Effects of Online Mindful Somatic Psychoeducation Program on Mental Health During the COVID-19
Article information
Abstract
Objective
This study aims to determine the effects of online mindful somatic psychoeducation program (o-MSP) on mental health in female university students during the coronavirus disease-2019 (COVID-19).
Methods
Thirty-eight female university students were randomly assigned to an intervention group (IG, n=19) or a control group (CG, n=19). IG received o-MSP for 2-hours per session, twice weekly for 4-weeks; CG maintained their usual daily routine for 4-weeks. Measurements were performed pre- and post-intervention to assess stress, anxiety, and social connectedness using Perceived Stress Scale, State-Trait Anxiety Inventory, and Social Connectedness Scale. A qualitative analysis of changes in soma and social connectedness, subjectification of the soma, and mind–body integration was conducted through online interviews.
Results
Regarding stress and social connectedness, there were no significant difference between the groups (p>0.05). However, significant differences were observed in the main effect of time of measurement and time×group interaction, with IG showing significant improvement post-intervention, unlike CG (p<0.05). Regarding anxiety, there were significant differences in the main effect of time of measurement, time×group interaction, and group factor (p<0.05). Post-intervention, CG did not show a significant change, while IG showed a significant decrease (p<0.05). Qualitative analysis revealed that participants experienced “changes in soma and social connectedness,” “subjectification of soma–body,” and “embodiment of mind–body integration,” and reported improved mental health.
Conclusion
The o-MSP effectively reduced stress and anxiety in female university students and improved social connectedness. This suggests that o-MSP can be used to manage the mental health of university students in various settings.
INTRODUCTION
The outbreak of coronavirus disease-2019 (COVID-19) and the resulting lockdown caused various problems related to mental health in university students at a time when they are forming their identities through social activities. Today, most COVID-19-related social restrictions have been lifted worldwide. Nevertheless, university students around the world continue to report psychological problems such as stress, anxiety, depression, frustration, anger, uncertainty, and insomnia caused by COVID-19-related restrictions on interpersonal exchanges [1,2]. Specifically, the lockdown, which was enforced to prevent the spread of severe acute respiratory syndrome-coronavirus-2 (SARS-CoV-2), engendered a sense of loneliness and disconnection and a decreased sense of social connectedness among individuals.
Social connectedness refers to an individual’s psychological sense of belonging. It is a key determinant of an individual’s social and psychological health, because it functions as a buffer against stress and anxiety, and enhances personal well-being [3,4]. This sense of connectedness has decreased as a result of the restrictions on social interactions, and the resulting isolation has reached record levels [5].
Several programs have been proposed in the fields of psychoeducation and psychological intervention to improve the social and psychological health of individuals. These include programs to improve chronic pain [6], anxiety disorders [7], and depression [8] through the process of observing the body and mind, feeling what is experienced [9], and accepting it. These programs are based on “mindfulness,” which is described as the ability to focus attention on the present moment. These meditation programs have effectively reduced negative emotions, including stress and anxiety, in college students [10,11].
Whereas mindfulness is the process of feeling and accepting experiences in the present moment, somatic psychoeducation is a manner of utilizing sensory-motor learning to expand one’s awareness of their bodily movements [12]. Somatic psychoeducation is a form of complementary medicine called “body therapies” and “intuitive restoration of self,” developed based on multidisciplinary theories that emerged from empirical inquiries into the body, breath, and states of being [13]. This somatic psychoeducation increases bodily relaxation [14] and reduces negative emotions in individuals [15]. Based on these findings, a mindful somatic psychoeducation program can improve an individual’s awareness, sensations, happiness, and relationships with others by developing one’s ability to focus on the “here and now” and observing one’s physical and mental healing experienced through movement [16]. However, the effectiveness of this intervention on the mental health of college students remains to be determined.
In May 2023, the World Health Organization and several countries such as Germany, Japan, and the United States declared the end of the COVID-19. However, disease forecasting experts have predicted the recurrence of a similar COVID-like pandemic within 10 years [17,18]. This means that lockdowns may reoccur, and different fields of society demand different responses to help people stay socially active [19,20]. Thus, appropriate online systems and content should be developed.
A study compared the effects of an online movement-based psychoeducation program and a face-to-face movement-based psychoeducation program and reported that the latter had more positive effects on participants’ psychological health [21]. Conversely, another study suggested that online interventions were more effective in increasing participants’ happiness, interest, and engagement than face-to-face interventions [22]. Interestingly, it was also reported that there were no significant difference in the effects of the two psychoeducation modality methods on participants’ learning outcomes [23]. These discrepancies may be due to the differences in the personal and environmental factors of the participants as well as differences in the intervention methods. Thus, further research on the psychoeducation modality method is required. Additionally, it is necessary to develop psychoeducational programs that can cope with various, and dynamic, psychoeducational environments. This study aims to investigate whether the online mindful somatic psychoeducation program (oMSP) can reduce stress and anxiety and improve social connectedness in female university students using quantitative and qualitative analyses.
METHODS
Study design and procedure
The study protocol was approved by the Institutional Review Board of the Sungshin Women’s University (approval number: SSWUIRB-2021-00). The study protocol includes clauses on procedures to safeguard the participants’ rights, safety, confidentiality, recruitment plan, and other guidelines.
The study was designed as a single-blind, randomized controlled trial. Under the blinded condition, measurements were performed before the first intervention (pre) and one day after the last intervention (post), using questionnaires administered equally to the intervention group (IG) and control group (CG). The data were collected through the school’s education system (Learning Management System). Information such as age, name, and date of collection was kept confidential, and all samples were number-coded and anonymized.
Reliance on questions already selected in the quantitative analysis did not allow participants to express their experiences during the intervention freely [24]. Therefore, we conducted a qualitative analysis of participants’ internal experiences of embodiment during the program through open-ended written questions and one-on-one online interviews.
Participants and data collection
A total of 46 students applied to participate in the study, and the research team recruited 38 people considering the selection and exclusion conditions. A total of 38 female college students attending the Sungshin Women’s University were recruited and randomly assigned to the IG (n=19) or CG (n=19). Information regarding recruitment of participants was promoted through school bulletin boards and social networking sites (Everytime, Facebook, etc.) for approximately 15 days in January 2021. A total of 38 students who satisfied the inclusion and exclusion criteria finally participated in this study voluntarily. All participants signed a written informed consent via email before participation in the study. The researchers thoroughly explained the experimental procedures, objectives, and precautions to all participants before participating in the research, and informed them that they could withdraw from the study at any time.
The inclusion criteria for this study were: 1) not having problems with the musculoskeletal system, 2) not having problems with the cognitive function, 3) not exercising regularly, that is, more than three-times a week, and 4) not undergoing medication for mental problems. The exclusion criteria were: 1) underweight or morbid obesity (body mass index <18 or >40), 2) current or former smokers (in the past 12 months), and 3) participating in any other program [25,26].
The sample size was selected based on similar studies and methods using G*Power 3.1.9.7 (Heinrich Heine University, Dusseldorf, Germany). Based on this test, at least 32 participants with an anticipated statistical power of 0.95, an α-error probability of 0.05, and an effect size of 0.03 were required for this study. For example, Muzik et al. [27] obtained positive results on depression and mindfulness with 18 participants in an experimental group in a mindfulness yoga intervention. Additionally, in a study on the effects of a yoga intervention on high school students’ emotional control [28], the experimental and CGs included 19 participants each. Considering the number of participants in these studies and a 20% drop-out rate, this study recruited 19 participants each for the IG and CG.
Intervention
The IG participated in the real-time o-MSP program using Zoom for two hours per session, twice a week, for four weeks. The CG was a standby group, provided with a video after the program was finished. During the session, the researcher verified the movements of the participants through a webcam and corrected inappropriate or insufficient movements. The program was performed by a professor who has been practicing and researching meditation and yoga for more than 15 years, has completed Somatics by Thomas Hanna, and has been teaching and researching intervention-related subjects for more than 20 years. After the researcher constructed the program, a psychiatrist with more than 20 years of clinical experience and a doctoral degree checked and finalized the content, and it was operated under his supervision.
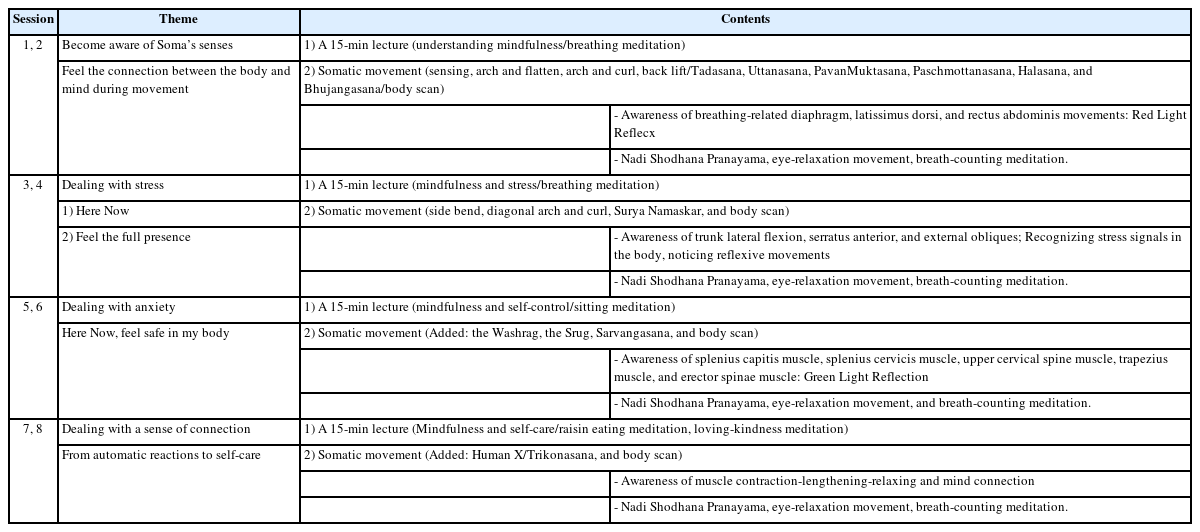
The program was based on the researcher’s practice and teaching process (Thomas Hanna’s Somatics, Korean Mindfulness-Based Stress Reduction [K-MBSR], Mindfulness Yoga, etc.), research, and references [29-31]. The o-MSP program comprised mindfulness practice, followed by a somatic movement to feel the sensation (spaciousness, weight, etc.) of the body in contact with the floor (Table 1). Somatic movements comprised Hanna’s Somatics and yoga-based movements, body scan, Nadi Shodhana Pranayama, eye-relaxation movements, and breath-counting meditation. The researcher instructed the participants to perform movements to correct stress-induced postural changes after explaining the Sensory Motor Amnesia.
Postural distortion caused by psychological distress induces a withdrawal response, which, when repeatedly triggered, results in a lordotic posture due to an increased tension pattern in the abdominal muscles, known as the Red Light Reflex. The postural distortion induced by eustress is an action response that, when frequently triggered, tends to maintain a kyphotic posture by contracting and tensing the muscles at the back of the body, called the Green Light Reflex [32]. Therefore, the exercises reflected contraction and relaxation of the flexors at the front of the body to relieve the Red Light Reflex and contraction and relaxation of the extensors to relieve the Green Light Reflex. The researcher instructed the participants to be aware of the following: their breathing during each movement; the sensory perception of the muscle contracting, lengthening, and relaxing; and the feeling or embodiment in the body and mind.
Measurement
Perceived Stress Scale
Stress was measured using the Perceived Stress Scale (PSS) developed by Cohen et al. [33] and revised into a short form by Cohen and Williamson [34]. The questionnaire comprises 10 items (e.g., “In the last month, how often have you been upset because of something that happened unexpectedly?”). Each item was rated on a 5-point Likert scale ranging from 0 (never) to 4 (very often). The PSS includes the following two factors: Perceived Self-Efficacy, comprising positively phrased items (PSS-PPI), and Perceived Helplessness, comprising negatively phrased items (PSS-NPI) [35]. Internal consistency between items (Cronbach’s α) was 0.858.
State-Trait Anxiety Inventory
Anxiety was measured using the State-Trait Anxiety Inventory (STAI) developed by Spielberger [36] and adapted into Korean by Kim and Shin [37]. This 40-item questionnaire comprises 20 state anxiety (e.g., “I am tense;” STAI-X1) and 20 trait anxiety (e.g., “I feel nervous and restless;” STAI-X2) items. Each item was rated on a 5-point Likert-type scale ranging from 1 (not at all) to 5 (mostly). Internal consistency between items (Cronbach’s α) was calculated at 0.934 for state anxiety and 0.901 for trait anxiety.
Social Connectedness Scale
Social connectedness was measured using the Social Connectedness Scale (SCS) developed by Summer et al. [38]. This 16-item scale has two factors: social connectedness and classroom connectedness. This study used only the 12 social connectedness items (e.g., “I feel disconnected from campus life”). Each item was rated on a 6-point Likert-type scale ranging from 1 (strongly disagree) to 6 (strongly agree). Internal consistency between items (Cronbach’s α) was 0.894.
Written questions and one-on-one online interviews
To assess the participants’ experiences of the mindful somatic yoga program, they were given open-ended written interview questions: “What did you experience in the process of participating in the program, for example, the alleviation of discomfort or any other changes, if any?”; “What physical and psychological experiences did you have?”; and “What did you experience while participating online in the program with peers?” Similarly, one-on-one online interviews were conducted synchronously after the program’s completion.
Statistical analysis and assurance of rigor
The data collected using stress, anxiety, and social connectedness questionnaires were analyzed using IBM SPSS Statistics 21.0 (IBM Corp., Armonk, NY, USA). Specifically, inter-item internal consistency analysis, independent sample t-test, descriptive statistics analysis, and two-way repeated measures analysis of variance (ANOVA) were performed. The level of significance for all results was set at p<0.05.
This study employed Giorgi’s [39] phenomenological lens for analyzing the data collected through interviews to ascertain and interpret the discomfort experienced by university students during the COVID-19 lockdown and their firsthand experience of embodiment while participating in the program. The data derived from the interviews were transcribed and anonymized, and the qualitative data were classified via inductive content analysis. Additionally, the rigor and ethical standards of the collected data were ensured by consulting yoga professionals and sports psychology professors who were not involved in this study.
RESULTS
General characteristics
Of the 46 volunteers, seven did not meet the inclusion criteria and one refused to participate. Thus, a total of 38 individuals participated, and none dropped out over the next eight weeks of the study (Figure 1).
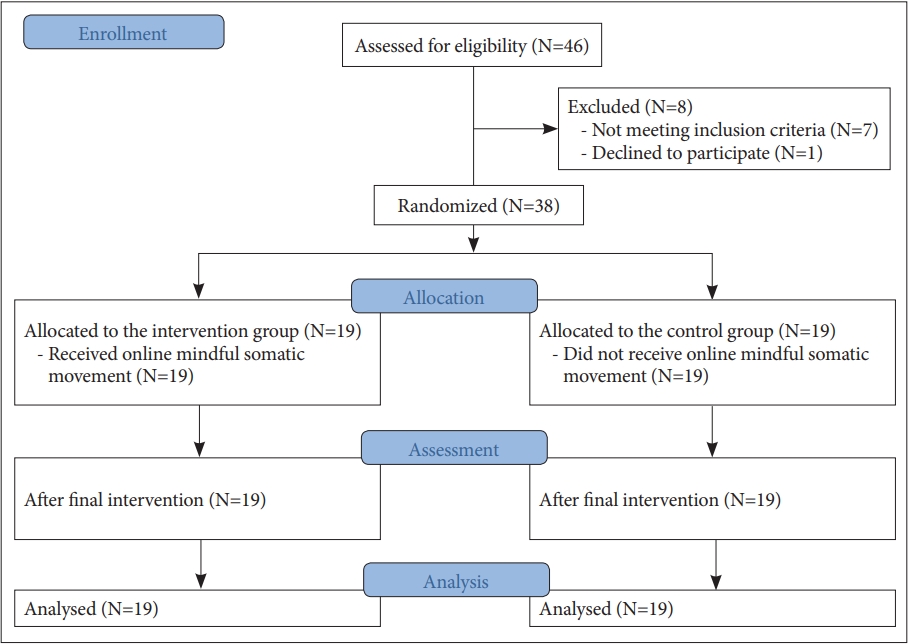
CONSORT chart. This flow diagram represents an experimental procedure. CONSORT, Consolidated Standards of Reporting Trials.
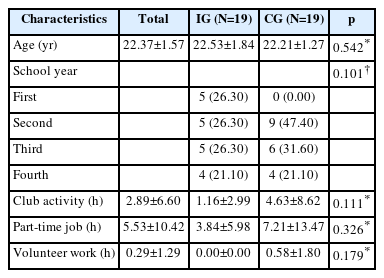
There were no significant difference in general characteristics such as age, school year, race, club activity, part-time job, and volunteer work between the IG and CG (Table 2). Additionally, the two groups had no significant difference in terms of the baseline values of quantitative variables such as stress, anxiety, and social connectedness (Table 3).
Quantitative analysis results
Stress
Table 3 shows that although there was no significant difference between groups in the PSS-PPI (F(1, 36)=2.765, p=0.105), there were significant differences in the main effect of time of measurement (F(1, 36)=10.865, p=0.002) and time×group interaction (F(1, 36)=17.171, p<0.001). In particular, the IG showed a statistically significant decrease in stress from 8.95±2.68 at pre-intervention to 4.79±2.44 at post-intervention (t=4.336, p<0.001).
Similar to the PSS-PPI, there was no significant difference between groups in the PSS-NPI (F(1, 36)=2.922, p=0.096). However, the main effect of time of measurement (F(1, 36)=14.406, p=0.001) and time×group interaction (F(1, 36)=18.191, p<0.001) showed significant differences. Additionally, the IG showed a significant change from 17.79±4.80 to 12.37±3.45 before and after intervention, respectively (t=5.009, p<0.001), while the CG did not show a significant change (p>0.05).
The PSS-Total also showed no significant difference between groups (F(1, 36)=3.591, p=0.66). However, the main effect of time of measurement (F(1, 36)=15.899, p<0.001) and time×group interaction (F(1, 36)=22.125, p<0.001) showed significant changes. The IG also showed a significant decrease of 9.58±8.06 from 26.74±6.67 before intervention to 17.16±5.33 after intervention (t=5.182, p<0.001).
Anxiety
As a result of analyzing the change patterns of anxiety between the IG and CG over time, there were significant differences between groups in state anxiety, trait anxiety, and total anxiety (state anxiety (STAI-X1): F(1, 36)=8.3, p=0.007; trait anxiety (STAI-X2): F(1, 36)=4.314, p=0.045; total anxiety (STAI): F(1, 36)=6.653, p=0.014). Additionally, there were significant differences in the main effect according to the main effect of time of measurement (STAI-X1: F(1, 36)=26.935, p<0.001; STAI-X2: F(1, 36)=25.058, p<0.001; STAI: F(1, 36)=31.349, p<0.001) and time×group interaction (STAI-X1: F(1, 36)=19.789, p<0.001; STAI-X2: F(1, 36)=20.491, p<0.001; STAI: F(1, 36)=24.04, p<0.001).
In particular, anxiety showed a statistically significant improvement post-intervention compared to pre-intervention in the IG. Specifically, state anxiety decreased from 53.95±9.88 to 38.21±7.18 (t=6.248, p<0.001), and trait anxiety decreased from 54.53±7.35 to 44.05±6.95 (t=7.069, p<0.001). Total anxiety showed a significant improvement from 108.47±15.99 to 82.26±13.6 (t=6.248, p<0.001) (Table 3).
Social connectedness
Connectedness did not show a significant change between groups (F(1, 36)=1.96, p=0.17), as did the change in stress. However, the main effect of time of measurement (F(1, 36)=19.674, p<0.001) and time×group interaction (F(1, 36)=23.745, p<0.001) showed significant differences. Moreover, unlike the CG, IG showed a significant improvement of -7.84±5.63 in social connectedness from 38.53±7.24 at pre-intervention to 46.37±4.87 at post-intervention (Table 3).
Qualitative analysis results
Changes in the soma and social connectedness
Physical soma
The COVID-19 lockdowns had imposed restriction on physical movement of individuals. Most participants experienced improvements in bodily flexibility, lung capacity, posture correction, body balance, pain relief, digestion, and sleep quality after participating in the o-MSP program (Supplementary Table 1 in the online-only Data Supplement).
Psychological soma
Participants stated feeling frustrated and isolated because of restrictions on school life and venturing outdoors. However, after participating in the o-MSP program, they expressed that their lethargy, depression, tension, anxiety, stress, and obsessive thoughts gradually decreased. They could think about other things. Additionally, they regained inner stability and comfort, which enabled them to focus on themselves (Supplementary Table 1 in the online-only Data Supplement).
Embodiment of social soma
Most students felt that the lockdown significantly restricted their social connectedness and complained about this stifling situation. However, they reported that the o-MSP program enabled them to experience a sense of connectedness with the university, or “the experience of social-soma, of being a social being” in a situation where they were not allowed residence on campus. Additionally, they experienced comfort, security, encouragement, and intimacy through social connectedness (Supplementary Table 1 in the online-only Data Supplement).
Changes in the subjectification of the soma
Mindfulness
Participants engaged in self-reflection while organizing their thoughts, and mindfulness was observed after participating in the program (e.g., forgetting about one’s appearance and movement, self-illustration, and accepting the futility of worrying and utility of unconditional acceptance of reality). During the body scan, they became aware of their nonchalant and neglectful attitudes about their body, and we observed mindfulness was induced in most of them (Supplementary Table 2 in the online-only Data Supplement).
Self-regulation
Online classes encouraged changes in students’ daily life patterns. Participants reported increased self-confidence regarding practicing mind control, converting negative thoughts into positive ones, and applying breathing to everyday life situations for mood adjustment. Thus, it can be inferred that they learned to control their feelings and moods (Supplementary Table 2 in the online-only Data Supplement).
Changes in the mind-body integration
Breath-mind connectedness
Participants experienced a feeling of being relaxed, calm, and pacified while focusing on breathing, and many students experienced that their thoughts and worries faded away during this process. Additionally, they learned how to calm their mind in stressful situations. In particular, their experiences of the connectedness of breath and mind suggests that they experienced mind–body or holistic integration (Supplementary Table 3 in the online-only Data Supplement).
Intentional movement–mind connectedness
When participants focused on intentional body movements and breathing while participating in the mindful somatic program, they realized that the body and mind/soul are one and that they all are the self. Additionally, they experienced that while moving their bodies, they felt physically and mentally less stifled, their minds refreshed, their moods lifted, and their depression eased. Furthermore, the experiences of feeling the back straightened and the presence of the spine while performing the o-MSP program, and gain in confidence were observed—these constitute the moments of body rehabilitation. These experiences enabled them to vividly feel that their body was alive through sensory-motor coupling, body rehabilitation, and healing (Supplementary Table 3 in the online-only Data Supplement).
DISCUSSION
This single-blind, randomized controlled trial investigated the effects of the o-MSP program on mental health in female university students during the COVID-19. The findings of this research are discussed below.
First, the o-MSP program can effectively reduce the stress caused by the lockdown. As Table 3 shows, in the IG, unlike the CG, the PSS was significantly decreased after the intervention. This implies that female university students perceived lower stress induced by lockdown. These results support the findings of Luberto et al. [40] who found that students who participated in an online mindfulness course during the COVID-19 pandemic could cope well with pandemic stress by experiencing focus, gratitude, and acceptance. The results also concur with that of another study that reported a reduction in the stress hormone cortisol in participants of a mindfulness-based exercise program [41].
Previous studies have reported that physical training, meditation, and somatic movement can reduce stress hormones [42] and alleviate disease-related stress, depression, and anxiety [43]. However, most of these studies have conducted face-to-face interventions and questioned the effectiveness of non-face-to-face training [22]. This study is significant because it confirms that stress can be meaningfully improved through an o-MSP program and suggests an effective stress management mechanism.
Second, significant differences in state and trait anxieties were observed between the IG and CG. This implies that the o-MSP program effectively reduced anxiety in female university students. These results support studies showing that participants who undergo mindfulness training exhibit lower levels of cognitive and somatic anxieties in an acutely stressful situation compared to controls [44], and that mindfulness-and acceptance-based interventions are associated with substantial alleviation of anxiety [45].
Third, regarding social connectedness, although there was no difference between groups, the CG showed no significant change after the intervention, while the IG exhibited a significant improvement of 7.84±5.63 (Table 3). This suggests that the o-MSP program improved the social connectedness among female students who had attended online lectures for the entire year because of the COVID-19 lockdowns. The results of this study are in line with the findings of previous studies that state that mindfulness leads to improved interpersonal relationships through the mediation of social connectedness [46] and that there is a positive correlation between mindfulness and social connectedness [47]. Movement-based psychoeducation programs with other people are not just about the individual, but also about sharing a sense of connection and experience with others, which is known as non-verbal shared consciousness [48]. We believe that the online psychoeducation method used in this study is a concrete example of this effect [49], which can reduce the social distance felt by individuals and promote the community spirit of participating students [50].
Finally, the qualitative analysis of the interviews with the participants regarding the effects of the program revealed the following categories: change in the soma and social connectedness, subjectification of the soma (mindfulness, self-regulation, etc.), and mind–body integration (breath–mind connectedness and intentional movement–mind connectedness).
Changes in soma and social connectedness
The participants embodied their experiences of physical change in flexibility, lung capacity, posture correction, pain relief, digestion, and sleep quality. This result supports the results of studies that reported experiences of reduced joint pain and fatigue, maintenance of correct posture, improved sleep quality, and increased physical activity through movements based on the somatic approach [51-53].
The participants embodied psychological soma, experiencing psychological stability and comfort that facilitated easy and unhindered self-reflection, thanks to reduced lethargy, depression, tension, anxiety, and stress. Additionally, it is in accordance with studies that have reported that mindfulness reduces negative emotions [52,54] and alleviates physical symptoms induced by anxiety, depression, and stress [55].
The participants also felt a sense of affiliation. In the process of sharing common topics, discussing their bodies and minds, sharing with others, and empathizing with others’ stories, a sense of affinity and unity was evoked, forming a community. Students experienced empathy, felt human universality, and embodied the social soma existing among people. This finding supports the findings of those studies that have reported that o-MSP classes contribute to creating an environment of unconditional mutual acceptance and forming social connectedness by familiarization with one another [51].
Subjectification of the soma
This category was classified into mindfulness and self-regulation. The participants experienced body-related mindfulness by realizing the need to be aware of and caring for the body. This was in line with the results of previous studies that reported that mindfulness training can promote the acceptance of one’s experiences and facilitate dis-identification with inner experiences by encouraging the detached observation of emotions [56]. According to Cox and Tylka [57], mindfulness-based exercises can minimize self-objectification and improve related outcomes by focusing attention on bodily functions and sensations. In other words, residing in the body implies communicating with the world from a first-person perspective rather than a third-person (i.e., observer) perspective.
Mind–body integration
Participants experienced “mind–body integration” through “breath–mind connectedness” and “intentional movement–mind connectedness.” An embodiment of breath–mind connectedness implies that participants experienced comfort, calmness, and detachment from disturbing bad thoughts and worries while focusing on breathing. Participants directly embodied lowered depression and change in mood and emotions amid body movements. They realized that the body and mind/soul unify when focused attention is given to breathing and that they all comprise the self. These results support the findings of previous studies that have reported that physical movement positively affects mood, emotion, and consciousness [24].
The opinions of these participants can provide empirical evidence for the claim that mind–body integration can be achieved through two pathways. First, the bottom-up pathways, in which peripheral somatic information influences neural processing and mental activity via ascending neural transmission to the brainstem and cerebral cortex when an individual focuses on breathing and bodily sensations. Second, through top-down pathways, which are activated by focused attention and relaxation intention at the level of the cerebral cortex [58].
Limitations
The limitations of this study are as follows. First, the participants were those who could volunteer to participate in the program during their vacations and were from a women’s university. Therefore, they do not represent all university students. Second, there is a limitation related to gender because only female students participated. Third, the small sample size limits the generalizability of our findings. Fourth, the study only measured pre-and post-intervention. As a result, the duration of the positive effects of o-MSP on mental health could not be clearly determined. Fifth, we could not conduct the intervention face-to-face due to social constraints, so we cannot identify differences in effectiveness between face-toface and non-face-to-face programs.
Further studies should conduct mixed-gender group studies considering the gender, race, and age of the participants and expand the sample size to represent the characteristics of the general population better. It is also necessary to conduct a follow-up measurement to determine the duration of the o-MSP effect. Finally, further research should also compare face-to-face classes, online classes, and a mix of both to identify differences in effectiveness based on the type of class delivery.
Conclusions
In this study, the o-MSP program reduced the stress and anxiety and enhanced social connectedness in university students. The analysis of the interviews with the participants revealed that they experienced: 1) changes in physical and psychological soma and the embodiment of social soma through their moving bodies, 2) soma–body subjectification through mindfulness and self-regulation, and 3) breathing and intentional movement as connected to the mind, so that mind–body integration could be achieved. Additionally, they recovered a sense of presence through the embodiment of social connection experiences between people transcending space. This study did not identify an effectiveness advantage between the online and face-to-face modalities of the mindful somatic psychoeducation program. However, we suggest that by identifying the effects of the online implementation of the program on the promotion of mental health, online somatic-based psychoeducation programs can be effectively used in various social settings in the future.
In this study, the following suggestions are made for somatic-based psychoeducation for patients who complain of distraction, distortion of sensory perception, hyperarousal, and derealization, including confusion of spatial and spatial concepts. It is a somatic-based “intentional-breathing-attention-movement psychoeducation” that cultivates awareness of interoception, proprioception, and kinesthetic awareness and recognizes body index/maps. We suggest that these psychoeducation interventions in this study could help patients stop negative thoughts and restore their sense of cognitive distortions so that they can stay fully here and now.
Supplementary materials
The online-only Data Supplement is available with this article at https://doi.org/10.30773/pi.2023.0304.
Qualitative analysis of changes in the soma and social connectedness following the online mindful somatic psychoeducation
Qualitative analysis of changes in subjectification of the soma following the online mindful somatic psychoeducation
Qualitative analysis of changes in the mind-body integration following the online mindful somatic psychoeducation
Notes
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Conflicts of Interest
The authors have no potential conflicts of interest to disclose.
Author Contributions
Conceptualization: Young Sook Yook. Data curation: Inkyoung Park, Hwi-young Cho. Formal analysis: Inkyoung Park, Hwi-young Cho. Funding acquisition: Young Sook Yook. Investigation: Young Sook Yook, Inkyoung Park, Hwi-young Cho. Methodology: Young Sook Yook, Jae-Hon Lee. Project administration: Young Sook Yook. Resources: Young Sook Yook, Jae-Hon Lee. Supervision: Young Sook Yook. Validation: Jae-Hon Lee, Hwi-young Cho. Visualization: Inkyoung Park, Hwi-young Cho. Writing—original draft: Young Sook Yook, Inkyoung Park, Hwi-young Cho. Writing—review & editing: Young Sook Yook, Jae-Hon Lee.
Funding Statement
This work was supported by the Sungshin Women’s University Research Grant of 2020.
Acknowledgements
All authors would like to express our gratitude to both groups of students who faithfully participated until the end of this experiment.