The Clinical Manifestation, Executive Dysfunction, and Caregiver Strain in Subthreshold Attention-Deficit/Hyperactivity Disorder
Article information
Abstract
Objective
Subthreshold attention-deficit/hyperactivity disorder (ADHD) has been suggested to be a “morbid condition” which also needs medical attention.
Methods
The present study recruited 89 children with subthreshold ADHD (sADHD), 115 children with diagnosed ADHD (cADHD), and 79 healthy controls (HC) to explore the clinical manifestation, executive functions (EFs) of sADHD, and the caregiver strain. The clinical manifestation was evaluated through clinical interviews and parent-reports. Executive functions were assessed both experimentally and ecologically. Caregiver strain was measured by a parent-reported questionnaire.
Results
For the clinical manifestation, both sADHD and cADHD indicated impairments when compared with HC. The comorbidities and the scaled symptoms indicated that the externalizing behaviors were relatively less serious in sADHD than cADHD, whereas the internalizing behaviors between two groups were comparable. For ecological EFs, sADHD scored between cADHD and HC in inhibition and working memory. For experimental EFs, sADHD was comparable to cADHD in inhibition, shifting, and was worse than cADHD in verbal working memory. For the caregiver strain, all scores of sADHD were between that in cADHD and that in HC.
Conclusion
Our present findings supported the suggestion of subthreshold ADHD as “morbid condition,” which should be treated with caution in clinical practice, especially for the internalizing behaviors and some key components of EFs.
INTRODUCTION
Attention-deficit/hyperactivity disorder (ADHD) is a neurodevelopmental disorder featured with inattention, hyperactivity, and impulsivity, which is associated with various functional impairments, including academic underachievement, interpersonal difficulties, and chaotic family life [1-3]. The worldwide prevalence rate of ADHD was about 5% in childhood and adolescence, and around 2.5% in adulthood [3-5]. A recent epidemiological survey in China revealed that 6.4% of schoolage children and adolescents have ADHD [6]. Moreover, caring for a child with ADHD tends to increase the economic burden of families, which was estimated to be five times greater than those without ADHD [7].
ADHD has become an important issue in public health, which has been aware of as a common psychiatric problem, resulting in increased rates on diagnosis and treatment. A new problem in recent clinical practices is that pediatric psychiatrists may encounter a substantial of visitors bothered by inattention, hyperactivity, or impulsivity, failing to meet the full diagnostic criteria of ADHD, but in need of professional help. According to the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5), a child must fulfill the following criteria to be diagnosed as ADHD: 6 or more symptoms of inattention and/or hyperactivity-impulsivity; symptoms have been present for at least six months, and they are inappropriate for developmental level [8]. For those who failed to meet the full diagnostic criteria, they may be grouped into ADHD-Not Otherwise Specified, but little recommendations were provided for how to offer appropriate help.
In the research area, studies on subclinical/subthreshold ADHD can be found. Two systematic reviews indicated that subthreshold ADHD is a morbid condition, with significantly high comorbidity rates with other psychiatric disorders, and associated with more behavioral problems and functional impairments [9,10]. Moreover, children with subthreshold ADHD (sADHD) are more likely to progress into ADHD or other psychiatric disorders in subsequent years, especially those whose subthreshold symptoms were neglected by their parents [11]. Therefore, efforts should be made to protect sADHD from current difficulties and future adversities.
In addition, in children with mental health bothering, caregivers should not be neglected. On one hand, there is a reciprocal relationship between parenting and children behavior. In longitudinal studies, while child behaviors can predict the level of caregiver strain, parenting stress can influence the development of child behaviors [12-14]. On the other hand, the strain of caregivers may influence the help seeking behavior of children. Surveys on the utilization of mental health services indicated that caregivers may play a dominant role in the usage of medical services in children and adolescents [15]. Also, a study in elementary children at high risk for ADHD found that caregiver strain can significantly increase the likelihood of ADHD treatment [16].
In this study, we will focus on this group of sADHD who visited pediatric psychiatrists for ADHD-like problems. To be specific, we conceptualize subthreshold ADHD as having 4–5 symptoms of inattention and/or 4–5 symptoms of hyperactivity/impulsivity, in congruence with the criteria adopted by the World Health Organization and some other researchers [17,18]. Following a description on their clinical features, we will carefully investigate their executive functions and caregiver strain. We propose that sADHD will show poorer executive functions and higher caregiver strain in comparison to healthy controls (HCs), and their impairments will be milder than children with ADHD (cADHD). As an addition, we planned that if the above assumptions were tested, we will take a step further to explore the potential mechanisms behind the relationship between executive functions and caregivers strain in sADHD.
METHODS
Participants and procedures
cADHD group and the sADHD group were recruited from referrals to clinics in the Peking University Sixth Hospital for problems with inattention and/or hyperactivity/impulsivity. Children in the HC group were recruited from primary or secondary schools in Beijing. The shared inclusion criteria for the three groups were: the age between 6 and 16 years old and an estimated full-scale intelligence quotient (IQ) above 70. The shared exclusion criteria were: major sensory-motor handicaps (e.g., paralysis, deafness, and blindness), a history of brain damage, and epilepsy.
Specific inclusion criteria for each groups were: for the sADHD group, the definition of subthreshold ADHD was based on the DSM-IV (4–5 inattentive symptoms and/or 4–5 hyperactive/hyperactivity symptoms), determined in semi-structured interviews performed by trained child psychiatrists; for the cADHD group, the diagnosis of ADHD was based on the DSM- IV, determined in semi-structured interviews performed by trained child psychiatrists; for the HC group, neither ADHD nor other psychiatric diseases were reported by parents, which was further verified by attending researchers.
The procedures used in this study adhere to the tenets of the Declaration of Helsinki. Informed consent was obtained from all of the children and their parents involved in the study. Ethics approval was obtained from the ethics committee of Peking University Sixth Hospital/Institute of Mental Health. The institutional review board (IRB) number is PKUH6 (2016)-(6).
Measures
Clinical assessments
The semi-structured Clinical Diagnostic Interview Scale (CDIS) is a semi-structured diagnostic interview according to the DSM-IV criteria [19]. Parents were interviewed with CDIS by senior psychiatrists to determine if the child meets the diagnostic criteria for ADHD and other psychiatric disorders. The Chinese Wechsler Intelligence Scale for Children (C-WISC) was used to assess the IQ [20]. Higher IQ indicates better intelligence.
The ADHD Rating Scale-IV (ADHD-RS) is a concise scale designed to evaluate symptoms of ADHD [21]. ADHD-RS consists of 18 items, of which nine items assess inattention symptoms and nine items assess hyperactivity/impulsivity symptoms. The higher the score is, the more severe the symptoms are.
The Conners Parent Symptom Questionnaire (PSQ) was developed to evaluate the behavioral problems of children [22]. PSQ consists of six subscales: conduct problem, learning problem, psychosomatic problem, impulsive-hyperactive, anxiety, and hyperactivity index. The higher the score is, the more severe the symptoms are.
Executive functions
The three core components of executive functions, including inhibition, working memory, and shifting, were evaluated both experimentally (Stroop Color Word Test [SCWT], Trail Making Test [TMT], and Digital Span Test [DST]) and ecologically (Behavior Rating Inventory of Executive Functioning [BRIEF]).
The SCWT was used to evaluate inhibition [23]. This test contained four parts: word naming (Part 1), color naming (Part 2), color interference (Part 3), and word interference (Part 4). As word naming is the advantageous response, inhibition ability was in the best indicated by the word interference index, subtracting the time for Part 4 from the time for Part 2. A higher score indicates a poorer inhibition ability.
The TMT was used to assess shifting ability [24]. There are two sheets of paper with 25 circles. Part 1 requires participants to connect circles with numbers (1–25) sequentially. Part 2 requires participants to connect circles sequentially between the numbers and letters (1-A-2-B-3-C, etc.). The index for shifting ability was the shift time, subtracting the time for Part 1 from the time for Part 2. A higher score indicates a poorer shifting ability.
The DST was used to measure verbal working memory. DST was consisted of two parts: forward and backward, asking the participant to repeat a series of numbers, in the forward sequence or in the backward sequence. In this study, we extracted the DST-backward score from C-WISC [20]. A higher score indicates a better working memory ability.
The BRIEF is an 86-item parent-report questionnaire designed to measure executive functioning in children aged 5 to 18 years [25]. Parents rate if their child’s behavior is “never,” “sometimes,” or “often” a problem, with higher ratings indicating greater perceived impairment. The BRIEF is composed of an overall score, the Global Executive Composite, and two broad indices: Metacognition Index (including Initiate, Working Memory, Plan/Organize, Organization of Materials, and Monitor subscales) and Behavior Regulation Index (including Inhibit, Shift, and Emotional Control subscales). Higher scores indicate poorer executive functioning. In this study, the scores of “Working Memory,” “Inhibit,” and “Shift” were analyzed.
Caregiver strain
The Caregiver Strain Questionnaire (CGSQ) was developed to assess strain experienced by parents of children and adolescents with serious emotional and behavioral disorder [26,27]. The CGSQ includes 21 items rated on a 5-point scale ranging from 1 (not at all a problem) to 5 (very much a problem). The CGSQ measures three dimensions of caregiver strain supported by exploratory and confirmatory factor analysis: objective strain (11 items), internalized subjective strain (6 items), and externalized subjective strain (4 items). Scores for each of the three subscales are calculated as the mean of the items in the subscale. An overall strain score is calculated by summing the three subscale scores.
Statistical analysis
We analyzed the differences between the cADHD group, the sADHD group, and the HC group using analysis of covariance for continuous variables. Gender and age were set as covariants. The chi-square test was used for categorical variables. For the identified significant group difference, post hoc comparisons between each pair of groups were performed, using Bonferroni corrections for multiple comparisons. Differences were deemed significant when p<0.05. The above statistical analyses were performed using IBM SPSS 24.0 (IBM Corp., Armonk, NY, USA) [28].
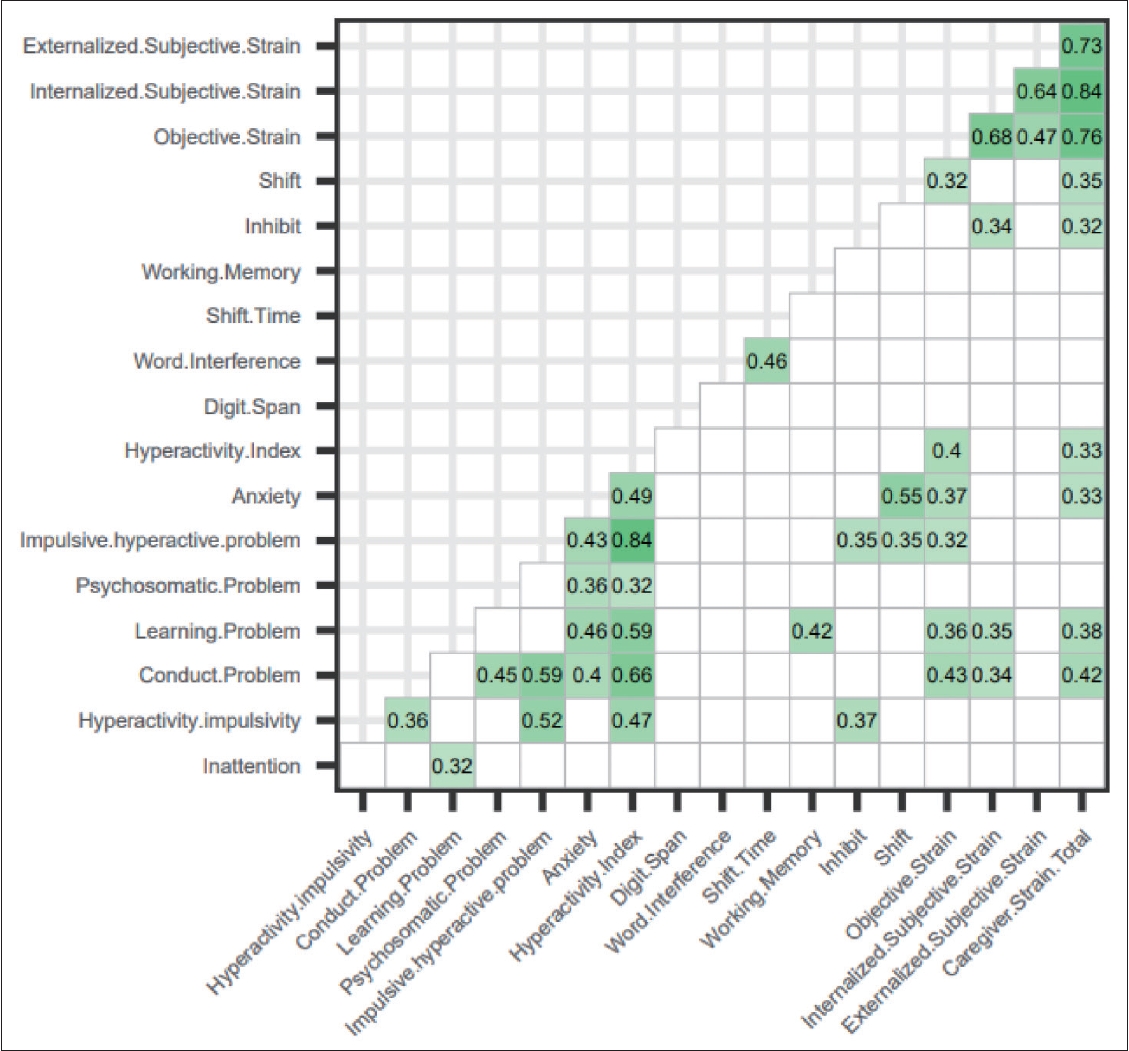
The correlogram was plotted with the ggcorrplot package in RStudio [29]. For the number of variables was 18, the significant level was set to be p<0.0028 to control type I error. We used green color and red color to indicate positive and negative significant correlation. Insignificant correlation was set to be blank. The coefficients of significant correlations were shown in boxes.
For exploring the potential relationship between executive functions and caregiver strain in sADHD group, we plan to construct possible (data driven) and reasonable (theory driven) mediation models using PROCESS macro on SPSS [30,31]. For the advantage of greater statistical power without assuming multivariate normality in the sampling distribution, bootstrap analyses will be adopted to test the significance of the indirect effects [32]. Parameter estimates and confidence intervals (CIs) of indirect effects will be generated based on 5,000 random samples. The mediation model will be demonstrated via a statistically significant indirect effect when the 95% bias-corrected CI for the parameter estimate does not contain zero.
RESULTS
Demographic characteristics and clinical features of cADHD, sADHD, and HC
The characteristics of children in three groups were illustrated in Table 1. The distributions of ages were significantly different (F(3, 283)=3.09, p=0.047), with the mean age of the HC group was higher than the sADHD group ([mean, M=10.20; standard deviation, SD=1.74]) vs. [M=9.25, SD=2.79], p=0.043). The gender distributions in the three groups also showed significant difference (F(3, 283)=21.37, p<0.001), with the cADHD group (83.5%) and the sADHD group (80.9%) showing higher male percentage than the HC group (57.0%).
Differences between the three groups on ADHD-RS scores, including the inattention subscore, the hyperactivity/impulsivity subscore, and the total mean score, were statistically significant (F(3, 283)=332.96, p<0.001; F(3, 283)=67.63, p<0.001; and F(3, 283)=232.55, p<0.001). Post hoc analyses indicated that the cADHD group scored the highest, followed by the sADHD group and then the HC group. The comorbidity status of the cADHD group and the sADHD group were shown in Table 1. Learning disorders were the top one comorbidity in both the cADHD group (34.8%) and the sADHD group (28.8%), with no statistically significant difference (χ2(1)=0.69, p=0.417). Also, comorbidity rates of tic disorders were remarkable in both groups, being 13.9% in the cADHD group and 13.0% in the sADHD group (χ2(1)=0.03, p>0.999). Externalizing comorbidity, oppositional defiant disorders (ODD) in particular, was more common in the cADHD group than the sADHD group (33.9% vs. 8.6%, p<0.001). In contrast, there was no significant difference between the cADHD group and the sADHD group on internalizing comorbidities like anxiety (7.0% vs. 5.8%, χ2(1)=0.10, p=0.758) and mood disorder (4.3% vs. 6.1%, χ2(1)=0.26, p=0.610).
PSQ scores in the three groups indicated that between-group differences were significant in all factors, including the conduct problem, learning problem, psychosomatic problem, impulsive-hyperactive, anxiety, and hyperactivity index (all p<0.001). Post hoc analyses showed that both the cADHD group and the sADHD group scored significantly higher than the HC group. The differences between the cADHD and sADHD groups were significant in the conduct problem ([M=7.17, SD=4.59] vs. [M=5.57, SD=3.94], p=0.015), learning problem ([M=7.17, SD=2.46] vs. [M=5.26, SD=2.40], p<0.001), impulsive-hyperactive ([M=5.37, SD=3.00] vs. [M=3.78, SD=2.62], p<0.001), and hyperactivity index ([M=13.20, SD=5.56] vs. [M=9.91, SD=4.72], p<0.001). Notably, the cADHD group and the sADHD group scored similar on psychosomatic problem ([M=1.35, SD=2.00] and [M=1.14, SD=1.37], p>0.999] and anxiety ([M=2.57, SD=2.24] and [M=2.76, SD=2.32], p>0.999), indicating comparable internalizing behaviors in these two groups.
Executive functions of cADHD, sADHD, and HC groups
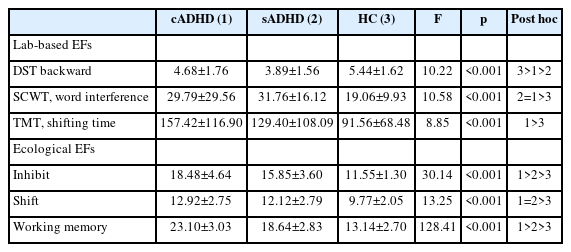
Results of C-WISC, DST, SCWT, TMT, and BRIEF were shown in Table 2. IQ in the three groups were significantly different (all p<0.001). Post hoc analyses showed that the HC group’s IQ was higher than the cADHD group and the sADHD group. In contrast, differences between the cADHD group and the sADHD group were not statistically significant.
For DST, the backward score showed significant difference in the three groups (p<0.001); whereas it is noteworthy that the sADHD group scored the lowest, being significantly lower than the cADHD group ([M=3.89, SD=1.56] vs. [M=4.68, SD=1.76], p=0.015), which was then lower than the HC group ([M= 4.68, SD=1.76] vs. [M=5.44, SD=1.62], p=0.049). For SCWT, we saw significant difference in the word inference score among the three groups (p<0.001). The sADHD group ([M=31.76, SD=16.12] vs. [M=19.06, SD=9.93], p<0.001) and the cADHD group scored higher than the HC group ([M=29.79, SD=29.56] vs. [M=19.06, SD=9.93], p<0.001), while the score of the sADHD group did not differ from the cADHD group (p>0.999). Regarding TMT, while the three groups differed significantly (p<0.001), post hoc analyses located the difference on the cADHD group and the HC group ([M=157.42, SD=116.90] vs. [M=91.56, SD=68.48], p<0.001).
Regarding BRIEF scores, an overall tendency is that the cADHD group scored higher than the sADHD group, which was higher than the HC group. Differences between the three groups were statistically significant (p<0.001). Post hoc analyses showed that while the cADHD group scored significantly higher than the HC group on all three factors, the cADHD group scored significantly higher than the sADHD group on Inhibit ([M=18.48, SD=4.64] vs. [M=15.85, SD=3.60], p<0.001) and Working memory ([M=23.10, SD=3.03] vs. [M=18.64, SD=2.83], p<0.001). Notebly, the Shift score in the sADHD group did not significantly differ from the cADHD group ([M=12.12, SD=2.79] vs. [M=12.92, SD=2.75], p=0.173).
Caregiver strain of cADHD, sADHD, and HC groups
As shown in Table 1, CGSQ scores of the cADHD group, the sADHD group, and the HC group in the three groups were significantly different (p<0.001). Post hoc analyses showed that scores in the cADHD group were significantly higher than the sADHD group, which was then scored higher than the HC group. For example, the score on objective strain in the sADHD group was lower than the cADHD group ([M=1.77, SD= 0.71] vs. [M=2.07, SD=0.83], p=0.008), while higher than the HC group ([M=1.77, SD=0.71] vs. [M=1.15, SD=0.23], p<0.001). Same patterns were seen on scores of internalized subjective strain, externalized subjective strain, and the total score (Table 1).
Relationship between executive functions and caregiver strain in the sADHD group
As shown in Figure 1, the total score of CGSQ was positively correlated with the conduct problem (r=0.42), learning problem (r=0.38), anxiety (r=0.33), and hyperactivity index (r=0.33) in PSQ, as well as Inhibit (r=0.32) and Shift (r=0.35) in BRIEF. In particular, objective strain was positively correlated with the conduct problem (r=0.43), learning problem (r=0.36), impulsive/hyperactive (r=0.32), Anxiety (r=0.37) and hyperactivity index (r=0.40) of PSQ, as well as Shift (r=0.32) in BRIEF. Internalized subjective strain was only positively correlated with the conduct problem (r=0.34) and learning problem (r=0.35) in PSQ, as well as Inhibit (r=0.34) in BRIEF.
Based on above results, we then tested mediation models between executive functions features and caregiver strain factors, taking behavioral problems (factors in ADHD-RS and factors in PSQ) as mediators. As indicated in Figure 2, there was a partial indirect effect of Shift on Objective Strain, mediated by Anxiety (β=0.04, standard error [SE]=0.02, 95% CI=0.01–0.09). Besides, the effects of Working memory on Objective strain (β=0.03, SE=0.01, 95% CI=0.01–0.07), Internalized subjective strain (β=0.04, SE=0.02, 95% CI=0.01–0.09), and Caregiver strain-total (β=0.03, SE=0.01, 95% CI=0.01–0.06), were all fully mediated by Learning problem.
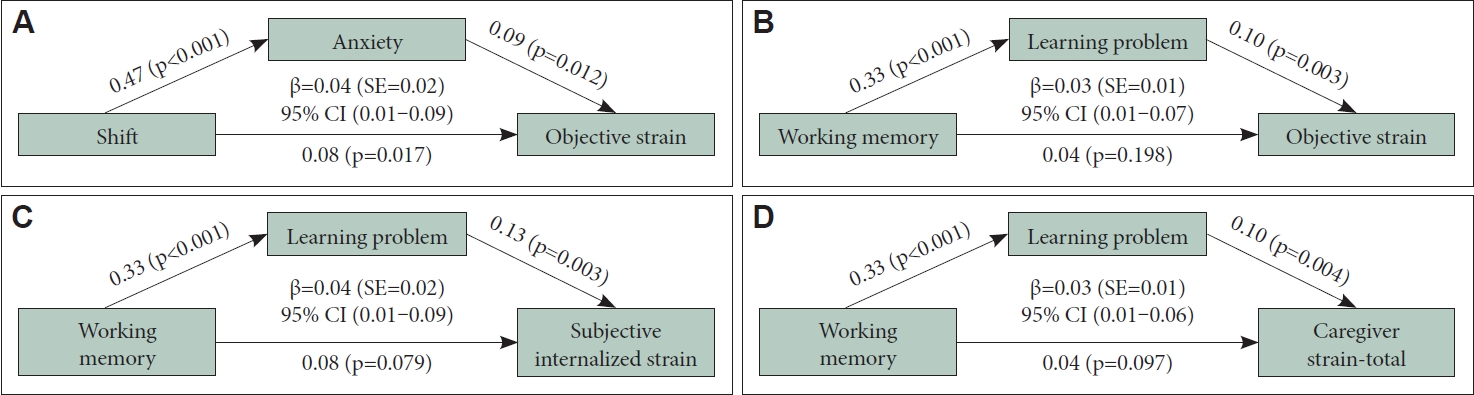
The mediation analyses to explore the potential “executive functions–behavioral problems-caregiver strain” relationship in the sADHD Group. A: The mediation model between shift and objective strain, mediated by anxiety. B: The mediation model between working memory and objective strain, mediated by learning problem. C: The mediation model between working memory and subjective internalized strain, mediated by learning problem. D: The mediation model between working memory and caregiver strain-total, mediated by learning problem. sADHD, subthreshold attention-deficit/hyperactivity disorder; SE, standard error; CI, confidence interval.
DISCUSSION
Our present findings indicated that subthreshold ADHD should be a morbid condition with significant comorbid psychiatric disorders and behavioral problems. Executive dysfunction should not be underestimated in these subjects, as the working memory of sADHD was even worse than cADHD. Besides, caregiver strain seemed to be an obvious issue in sADHD, which was positively correlated with parent-reported measures on behavioral problems and executive functions. A potential explanation on the relationship between executive dysfunction and caregiver strain in sADHD was that executive functions (i.e., working memory and cognitive flexibility) of sADHD increased caregiver strain through the mediation of emotion (i.e., anxiety) and behavior (i.e., learning problems).
Clinical manifestation of sADHD
Consistent with previous studies on subthreshold ADHD, our research demonstrated that a careful clinical interview with parents of sADHD may elucidate multiple comorbid mental disorders including ODD, anxiety disorders, mood disorders, tic disorders, and learning disorders [33,34]. In addition, both clinical interviews and parent-reported questionnaires indicated that while internalizing problems like anxiety and psychosomatic problems may be equally (if not more) common in sADHD, severe externalizing behavioral problems like oppositional defiant problem, conduct problem, or hyperactivity may be less in sADHD than in cADHD.
Our results are partly consistent with previous conclusions that sADHD show more externalizing behavioral problems like conduct problems, when compared to their healthy peers [35-38]. However, we would like to emphasize our results regarding internalizing problems, assuming that problems of sADHD may be more implicit, hidden from the observation of caregivers and doctors. Therefore, a more careful investigation on the subjective wellbeing of sADHD, thorough qualitative approaches like in-depth person-centered interviews or natural environment plays, should be recommended [39].
Executive functions of sADHD
ADHD is a neurodevelopmental disorder, and it is well established that ADHD is related to various cognitive deficits, including cognitive control, reward processing, and timing, throughout developmental stages, including childhood, adolescence, and adulthood [40-42]. Though in controversial, a modern concept of ADHD claimed that executive dysfunction might be an important phenotype of this disorder [43]. In the current study, an overall impression is that parent-rated executive functions of sADHD were poorer than their healthy peers, however better than those with diagnosed ADHD. This phenomenon is consistent with previous studies, showing that cognitive impairments of subthreshold ADHD were similar to ADHD in the pattern but milder in magnitude [17,36,44,45].
According to the results of lab-based tests, sADHD performed equal to cADHD on tasks evaluating inhibition and shifting ability. In particular, the performance of sADHD on the Digit Span Test was even poorer than cADHD, indicating a poorer verbal working memory ability in sADHD. This phenomenon echoes the results of a recently published study in Chinese sADHD, indicating that sADHD exhibited reduced cognitive control efficiency, which was not significantly different from cADHD [45]. In addition, just as indicated in Supplementary Table 1 (in the online-only Data Supplement), the main results regarding groups comparisons of executive functions among cADHD, sADHD, and HC groups remained the same when controlling age, gender, and IQ.
Above all, though not all children exhibit executive dysfunctions, we claim that thorough assessments on executive functions may help to better understand the strengths and limitations of sADHD. Considering executive function training showed satisfactory acceptance and effectiveness not only in cADHD but also in sADHD, we propose that cognitive training tailored upon individual cognitive strengths and weaknesses may also be beneficial for sADHD [46,47]. In particular, results of our study suggest that it makes sense to allocate more lessons on working memory when designing cognitive training programs for sADHD.
Caregiver strain of sADHD
In the current study, caregivers of sADHD reported higher strain, both objective and subjective, than those of normally developed children. This result is parallel to studies in ADHD, indicating that parents of cADHD experience a high level of caregiver strain and a low level of instrumental support, and the most dominant factors loading on parenting stress were children’s behavioral problems and parents’ unmet needs for support [16,48]. Therefore, efforts should be made to support caregivers of sADHD.
By supporting the caregiver strain, we may improve the mental health of both caregivers and children. As demonstrated by studies in children ADHD, while subjective strain of caregivers might influence the development of child externalizing behaviors, interventions targeting parenting distress could alleviate early dysfunctional parent-child interactions and then reduce behavioral problems of children [14,49,50]. We recommend that interventions for parents of cADHD, like the New Forest Parenting Program, family collaboration, and education on effective coping strategies, may be used for reference when developing supporting programs for caregivers of sADHD [51,52].
Potential explanations on the relationship between sADHD and caregiver strain
In sADHD, caregiver strain was positively correlated with parent-reported executive functions. However, despite the significant and severe executive deficits shown in laboratory tests, there is no significant correlation between lab-based executive functions and caregiver strain. Besides, in comparison to internalizing behavioral problems, externalizing behavioral problems were more strongly correlated with caregiver strain. Therefore, we propose that subjective internal bothering and underlying cognitive deficits might be obscured from the observation of caregivers, and the over-reliance on parent reports may lack the power to capture impairments of sADHD sufficiently.
In addition, ADHD symptoms, as evaluated in ADHD-RS, did not show significant correlation with caregiver strain. The above results are in line with previous longitudinal research, demonstrating that functional sequela including ODD and school disciplinary problems, rather than ADHD symptoms, contributed to the lifetime maternal caregiver strain in adolescents and early adults with ADHD [53]. In this sense, interventions directly targeting functional problems, behavioral training for example, should also be recommended [54].
Finally, our results showed that cognitive inflexibility of sADHD increased objective caregiver strain, whose effect was partially mediated through its effect on children’s anxiety problems. In comparison, the impaired working memory of sADHD increased objective and subjective aspects of caregiver strain, which is totally mediated by its effect on learning problems of children. Therefore, our results indicated that executive dysfunction of sADHD, cognitive inflexibility and working memory impairments in particular, can significantly increase caregiver strain, through their effects on emotional and behavioral problems of children.
Strengths and limitations
A strength of the current study is that it profiled the executive functions of sADHD and the strain of their caregivers, which were neglected by previous studies on subthreshold ADHD. Therefore, our study may help clinicians, researchers, and parents to better understand this group of children. Another strength of this study is the adoption of the multi-method approach on executive function evaluation. By doing so, we provided stronger evidence to the conclusion that subthreshold ADHD is associated with executive dysfunctions.
In addition, the adoption of lab-based tests allowed us to reveal a unique phenomenon that sADHD performed even poorer than cADHD on the verbal working memory task. Though our results may lack the power to explain reasons behind this phenomenon, a possible explanation is that the subthreshold ADHD defined in our study may not necessarily a milder type of ADHD. Therefore, when working with children visiting psychiatric clinics for ADHD-like problems, explorations beyond ADHD core symptoms should be considered, and a more detailed examination on cognitive functions may help to understand their existed but hidden impairments.
Some limitations should be considered. Firstly, while our results constructed a mediation model between shift, anxiety, and objective caregiver strain, we suggest that this is one of multiple possible explanations on the relationship between children’s executive functions and the strain of caregivers. Besides, for the cross-sectional nature of this study, as well as the reciprocal relationship between cognitive flexibility and anxiety, we preclude any causal deductions [55]. In addition, both behavioral problems and caregiver strain were evaluated by parents, so we retain the caution that the subjectivity of reporters might bias the results of this study. Finally, the sample sizes of the three groups were not well-matched, which may limit the statistical power of the present study.
To conclude, though clinical symptoms of sADHD did not meet the diagnostic criteria for ADHD, they show significant mental health problems, especially the internalizing behaviors, which may be ignored. The subthreshold ADHD might also exhibit impairments in executive functions, especially in verbal working memory and cognitive flexibility. The executive function impairments may be linked with the internalizing behaviors and further lead to the increase objective strain of the caregivers. We recommend mental health professionals to make a careful examination on mental health problems, executive functions, and parent-child interactions when working with sADHD.
Supplementary Materials
The online-only Data Supplement is available with this article at https://doi.org/10.30773/pi.2023.0070.
Groups comparisons of executive functions among cADHD, sADHD, and HC groups controlling age, gender and IQ
Notes
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Conflicts of Interest
The authors have no potential conflicts of interest to disclose.
Author Contributions
Conceptualization: Yajing Tang, Lu Liu, Qiujin Qian, Yufeng Wang. Data curation: Yajing Tang, Haimei Li, Xinxin Yue. Formal analysis: Yajing Tang, Sunwei Qiu. Funding acquisition: Lu Liu, Qiujin Qian. Investigation: Yajing Tang, Lu Liu, Qiujin Qian, Yufeng Wang. Methodology: Yajing Tang, Lu Liu, Qiujin Qian, Yufeng Wang. Project administration: Yajing Tang, Sunwei Qiu, Haimei Li, Feifei Si, Mengjie Zhao, Min Dong, Meirong Pan, Xinxin Yue. Resources: Lu Liu, Qiujin Qian. Supervision: Lu Liu, Qiujin Qian, Yufeng Wang. Validation: Lu Liu, Qiujin Qian, Yufeng Wang. Visualization: Yajing Tang. Writing—original draft: Yajing Tang. Writing—review & editing: Feifei Si, Mengjie Zhao, Min Dong, Meirong Pan, Lu Liu, Qiujin Qian.
Funding Statement
The National Natural Science Foundation of China (81873802; 81571340), the Capital’s Funds for Health Improvement and Research (CFH: 2022-2-4114), and the National Key Basic Research Program of China (973 program 2014CB846104).