|
 |
- Search
| Psychiatry Investig > Volume 17(5); 2020 > Article |
|
Abstract
Objective
Methods
Results
ACKNOWLEDGEMENTS
The authors have no potential conflicts of interest to disclose.
Author Contributions
Conceptualization: Rong Pan, Liqing Zhang. Data curation: Rong Pan, Liqing Zhang. Formal analysis: Rong Pan, Liqing Zhang. Funding acquisition: Jiyang Pan. Investigation: Rong Pan, Liqing Zhang. Methodology: Rong Pan, Liqing Zhang. Project administration: Rong Pan, Liqing Zhang. Resources: Rong Pan, Liqing Zhang. Software: Rong Pan, Liqing Zhang. Supervision: Jiyang Pan. Validation: Rong Pan, Liqing Zhang. Visualization: Rong Pan, Liqing Zhang. WritingŌĆöoriginal draft: Rong Pan, Liqing Zhang. WritingŌĆöreview & editing: Rong Pan, Liqing Zhang, Jiyang Pan.
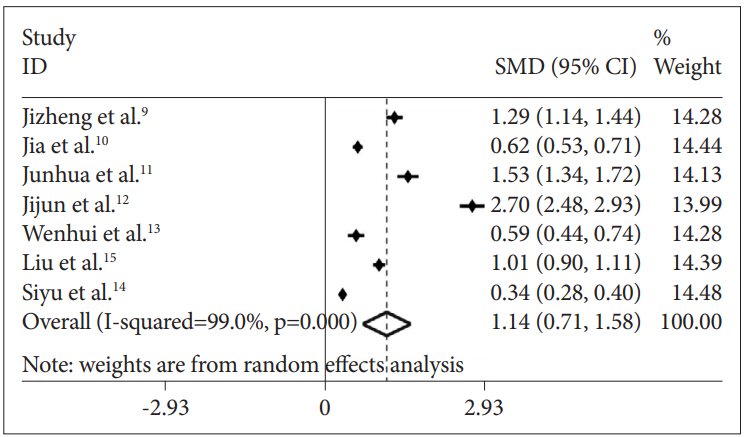
Figure┬Ā3.
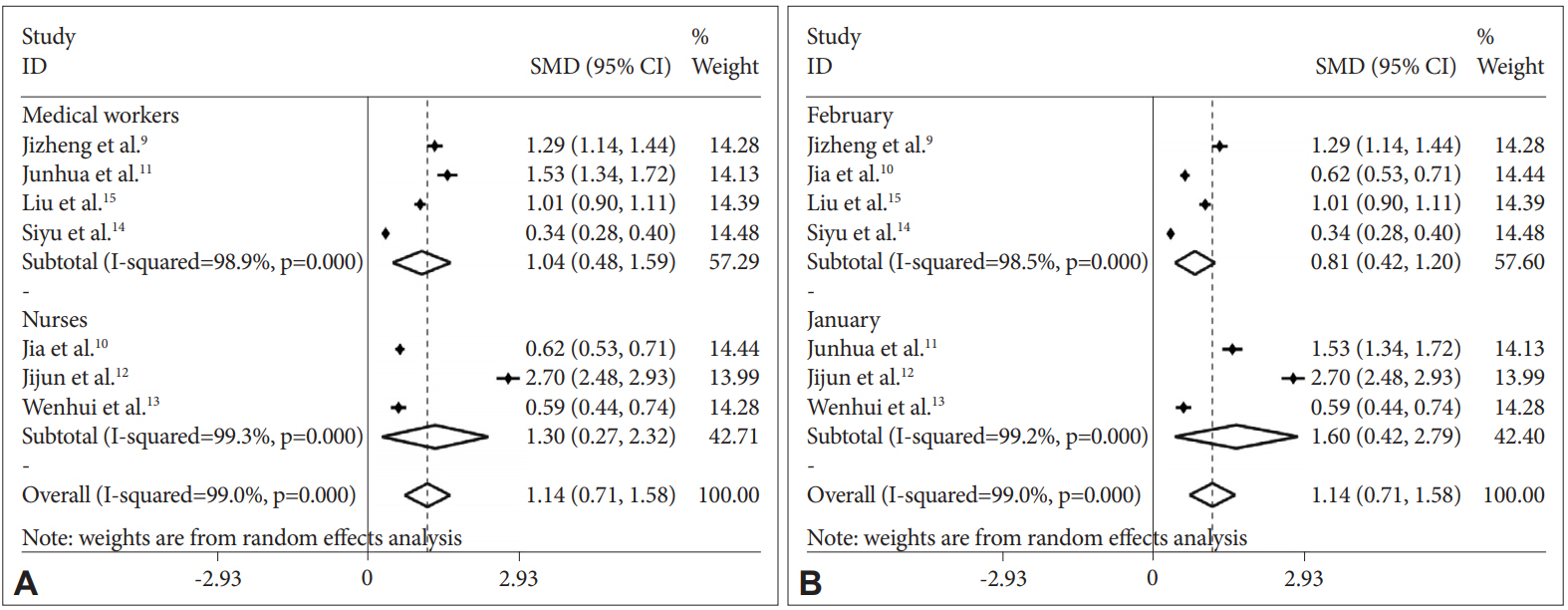
Figure┬Ā4.
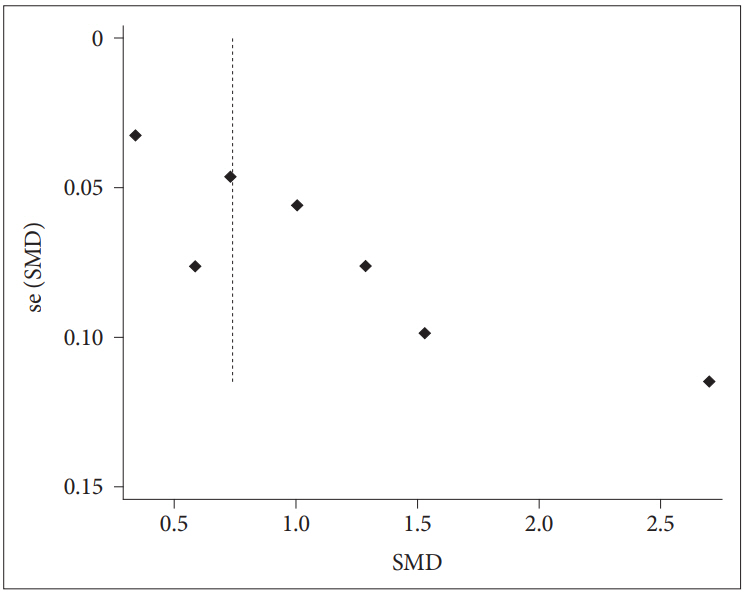
Table┬Ā1.
| Author | Region | Sample size | Study subjects | Main results | Quality assessment |
|---|---|---|---|---|---|
| Jizheng et al. [9] | Fuyang, China | 230 | Front-line medical staff of Fuyang city second peopleŌĆÖs hospital | SAS: 42.91┬▒10.89; | 15 |
| PTSD-SS: 42.92┬▒17.88 | |||||
| Jia et al. [10] | Mianyang, China | 867 | Nurse of Mianyang Central Hospital | SAS: 34.97┬▒5.493 | 14 |
| TAF: 8.33┬▒5.456 | |||||
| Junhua et al. [11] | Wuhan, China | 126 | Front-line medical staff with confirmed or suspected novel coronavirus infection | PHQ-15: (9.72┬▒1.604)/(3.47┬▒1.55) | 18 |
| SAS: (45.47┬▒1.405)/(43.47┬▒2.779) | |||||
| SDS: (51.25┬▒1.611)/(35.00┬▒3.055) | |||||
| PCL-C: (34.81┬▒1.36)/(30.75┬▒1.159) | |||||
| PSQI: (14.00┬▒3.874)/(10.36┬▒3.39) | |||||
| Jijun et al. [12] | Sichuan, China | 106 | Front-line nurses | PSQI: 7.96┬▒2.12; | 13 |
| SAS: 56.39┬▒6.99 | |||||
| Wenhui et al. [13] | Hangzhou, China | 207 | Front-line nurse of Xixi Hospital of Hangzhou | SAS: 35.43┬▒6.66 | 14 |
| Siyu et al. [14] | China | 5,393 | Physicians, Nurses, Clinical Assistants and medical students | SAS: 32.80┬▒8.60 | 18 |
| ISI: 6.10┬▒5.00 | |||||
| Liu et al. [15] | China | 512 | Front-line medical staff | SAS: 39.56┬▒8.91 | 19 |
SAS: Self-rating Anxiety Scale, PTSD-SS: Post-Traumatic Stress Disorder Self-rating Scale, TAF: The Triage Assessment Form, PHQ-15: Patient Health Questionnaire, SDS: Self-rating Depression Scale, PCL-C: Post-Traumatic Stress Disorder self-assessment scale (PTSD Checklist-Civilian Version), PSQI: Pittsburgh Sleep Quality Index, ISI: Insomnia Severity Index
Table┬Ā2.
| Studies |
Comparison with Chinese anxiety norm |
||
|---|---|---|---|
| SMD | 95% CI | Weight % | |
| Jizheng et al. [9] | 1.286 | 1.137-1.435 | 14.29 |
| Jia et al. [10] | 0.616 | 0.526-0.706 | 14.44 |
| Junhua et al. [11] | 1.531 | 1.338-1.724 | 14.13 |
| Jijun et al. [12] | 2.701 | 2.476-2.926 | 13.99 |
| Wenhui et al. [13] | 0.587 | 0.437-0.736 | 14.28 |
| Siyu et al. [14] | 1.005 | 0.896-1.115 | 14.39 |
| Liu et al. [15] | 0.340 | 0.276-0.404 | 14.48 |
| Overall | 1.145 | 0.705-1.584 | 100.00 |
| Heterogeneity test: Žć2=591.07ŌĆādf=6 (p<0.001)ŌĆāI2=99.0% | |||
| Test of SMD: z=5.10 (p<0.001) | |||
REFERENCES