Similarities of Aspects of Biological Rhythms between Major Depression and Bipolar II Disorder Compared to Bipolar I Disorder: A Finding from the Early-Onset Mood Disorder Cohort
Article information
Abstract
Objective
The biological rhythm is closely related to mood symptoms. The purpose of this study was to assess the differences in biological rhythms among subjects with mood disorder [bipolar I disorder (BD I), bipolar II disorder (BD II), major depressive disorder (MDD)] and healthy control subjects.
Methods
A total of 462 early-onset mood disorder subjects were recruited from nine hospitals. The controls subjects were recruited from the general population of South Korea. Subject groups and control subject were evaluated for the Korean language version of Biological Rhythms Interview of Assessment in Neuropsychiatry (K-BRIAN) at the initial evaluation.
Results
The mean K-BRIAN scores were 35.59 [standard deviation (SD)=13.37] for BD I, 43.05 (SD=11.85) for BD II, 43.55 (SD=12.22) for MDD, and 29.1 (SD=8.15) for the control group. In the case of mood disorders, biological rhythm disturbances were greater than that in the control group (p<0.05). A significant difference existed between BD I and BD II (BD I <BD II, p<0.001) and between BD I and MDD (BD I<MDD, p< 0.001) but no difference was observed between BD II and MDD.
Conclusion
BD II and MDD are similar to each other but different from BD I in biological rhythm patterns in early-onset mood disorder cases. Biological rhythm disturbances are similar for early-onset major depression and BD II.
INTRODUCTION
Circadian rhythms exist in lifeforms from microorganisms to mammals and drive circadian cycles (cycles that repeat roughly every 24 hours) to help anticipate and respond to environmental changes [1]. Circadian rhythms help synchronize an organism to periodic fluctuations in the external environment and also facilitate integration of an organism’s internal social environment [2]. Recognition of its importance is growing, and the Nobel Prize in Physiology or Medicine 2017 was awarded to Jeffrey Hall, Michael Rosbash, and Michael Young, who contributed to circadian biology by studying the biological clock and circadian oscillation control through period proteins [3]. The biological rhythm represented by a circadian rhythm is closely related to mood symptoms as well as physiological effects such as sleep patterns, eating behavior, hormone secretion, blood pressure, and body temperature [4]. Previous studies showed that an altered circadian rhythm and sleep disturbances occur in depressive disorders [2], and irregularity of the sleep-wake cycle, eveningness-chronotype, and abnormal melatonin secretion occur in bipolar disorder [5-8]. These studies suggest the changes that occur to biological rhythms (including sleep) in those with mood disorders.
Additionally, integrated insights give an understanding of how biological rhythm disturbances affect a variety of conditions and biological functions such as—monoamine signaling of mood disorders, the immune system, hypothalamic–pituitary–adrenal (HPA) axis regulation, metabolic peptides, cellular processes (redox, mitochondria, apoptosis, neurogenesis) [9], cerebral parenchyma, suprachiasmatic nucleus [10], and regulation of the biological clock through epigenetic control [11]. Researchers have made an effort, through a variety of measurements and actigraphy, to evaluate biological rhythms in subjects with mood disorders objectively [12,13]. In addition, studies show that correction of biological rhythms through light therapy, behavior modification, and pharmacological agents (such as melatonin) reduces the duration of mood-related symptoms and the severity of other symptoms [14,15], improving the overall quality of life [16]. Thus, objective analysis of biological rhythms in the treatment of subjects with early mood disorders may give insights into the diagnosis, treatment, and prognosis of subjects.
The Biological Rhythm Interview of Assessment in Neuropsychiatry (BRIAN) is an assessment that extends to areas including social activity and eating patterns, in contrast to assessments such as the Pittsburgh Sleep Quality Index (PSQI) [17], the Morningness-Eveningness Questionnaire (MEQ) [18], and the Seasonal Pattern Assessment Questionnaire (SPAQ) [19]. BRIAN consists of 21 items divided into five main areas, related to circadian rhythm disturbance in psychiatric subjects. These five domains are sleep, activities, social-rhythm, eating-pattern, and predominant-rhythm [20], and BRIAN’s validity and reliability have been confirmed for Korean population [21].
The purpose of this study was to evaluate sleep, activity, social-activity, eating patterns, and predominant rhythm (chronotype) in early-onset mood disorder subjects and healthy subjects and then verify the biological rhythm differences among bipolar I disorder (BD I), bipolar II disorder (BD II), major depressive disorder (MDD) and control subjects.
METHODS
Participants
A total of 467 subjects were recruited. Each subject was less than 35 years old and had a major mood disorder within two years of the treatment; or less than 25 years old and presently diagnosed with a major mood disorder. Subjects with evidence of intellectual disabilities, organic BRIAN injury, or difficulty in reading and understanding Korean characters were excluded [22]. Subjects were recruited from nine different hospitals participating in the Mood Disorder Cohort Research Consortium (MDCRC), including Korea University Hospital, Seoul National University Hospital, Seoul National University Bundang Hospital, Samsung Medical Center, Severance Hospital, Busan National University Hospital, Gyeongsang National University Hospital, Cheonnam National University Hospital, and the National Center for Mental Health [22]. Subjects were diagnosed using the Mini-International Neuropsychiatric Interview (M.I.N.I.) [23], which classified 138 subjects with BD I, 170 subjects with BD II, and 159 subjects with MDD. 40 control subjects were recruited by matching gender and age from the general population of young adults at Korea University Anam Hospital [21].
All subjects and control subjects received informed consent prior to the test, and this study was reviewed by the Institutional Review Boards for all nine participating hospitals (2015 AN0239) [22].
Assessments
During the initial evaluation, 467 subjects were evaluated for K-BRIAN scores and sociodemographic characteristics. A Korean language version of the mood disorder questionnaire (K-MDQ) [24] was performed to identify bipolarity in the subject. The MDQ is a self-report questionnaire designed to help detect bipolar disorder and focuses on symptoms of hypomania and mania [25]. The K-MDQ was validated in 2009 [24]. Korean language versions of the Montgomery-Asberg Depression Rating Scale (K-MADRS) [26] and the Young Mania Rating Scale (YMRS) [27] were used to evaluate depressive and manic-hypomanic symptoms respectively. Subjects with a K-MADRS score greater than 35 and a YMRS score greater than 25 were classified as severely ill and expected to have low reliability due to mood symptoms [28,29]. In those cases, the K-BRIAN value was used after the mood symptoms improved.
A total of 462 subjects were enrolled. Two subjects with BD II and three with MDD were excluded. The enrolled participants included 138 subjects with BD I, 168 subjects with BD II, and 156 subjects with MDD. The control subjects were administered the M.I.N.I. [23] by a psychiatrist and assessed using the K-BRIAN [21] and the K-MDQ [24]. The K-BRIAN total score used for this study is the sum of the values of four subgroups—sleep, activities, social-rhythm, and eating-patterns. Chronotypes were excluded from the score as in earlier studies [20,21,30-32].
Statistical analyses
First, a normality test of the four groups (BD I, BD II, MDD, and control) was performed. Then, a one-way analysis of variance (ANOVA) for continuous data and a chi-square test for categorical data was performed to analyze statistical differences between the four groups. A Levene’s test for variance and a Welch’s t-test for robustness were performed to test for equal variance. Dunnett’s T3 method was performed post hoc based on a 0.05 p-value significance level. All statistical analyses were performed using SPSS version 21 for windows (IBM, Corp., Armonk, NY, USA).
RESULTS
The mean age of each group was 23.49 (SD 3.48) years for BD I, 23.00 (SD 3.01) years for BD II, 22.67 (SD 3.66) years for MDD, and 24.76 (SD 4.46) years for the control group. There was a statistically significant difference in mean age between MDD and control group (F=3.182, p<0.05). Mean age at onset was 18.34 (SD 4.88) years in BD I, 16.46 (SD 3.76) years in BD II, and 17.89 (SD 4.72) years in MDD; BD I and BD II are statistically different (F=7.675, p<0.001). The gender ratio was 60.14% female in BD I, 59.51% female in BD II, 52.56% female in MDD, and 50% in the control group. There was no statistically significant difference in gender ratio between groups (χ2=4.637, p=0.200). Body-Mass-Index (BMI) was 24.19 (SD 3.58) for BD I, 23.83 (SD 4.52) for BD II, 23.36 (SD 4.01) for MDD.
Socioeconomic status was classified into five categories, taking into account occupation and income [33]. For education level, the percentage of subjects who attended the undergraduate university level or higher were identified. There was a statistically significant difference in socioeconomic status and education level between study groups and the control group (p<0.001). Table 1 shows the sociodemographic characteristics of the study’s subjects.
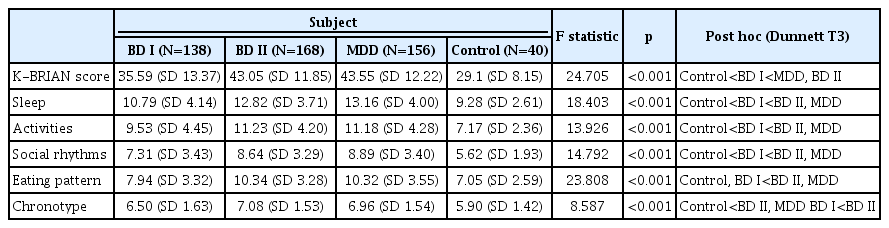
The value of the K-BRIAN score was 35.59 (SD 13.37) for BD I, 43.05 (SD 11.85) for BD II, 43.55 (SD 12.22) for MDD, and 29.1 (SD 8.15) for the control group. The K-BRIAN values for each subgroup are shown in Table 2. The K-BRIAN scores among the four groups are statistically different (F=24.705, p<0.001). Post hoc analyses of the scores yielded the following statistical differences for BD I vs. BD II (BD I is less than BD II, p<0.001), BD I vs. MDD (BD I is less than MDD, p<0.001). However, no significant difference was found between the BD II and MDD groups (p=0.982)
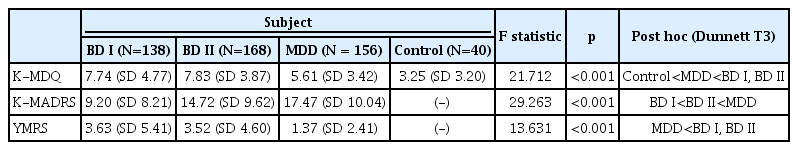
Mean K-MDQ scores were 7.74 (SD 4.77) for BD I, 7.83 (SD 3.87) for BDII, 5.61 (SD 3.42) for MDD, and 3.25 (SD 3.20) for the control group. There are significant differences among the four groups, BD I, BD II, MDD, and the control group (F=21.712, p<0.001). As a result of post hoc analysis, BD I was greater than MDD (p<0.001) and BD II was greater than MDD (p<0.001). However, no significant difference was found between the BD I and BD II groups (p=0.997). The K-MADRS results were 9.20 (SD 8.21) for BD I, 14.72 (SD 9.62) for BD II, and 17.47 (SD 10.04) for MDD, showing statistically significant differences among the three groups, BD I, BD II, MDD (F= 29.263, p<0.001), In post hoc analysis, BD I and MDD (BDI is less than MDD, p<0.001), BD II and MDD (BD II is less than MDD, p<0.001) were statistically different. For the mean YMRS scores, BD I was 3.63 (SD 5.41), BD II was 3.52 (SD 4.60), and MDD was 1.37 (SD 2.41). A significant difference exists among three groups, BD I, BD II, MDD (F=13.631, p<0.001). In post hoc analysis comparison BD I and MDD (BD I is greater than MDD, p<0.001), BD II and MDD (BD II is greater than MDD, p<0.001) with statistical significance. The clinical characteristics of the study subjects are shown in Table 3.
DISCUSSION
Earlier studies suggest that biological rhythms and physiological functions of the body and the mood influence each other directly and indirectly [5,9,10,34,35]. It is important to control disturbances to biological rhythms in order to reduce the severity of adverse mood-related symptoms, reduce the duration of these symptoms, and increase the overall quality of life [14-16]. According to a prior study examining BD, biological rhythms checked with BRIAN can be used as a subject’s trait marker rather than a static state at only the time of the assessment [36]. In the previous study using BRIAN, the biological rhythm disturbance was greater in BD than in the control group [20]. In drug-naïve, young adult subjects with mood disorders, biological rhythm disturbance was greater than that of the control group and the BD group showed higher BRIAN values than MDD [32]. In a study of 1,023 subjects, those with BD had higher BRIAN values than those with MDD, and when they were classified by mood, subjects showed euthymic MDD–euthymic bipolar–unipolar depression–hypomanic/manic/mixed–bipolar depression in that order, indicating that the most disturbing biological rhythm was found in bipolar depression [31]. However, in a recent study, subjects with MDD tended to have a higher total BRIAN score than those with BD, but there was no statistical difference between the two groups [13].
However, some earlier studies have weaknesses, such as only comparing the BD group and control group [20,37], or only comparing the BD group to those with depressive disorders [31,32]. In addition, only disturbances of biological rhythms according to mood were identified in subjects with BD [30,35,38]. The strength of the present study is that it was designed to analyze BD I and BD II and to compare the biological characteristics of the disease groups in more detail. Furthermore, analyses of study data identified characteristics of each disease group for early-onset mood disorders in young adults.
According to the result of present study, the disturbance of biological rhythms for those with BD II and MDD is statistically significant compared to subjects with BD I. This differs from previous studies [31,32,39] which proposed that BD is more disturbing to biological rhythms than MDD. Therefore, it is important to note that BD I and BD II, and MDD show different biological rhythm patterns in early mood disorders.
First, when comparing the K-MDQ score, both BD I and BD II groups scored higher than the MDD group. However, the BD I and BD II groups could not be distinguished. The results of this study show that the disturbance of the biological rhythms for BD II is greater in all subgroups (sleep, activities, social rhythm, eating pattern, chronotype) compared to BD I. In the case of BD II, the general clinician considers BD II to be a simple and milder form of a manic-depressive illness [40], and often BD II goes underdiagnosed or misdiagnosed as unipolar disorder or personality disorder [41]. Many studies have confirmed that BD I and BD II have different pathophysiological characteristics, and BD II is known to have more clinically complex characteristics [42]. In particular, BD II subjects are known to have depressive predominant polarity [43,44], suffer from a longer depressive duration (compared to BD I), and experience more persistent residual depression [45]. In addition, subjects with BD II have a higher incidence of premenstrual symptoms compared to subjects with BD I [46]. Combining this evidence, we hypothesize that BD I and BD II have different characteristics in terms of the long-term disease course and pathophysiology. In view of earlier results, the distinction between BD I and BD II, which are bound by the same bipolar spectrum, is important and reveals the limitations of an assessment focused on symptoms (such as K-MDQ). Thus, BRIAN, which is known to reflect a subject’s traits [36], may be used as a tool to distinguish bipolar disorder’s endophenotype if subsequent studies strengthen the evidence.
Second, Subjects with early-onset MDD showed similar levels of disturbances in biological rhythms as those with BD II. However, using the results of K-MADRS, MDD subjects had a significantly higher value than BD subjects. According to some studies, 40–50% of subjects with depressive episodes in the out-subject and in-subject setting were diagnosed with BD during the course of the disease [47-50], and the risk factor of diagnostic change was related to these factors—onset at a young age, high number of depressive episodes, bipolar family history, female gender, psychosis, depressive mixed episodes with mood lability, psychomotor agitation, and crowded thoughts [48,51,52].
Studies have shown that the onset of first depression in BD subjects is faster than that of subjects with MDD [52-56] and the first episode of BD is known to begin primarily with depression [57]. Therefore, progression from early-onset major depression to BD is an important consideration for prognosis, course of disease, and choice of medication. Early-onset major depression showed a disturbance of biological rhythms similar to BD I and BD II. Hence, for subjects with early-onset major depression, the hallmarks of BD II should be noted throughout the disease such as more chronicity [58], lower probability of returning to a premorbid level of function between episodes [59], higher rate of rapid cycling [60], and shorter well periods [59]. With further research comparing biological rhythm disturbances to long-term MDD subjects, BRIAN will yield new criterion for suggesting bipolarity in early-onset major depression.
This current study also has limitations. The first is that the number of subjects in the control group was smaller than that of the subject groups, and most of the control group were college students. However, the goal of this study was to compare each subject group to each other. It is well known from previous studies that disturbances in biological rhythms are higher in the mood disorder groups than in the control group [20,31,32], Thus, a small control group population should not affect the validity of the study. In addition, the analysis of sociodemographic characteristics (education, tobacco) showed significant differences in the control group compared to the subject groups and should be considered due to the characteristics of the control subjects. The second limitation is that BRIAN itself has limitations such as recall-bias and answer-reliability problems [61], but it is meaningful in that it is not invasive and can easily obtain information serially. Finally, although biological rhythms identified through BRIAN are known to reflect the subject’s traits [36], circadian rhythm [62] and mood change with the seasons [63]. Follow-up studies are needed to determine the relationship between seasonality and biological rhythms.
This study is a large-scale examination of subjects with early-onset mood disorders in South Korea, and it takes an important step to separate BD I and BD II and analyze early-onset MDD. This study suggests a new approach to the characteristics of early-onset mood disorders through the assessment of biological rhythms. Existing assessments related to mood disorders can distinguish BD and MDD because they focus on symptoms, but there are limitations in actually distinguishing endophenotype of BD or diagnosing early-onset major depression. Assessments (such as BRIAN) that reflect the subject’s traits in terms of biological rhythms may provide additional information to the current diagnostic systems with further research. It is also realistic to believe that new tools for classifying diseases will arise from further research which could change the current practice of simply classifying overlapping diseases as degrees of severity.
Acknowledgements
This study was supported by the Korea Health 21 R&D Project funded by the Ministry of Health & Welfare (HM14C2606) and the National Research Foundation of Korea (2017M3A9F1031220), Republic of Korea.
Notes
The authors have no potential conflicts of interest to disclose.
Author Contributions
Conceptualization: Heon-Jeong Lee, Su Cheol Kim. Data curation: Heon-Jeong Lee, Chul-Hyun Cho, Yong-Min Ahn, Se Joo Kim, Tae Hyon Ha, Boseok Cha, Eunsoo Moon, Dong Yeon Park, Ji Hyun Baek, Hee-Ju Kang, Hyonggin An. Formal analysis: All author. Funding acquisition: Heon-Jeong Lee. Investigation: All author. Methodology: Heon-Jeong Lee, Su Cheol Kim, Chul-Hyun Cho, Yujin Lee, Ju Yeon Seo. Project administration: Heon-Jeong Lee, Su Cheol Kim. Resources: All author. Software: Su Cheol Kim, Chul-Hyun Cho. Supervision: Heon-Jeong Lee. Visualization: Su Cheol Kim, Chul-Hyun Cho, Yujin Lee. Writing—original draft: Su Cheol Kim. Writing—review& editing: Heon-Jeong Lee, Chul-Hyun Cho, Yujin Lee.