niew WI. Parent-child interaction of mothers with depression and their children with ADHD. Res Dev Disabil 2013;34:656-668. PMID: 23123879.


23. Macek J, Gosar D, Tomori M. Is there a correlation between ADHD symptom expression between parents and children? Neuro Endocrinol Lett 2012;33:201-206. PMID: 22592202.

24. Roth N, Beyreiss J, Schlenzka K, Beyer H. Coincidence of attention deficit disorder and atopic disorders in children: empirical findings and hypothetical background. J Abnorm Child Psychol 1991;19:1-13. PMID: 2030244.


25. Han DH, Kim SH, Chung US, Cho JH, Park JS, Ahn JY, et al. Association between Atopic Dermatitis and Attention Deficit Hyperactivity Disorder Symptoms in Korean Children. Korean J Psychosom Med 2006;14:88-93.
26. Suwan P, Akaramethathip D, Noipayak P. Association between allergic sensitization and attention deficit hyperactivity disorder (ADHD). Asian Pac J Allergy Immunol 2011;29:57-65. PMID: 21560489.

27. Warschburger P, Buchholz HT, Petermann F. Psychological adjustment in parents of young children with atopic dermatitis: which factors predict parental quality of life? Br J Dermatol 2004;150:304-311. PMID: 14996102.


28. Nagano J, Kakuta C, Motomura C, Odajima H, Sudo N, Nishima S, et al. The parenting attitudes and the stress of mothers predict the asthmatic severity of their children: a prospective study. Biopsychosoc Med 2010;4:12PMID: 20929533.



29. Abidin RR, Wilfong E. Parenting stress and its relationship to child health care. Child Health Care 1989;18:114-116. PMID: 10292918.


30. Abidin RRO. Parenting Stress Index: Professional Manual. 3rd Edition. FL: Psychological Assessment Resources; 1995.
31. Lee KS, Chung KM, Park JA, Kim HJ. Reliability and validity study for the Korean version of Parenting stress index short form (K-PSI-SF). Korean J Woman Psychol 2008;13:363-377.

32. Achenbach TM. Manual for Child Behavior Checklist 4-18, 1991 Profile. Burlington: University of Vermont Department; 1991.
33. Oh KJ, Lee HL, Hong KE, Ha EH. Korean Child Behavior Checklist. Seoul: Jungang Press; 1997.
34. DuPaul GJ, Power TJ, McCoey K, Ikeda M, Anastopoulos AD. Reliability and validity of parent and teacher ratings of attention-deficit/hyperactivity disorder symptoms. J Psychoeduc Assess 1998;16:55-68.

35. So YK, Noh JS, Kim YS, Ko SG, Koh YJ. The reliability and validity of Korean parent and teacher ADHD rating scale. J Korean Neuropsychiatr Assoc 2002;41:283-289.
36. Zhang S, Faries DE, Vowles M, Michelson D. ADHD Rating Scale IV: psychometric properties from a multinational study as a clinician-administered instrument. Int J Methods Psychiatr Res 2005;14:186-201. PMID: 16395872.


37. Yoo HK, Lee J, Kang SH, Park EH, Jung J, Kim BN. Standardization of the comprehensive attention test for the Korean children and adolescents. J Korean Acad Child Adolesc Psychiatry 2009;20:68-75.
38. Brozek JL, Bousquet J, Baena-Cagnani CE, Bonini S, Canonica GW, Casale TB, et al. Allergic Rhinitis and its Impact on Asthma (ARIA) guidelines: 2010 revision. J Allergy Clin Immunol 2010;126:466-476. PMID: 20816182.


39. Yang YH, Kim JW, Kim YN, Cho SC, Kim BN. Screening for Attention Deficit/Hyperactivity Disorder for children in Seoul. J Korean Neuropsychiatr Assoc 2008;47:292-298.
40. American Psychiatric Association Press. DSM-IV, Diagnostic and Statistical Manual of Mental Disorders. Fourth Edition. Washington DC: American Psychiatric Association Press; 1994.
41. McQuaid EL, Weiss-Laxer N, Kopel SJ, Mitchell DK, Nassau JH, Wamboldt MZ, et al. Pediatric Asthma and Problems in Attention, Concentration, and Impulsivity: Disruption of the Family Management System. Fam Syst Health 2008;26:16-29. PMID: 19198669.



42. Tsai MC, Lin HK, Lin CH, Fu LS. Prevalence of attention deficit/hyperactivity disorder in pediatric allergic rhinitis: a nationwide populationbased study. Allergy Asthma Proc 2011;32:41-46. PMID: 22221429.


43. Jauregui I, Mullol J, Davila I, Ferrer M, Bartra J, del Cuvillo A, et al. Allergic rhinitis and school performance. J Investig Allergol Clin Immunol 2009;19(Suppl 1):32-39.

44. Buske-Kirschbaum A, Schmitt J, Plessow F, Romanos M, Weidinger S, Roessner V. Psychoendocrine and psychoneuroimmunological mechanisms in the comorbidity of atopic eczema and attention deficit/hyperactivity disorder. Psychoneuroendocrinology 2013;38:12-23. PMID: 23141851.


45. Yonas MA, Lange NE, Celedon JC. Psychosocial stress and asthma morbidity. Curr Opin Allergy Clin Immunol 2012;12:202-210. PMID: 22266773.



46. Richards LM. It is time for a more integrated bio-psycho-social approach to ADHD. Clin Child Psychol Psychiatry 2013;18:483-503. PMID: 23104966.


47. Motoyama K, Matsuzaka T, Nagaoka T, Matsuo M. The effect of parent training program on children with attention deficit/hyperactivity disorders and/or pervasive developmental disorders. No To Hattatsu 2012;44:289-294. PMID: 22844759.

Table┬Ā2
Comparison of the parenting stress, behavior problem and ADHD frequency between AR group and control group
Table┬Ā3
The correlation of the parenting stress and the severity of allergic rhinitis, and the correlation between parenting stress and ADHD-like behavior symptom









