Impaired Empathic Abilities among Patients with Complex Regional Pain Syndrome (Type I)
Article information
Abstract
Objective
The aims of this study were to evaluate differences in empathic abilities between patients with complex regional pain syndrome (CRPS) Type I and healthy control subjects (HCs) and to assess correlations between empathic abilities and multidimensional aspects of pain.
Methods
Empathic ability was measured in 32 patients with CRPS Type I and in 36 HCs using the Interpersonal Reactivity Index (IRI). A comprehensive assessment of pain was conducted in the patient group using the West Haven-Yale Multidimensional Pain Inventory (WHYMPI). Psychiatric symptoms were assessed using the Beck Depression and Anxiety Inventories (BDI and BAI), and quality of life was evaluated using the WHO Quality of Life (WHOQOL-BREF) questionnaire.
Results
Patients with CRPS showed impaired cognitive and emotional empathic abilities compared with HCs. Significantly lower levels of perspective taking and empathic concern and higher levels of personal distress on the IRI were exhibited by the patient group. Perspective taking and personal distress were associated with affective distress and poor quality of life in social contexts (BDI, BAI, and WHOQOL). However, empathic concern was positively correlated with pain severity and social support from others (WHYMPI).
Conclusion
A tendency toward self-oriented distress in social cognition was exhibited among patients with CRPS Type I. Impaired empathic ability was shown to have potentially negative effects on subjective emotional outcomes and social performance in the lives of patients. Interventions to improve emotional awareness and theory of mind would be beneficial for enhancing social functioning in patients with CRPS Type I.
INTRODUCTION
Complex regional pain syndrome Type I (CRPS I), formerly known as reflex sympathetic dystrophy (RSD), is a medical condition characterized by chronic and distressing neuropathic pain manifested in sensory, autonomic, trophic, and motor abnormalities.1 The nature of the pain is non-dermatomal, and it is often associated with allodynia.2 The severity of pain experienced by patients with CRPS is known to be the highest among all diagnostic pain conditions, as measured by the McGill Pain Questionnaire.34 The pain, which is localized to one or more extremities (the arm, hand, leg, or foot), may result in functional impairment of the affected limbs, subsequently causing severe disability with respect to the activities of daily life and significantly interfering with quality of life.5
As is well known to be the case with other forms of chronic pain disease, CRPS is associated with negative psychological outcomes such as increased depression and anxiety,6 and compromised cognitive functioning such as impaired attentional capacity and processing speed.7 Imaging studies in patients with CRPS have shown abnormalities in brain structure and functioning in regions associated with emotion, autonomic functioning, and pain perception.89 These regions include the ventromedial prefrontal cortex, the anterior insula (AI), and the anterior cingulate cortex (ACC), which plays a role in understanding others' emotional states and feeling empathy for the pain of others,10 suggesting possible impairment in social cognitive functioning, especially with regard to empathic ability, among patients with CRPS.11 Previous research has demonstrated deficits among patients with CRPS in perceiving the emotional and mental states of others, particularly as they relate to pain affect.12
Empathy, defined as the "reactions of one individual to the observed experiences of another," is an essential ability for social functioning, and it has been described as multidimensional in nature, consisting of both cognitive and emotional components.13 Impaired empathic ability is known to be associated with dysfunctional social behaviors and personal distress in social interactions13 and it has been reported in various psychiatric disorders such as autism,14 schizophrenia,15 mood disorder,16 alcoholism,1718 personality disorders,1920 and traumatic brain injury.2122 Impaired empathic ability in PTSD has been recently reported, with patients afflicted by PTSD showing lower levels of empathic concern and perspective taking along with higher levels of personal distress on the Interpersonal Reactivity Index (IRI).2324
Considering the subjectivity of chronic pain, understanding how patients experience pain and communicate it with others is crucial in clinical practice for accurate evaluation and treatment planning. Within this context, Turk and Kerns have emphasized the multidimensional quality of chronic pain, suggesting that pain assessment should include an evaluation of patients' perception of pain and the meaning of pain for them, an evaluation of their physical, emotional, cognitive and behavioral responses to pain, an evaluation of the impact of pain on different aspects of their lives (e.g., vocational, social, and marital, as well as physical), the responses of significant others to their pain, and an assessment of coping strategies employed.25
Given that empathy plays a key role in social interactions, empathic ability in patients with chronic pain may influence their interaction with clinicians, the social support they receive from family or caregivers, their social functioning, and their quality of life in interpersonal contexts. In contrast to the abundant emphasis placed on others' empathy (e.g., clinicians, caregivers, and spouses) in the evaluation and management of patients with chronic pain,2627282930 little attention has been focused on the empathic abilities of the patients themselves. Noll-Hussong et al.31 has reported that patients with chronic pain disorder show disturbances in their ability to imagine how others would feel in particular painful situations. The patients reported significantly lower scores on the Empathic Concern subscale of the IRI, accompanied by lower activation of the left perigenual ACC compared with healthy controls.
To our knowledge, the present study is the first to evaluate the empathic ability of patients with CRPS Type I and its correlation with multidimensional aspects of pain. We hypothesized that patients with CRPS would show impaired empathic ability compared with healthy controls. Additionally, we assessed patients with respect to emotional distress, multidimensional measures of pain, and clinical behaviors to evaluate their association with empathic ability.
METHODS
Subjects
Forty-one patients with CRPS were recruited from the Pain Clinic of Seoul National University Hospital (SNUH), and 17 from a CRPS support organization in Korea. All patients had their diagnosis confirmed by a board-certified anesthesiologist based on the criteria of the International Association for the Study of Pain.32 Of a total number of 58 patients, 46 were eligible to participate, with 12 excluded due to their having been diagnosed CRPS Type II rather than Type I. After excluding 14 additional patients due to missing data, we analyzed data from 32 patients (19 men, 13 women). Twenty-four patients from the SNUH Pain Clinic were given self-report questionnaires in printed form, and eight patients from the CRPS support organization completed the same self-report questionnaire online. The Structured Clinical Interview for DSM-IV-Disorders Axis I Disorders (SCID-I)33 was used to identify neuropsychiatric comorbidities in patients from the SNUH Pain Clinic; comorbidities for patients from the CRPS support organization were identified by self-report. Medication was reviewed for all patients, and opioids were converted to oral morphine equivalent doses.34 Thirty-six normal healthy controls (18 men, 18 women) were recruited through internet advertisements. None of these had a history of hospitalization, and none was currently taking any medications.
This study was approved by the Institutional Review Board (IRB) at Seoul National University Hospital (Seoul, Korea). All data were obtained under written informed consent granted by all subjects after a full explanation of the experimental methods; medical records were treated anonymously.
The Interpersonal Reactivity Index
Empathic ability was measured using the IRI. The IRI is a multidimensional scale composed of 28 self-report items measuring cognitive and emotional dimensions of empathy.1335 There are four subscales of the IRI, with the Perspective-taking and Fantasy subscales representing a cognitive dimension, and the Empathic Concern and Personal Distress subscales representing an emotional dimension. Each subscale consists of seven items, and the total scores for each subscale range from 0 to 28. The Fantasy (FS) scale assesses the tendency to imaginatively transpose oneself into the feelings and actions of fictitious characters in books, movies, and plays, and the Perspective-taking (PT) scale measures the tendency to take the psychological point of view of others. The Empathic Concern (EC) scale measures feelings of sympathy and concern for others, and the Personal Distress (PD) scale assesses self-oriented anxiety upon observing others in distress. The IRI has been demonstrated to have good reliability and validity, and it has been translated into a Korean version that has been proven valid. Each subscale was analyzed as single variable.36
The West Haven-Yale Multidimensional Pain Inventory
A comprehensive assessment of pain was conducted in patients with CRPS using the West Haven-Yale Multidimensional Pain Inventory (WHYMPI). The WHYMPI provides a multidimensional assessment of the subjective experience of pain from a cognitive-behavioral perspective.25 Higher scores on the WHYMPI indicate more severe pain. The 52 items are categorized into three parts. Part I consists of subscales measuring pain severity (PS), pain-related interference (I), social support from others (S), patients' perception of their degree of life control (LC), and affective distress (AD). Part II evaluates patients' perceptions of the responses of significant others to their communication of pain, which are classified as punishing (PR), solicitous (SR), or distracting responses (DR). Part III assesses five domains of activity: household chores, outdoor work, activities away from home, social activities, and general activity (GA). All of the subscales except those in Part III were handled as a single variable, and from Part III, only general activity was included in the analysis. Patients' MPI responses were scored and classified using MPI Software Version 3.0.37 The reliability and validity of the WHYMPI measures have been well established, with broad support for their efficacy in assessing the overall adjustment of chronic pain patients and outcomes of treatment interventions.38394041424344
Psychological profiles
Symptoms of depression and anxiety were evaluated in both the patient and control groups using the Beck Depression Inventory (BDI-I)45 and the Beck Anxiety Inventory (BAI),46 each composed of 21 items (score range, 0-63). Quality of life was assessed using the WHO Quality of Life Scale Abbreviated Version (WHOQOL-BREF).47 Of the six subdomains of the WHOQOL-BREF, we included in our analysis those representing physical health, psychological health, social relationships, and environment; overall quality of life and general health were excluded due to their narrow score ranges (1-5). The Korean version of the WHOQOL-BREF, developed by Kim et al., has demonstrated reliability and validity.48
Statistical analysis
The SPSS software (v. 22.0; SPSS, Chicago, IL, USA) was used for data analysis. Differences in age, education, IRI scores, and psychological profiles between the patient and control groups were assessed using a Student's two-tailed t-test for independent samples, and differences in gender distribution were analyzed using a chi-square test for independent samples. An analysis of covariance was used to adjust for age, years of education, and gender in group comparisons. A Pearson correlation analysis was used to evaluate the association between the subscales of the IRI and the WHYMPI, and a Pearson's partial correlation analysis was used to correct for age, gender, and years of education. The p-value deemed to indicate significance was set at 0.05.
RESULTS
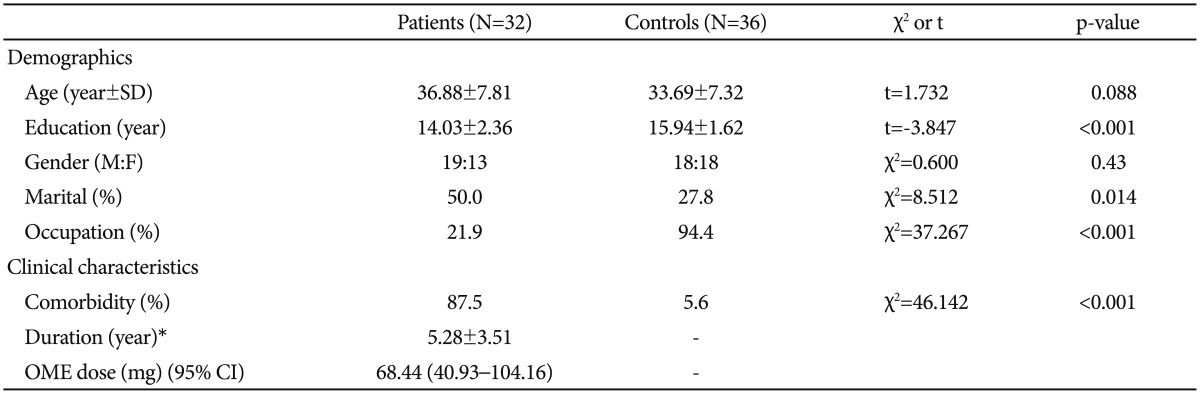
Twenty-eight patients (87.5%) had comorbid Axis I psychiatric disorders, including major depressive disorder (n=19), anxiety disorder (n=5), depressive disorder due to general medical condition (n=3) and bipolar disorder not otherwise specified (n=1). Patients were taking various forms of medication, including opioid analgesics (i.e., buprenorphine, fentanyl, hydromorphone, morphine, oxycodone, tramadol), non-opioid analgesics (i.e., acetaminophen, zaltoprofen), anticonvulsants (i.e., gabapentin, phenytoin, pregabalin, valproic acid), mood stabilizer (i.e., lithium), antidepressants (i.e., bupropion, duloxetine, escitalopram, milnacipran, mirtazapine, nortriptyline, tianeptine), antipsychotics (i.e., aripiprazole, olanzapine, quetiapine), anxiolytics (i.e., alprazolam, clonazepam, etizolam, lorazepam), and hypnotics (i.e., trazodone, triazolam, zolpidem). There were no significant differences in demographic characteristics between the patient and control groups, with the exception of education, with the patient group reporting fewer years of education than the control group. The basic demographic and clinical characteristics of all subjects are provided in Table 1.
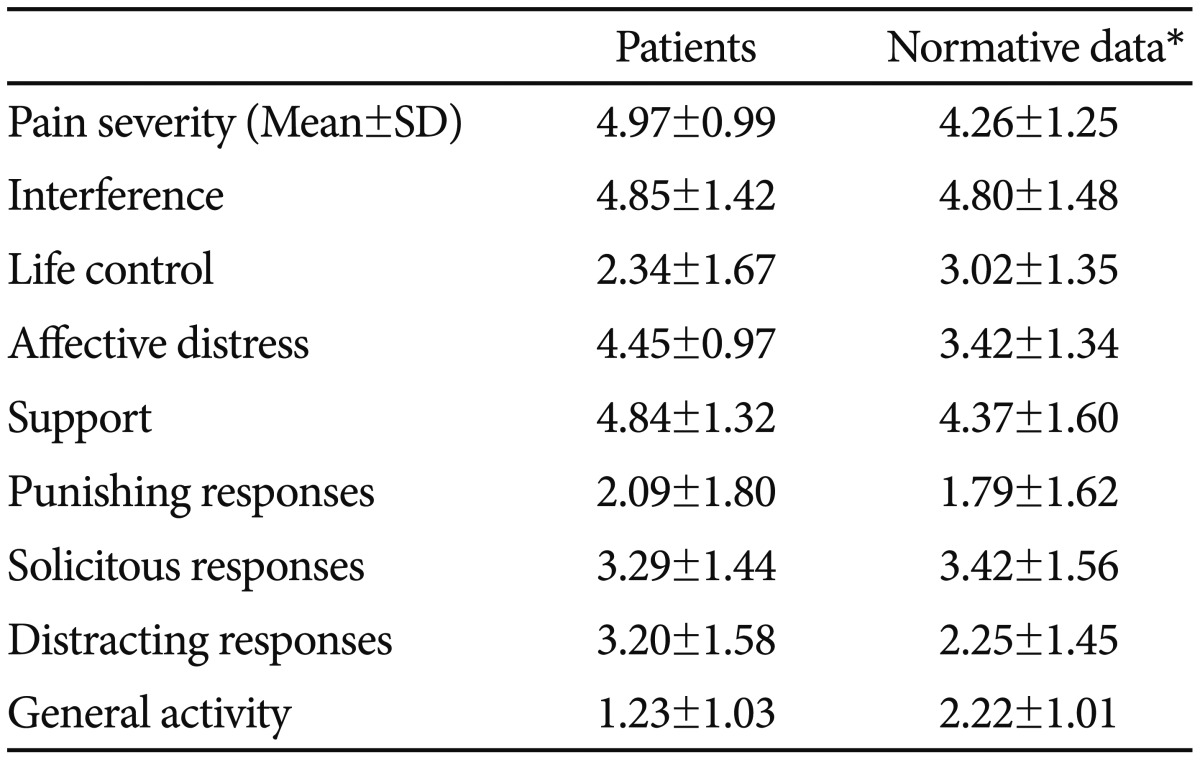
The results of pain assessment in the patient group, as measured WHYMPI scores, are shown in Table 2. Patients with CRPS exhibited higher scores for pain severity, interference, and affective distress, and lower scores for life control compared with the normative data of a heterogeneous chronic pain sample provided by Kerns et al.25
Patients with CRPS showed impaired empathic ability compared with the healthy controls. No difference was observed with respect to the Fantasy subscale of the IRI, but the patients exhibited significantly lower scores relative to healthy controls on the Perspective-taking (14.56 vs. 17.69, t=-2.716, p=0.009) and Empathic Concern (14.97 vs. 18.42, t=-3.282, p=0.002) scales and higher scores on the Personal Distress scale (17.28 vs. 11.56, t=4.575, p<0.001) (Table 3). The analysis of covariance showed that these differences remained significant after adjusting for age, years of education, and gender: Perspective-taking (F=6.582, p=0.013), Empathic Concern (F=6.582, p=0.007), and Personal Distress (F=15.603, p<0.001). As expected, BDI and BAI scores were significantly higher, and WHO-QOL scores were lower among patients with CRPS relative to the control group (Table 3).
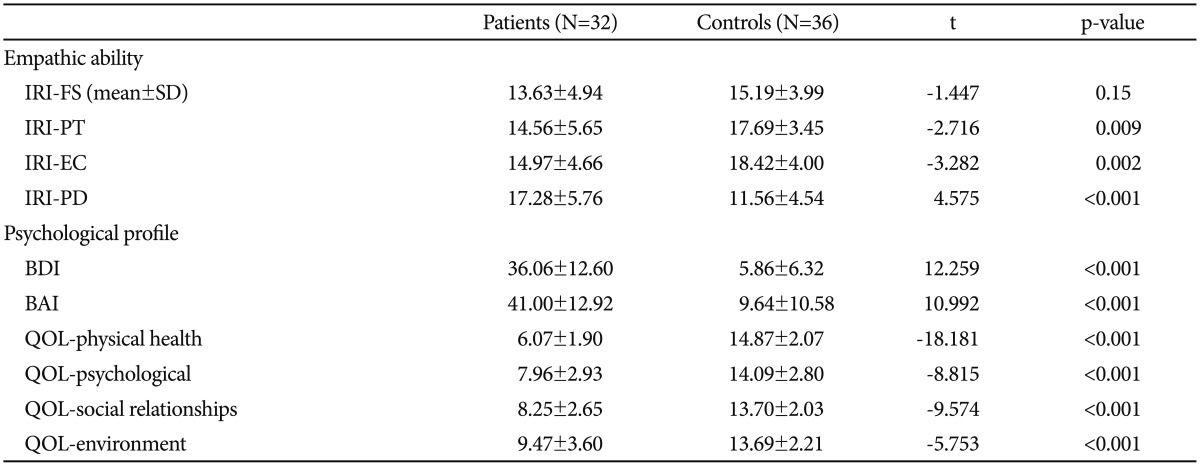
Comparison of empathic abilities and psychological profiles between patients with CRPS and healthy control subjects
Correlations of each subscale of the IRI with pain measures and psychological variables were also examined and are presented in Figure 1. Scores on the IRI Fantasy scale were not correlated with any other variables. Scores on the IRI Perspective-taking scale exhibited a positive correlation with WHYMPI scores for life control (Pearson's r=0.459, p=0.008) and negative correlations with BDI (r=-0.384, p=0.030) and BAI scores (r=-0.351, p=0.049). Scores on the IRI Empathic Concern scale were not correlated with the psychological profile measures, but they were positively correlated with WHYMPI scores for pain severity (r=0.361, p=0.042) and support (r=0.353, p=0.047). Scores on the IRI Personal Distress scale were positively correlated with BDI scores (r=0.424, p=0.015) and WHYMPI scores for affective distress (r=0.382, p=0.031); they were negatively correlated with WHOQOL scores for psychological health (r=-0.434, p=0.013), social relationships (r=-0.441, p=0.013), and environment (r=-0.527, p=0.002) and with WHYMPI scores for general activity (r=-0.457, p=0.008). When corrected for age, gender, and education, most of the above results remained significant, with the exceptions of the correlations between perspective taking and BAI, between empathic concern and support, and correlations of personal distress with affective distress, BDI scores, and BAI scores.

Correlations of each subscale of the IRI with pain measures and psychological variables. IRI-PT scale exhibited a negative correlations with BDI and BAI scores (A and B). IRI-EC scale were positively correlated with WHYMPI scores for pain severity and support (C and D). IRI-PD scale were negatively correlated with WHOQOL scores for social relationships and WHYMPI scores for general activity (E and F). IRI: Interpersonal Reactivity Index, FS: fantasy scale, PT: perspective taking, EC: empathic concern, PD: personal distress, BDI: Beck Depression Index, BAI: Beck Anxiety Index, MPI: West Haven-Yale Multidimensional Pain Inventory, PS: pain severity, S: support, GA: general activity, QOL: WHO quality of life instruments, SO: social relations.
DISCUSSION
Patients with CRPS showed impairments with respect to both the cognitive and emotional dimensions of empathic ability, exhibiting decreased perspective taking (cognitive empathy) and empathic concern (emotional empathy), and increased personal distress (emotional empathy) relative to HCs.
Lower scores on the IRI Perspective-taking scale were associated with higher scores on the BDI and BAI, implying that such deficits in theory of mind13 might lead to more profound emotional distress among patients with CRPS. A positive correlation between scores on the IRI Perspective-taking scale and WHYMPI scores pertaining to life control suggests that chronic pain patients' feelings of loss of control over their lives may result from impaired social interactions with others.
Among the IRI subscales, only Empathic Concern demonstrated a positive correlation with pain severity scores on the WHYMPI. This result is compatible with previous findings of positive correlations between pain ratings and IRI Empathic Concern scores in response to pictures of painful stimuli among patients with chronic pain disorder.31 Moreover, a positive correlation has been observed between scores on the IRI Empathic Concern scale and brain activity (in the ACC and AI) in response to perception of vicarious pain among normal individuals and patients with congenital insensitivity to pain.104950 The correlation between severity of pain and empathic concern suggests two possible explanations: patients with higher emotional empathic ability may be more sensitive to their own pain as well as to the pain of others, or patients may become more sensitive to others' pain after experiencing chronic pain. However, in light our finding of lower emotional empathic ability among patients with CRPS than among healthy controls, the former explanation appears to be preferable, given that patients with lower empathic ability reported lower scores on pain severity, indicating disrupted self-perception of pain. There is evidence that chronic pain may result in abnormal processing (down-regulation) of the "affective pain network" of the brain (in the ACC and AI), which is also engaged as part of the emotional and pain empathy network.31 Whether due to a modification caused by chronic pain or to an underlying CNS abnormality, previous reports indicate an alteration in the interoceptive representation of affective pain and emotional self-awareness among patients with CRPS.89 A lack of emotional awareness is a well-known characteristic among patients with chronic pain.51525354 Furthermore, higher levels of alexithymia have been frequently reported among patients with CRPS.55 The AI and the ACC are crucial both for representing one's own affective states and for experiencing the affective states of others, suggesting a mediating role of "affective pain/emotional self-awareness" between empathic ability and one's own perception of pain as expressed on self-report scales. Therefore, impaired empathic concern for others may not be the direct result of the presenting pain, but may instead point to an anomaly in perception and self-awareness pertaining to affective dimensions of pain among patients with CRPS Type I.
The positive correlation between IRI Empathic Concern scores and WHYMPI scores related to support suggests that support from others may improve the emotional empathic abilities of patients, or vice versa, that better emotional empathy may result in better support from others.
The higher scores on the IRI Personal Distress scale among patients relative to healthy controls indicate that patients with CRPS experience a higher degree of self-oriented distress. A greater susceptibility to such emotional distress can be assumed be a result of chronic pain1156 a notion that is supported in the present study by the positive correlations between personal distress and BDI and between personal distress and WHYMPI scores measuring affective distress. Such imbalanced emotional empathic ability may have an impact not only on subjective emotional distress but also, and particularly, on distress in social contexts. Our results showed that higher IRI Personal Distress score among patients with CRPS were associated with poorer quality of life, specifically in the social relationships and environment subdomains of the WHOQOL, as well as with poor general activity in daily life.
Increased self-oriented distress (as reflected by higher IRI Personal Distress scores) among patients with CRPS, presumably as a consequence of chronic pain, is not surprising. However, together with a lack of emotional empathy for others (as demonstrated by lower IRI Empathic Concern scores), a notable trend toward self-oriented distress among patients with CRPS could have negative effects on their social lives. The coexistence of impaired emotional empathic ability (lower IRI Empathic Concern scores), a lack of self-awareness pertaining to affective pain, and impaired cognitive empathic ability (lower IRI Perspective-taking scores) may result in poor skills in communicating pain5758 potentially increasing the discrepancy between clinicians' and patients' perception of pain.2859
As a result, clinical attention to the affective dimensions of pain is needed when assessing patients with CRPS. Assessing the empathic abilities of patients may be helpful for understanding the subjective emotional distress deriving from the pain, for determining the factors that are related to patients' social functioning, and for decreasing the gap between clinicians' and patients' understanding of pain.60 Improving emotional awareness in patients with CRPS, for example, via mindfulness-based intervention, interpersonal psychotherapy and group psychotherapy, may help to improve patients' emotional empathic abilities, their regulation of the affective dimensions of pain, and the overall quality of their social lives.61626465 Furthermore, efforts directed at strengthening cognitive empathic abilities by improving theory of mind, for example via cognitive behavioral therapy6667 may help patients with CRPS to take greater control of their lives. Enhanced communication of pain, derived from improvements in theory of mind capabilities, would increase the probability of appropriate pain management for such patients.
The limitations of this study pertain primarily to its methodology, as all of the data were obtained through self-report questionnaires. Additionally, the small sample size and the failure to consider the effects of medication on empathic abilities also limit the generalizability of the results. Gender differences have been demonstrated for each subscale of the IRI, with a tendency for women to score higher than men on each subscale,1335 whereas reports on age differences remain controversial.686970 In our study, these variables, which did not differ across groups, were taken into consideration as potential confounders in our analysis, as was education, which did differ across groups. However, we did not assess intelligence, which may be a factor influencing self-report measures of empathic ability. Though not proven to be confounding factors, demographic data addressing the life pattern of the subjects such as body mass index, cigarette smoking was not included in the assessment, and could be pointed out as a limitation. Additionally, all participants being confined to Asian, the result of this study could not reflect any potential ethnic differences, thus limiting the generalizability.
Further investigation, including neuroimaging studies of altered brain function encompassing the pathophysiology of CRPS and related neurocognitive functions is needed to identify the underlying mechanisms of impaired empathic ability among patients with CRPS. It would also be useful to compare patients with CRPS with those suffering from other chronic pain conditions and to conduct clinical trials targeting empathic ability.
Despite these limitations, the present study is the first to assess the empathic abilities of patients with CRPS. Impaired empathic ability was observed among patients with CRPS Type I compared with HCs, indicating a notable trend toward self-oriented distress in emotional empathic ability, reflecting not only patients' emotional distress from the pain itself but also difficulties in their social lives. These results illuminate the importance of assessing the empathic abilities of patients with CRPS in clinical practice to achieve better communication regarding pain and more comprehensive management of chronic pain.
Acknowledgments
The authors thank all the participants in this study, especially from the CRPS support organization, Korea. This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT & Future Planning (2014R1A1A1004553).