 |
 |
- Search
| Psychiatry Investig > Volume 19(12); 2022 > Article |
|
Abstract
Objective
Methods
Results
Conclusion
Notes
Availability of Data and Material
The data supporting the findings of this study are not publicly available due to ethical restrictions for protecting participants’ confidentiality and privacy but are accessible from the corresponding author on reasonable request with the approval of the Institutional Review Board of CHA Bundang Medical Center.
Conflicts of Interest
Minji Bang, a contributing editor of the Psychiatry Investigation, was not involved in the editorial evaluation or decision to publish this article. All remaining authors have declared no conflicts of interest.
Author Contributions
Conceptualization: Minji Bang, Sang-Hyuk Lee. Data curation: Wonsuk Shin, Sra Jung, Minji Bang. Formal analysis: Naok Kang, Wonsuk Shin. Funding acquisition: Minji Bang. Investigation: Wonsuk Shin, Sra Jung, Sang-Hyuk Lee. Methodology: Wonsuk Shin, Sang-Hyuk Lee. Project administration: Minji Bang, Sang-Hyuk Lee. Resources: Minji Bang, Sang- Hyuk Lee. Software: Naok Kang. Supervision: Minji Bang. Validation: Minji Bang. Visualization: Naok Kang, Minji Bang. Writing—original draft: Naok Kang. Writing—review & editing: Minji Bang, Sang-Hyuk Lee.
Funding Statement
This study was supported by the Basic Science Research Program through the National Research Foundation funded by the Ministry of Science and ICT, Republic of Korea (grant no. NRF-2021R1C1C1012901 and NRF-2018R1D1A1B07050493). The funding sources had no role in the study design, collection, analysis, and interpretation of data, in the writing of the report, or in the decision to submit the paper for publication.
Figure 1.
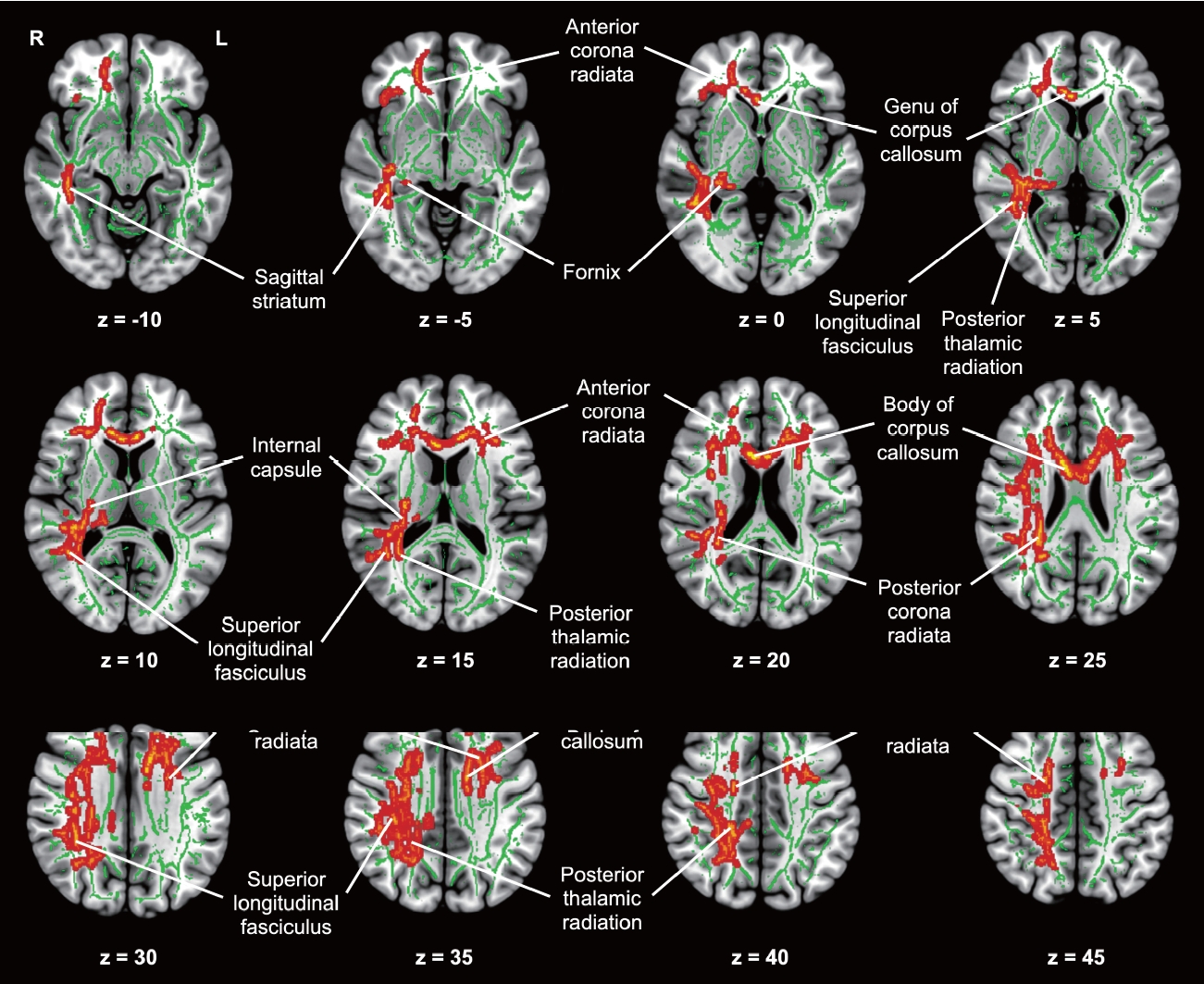
Figure 2.
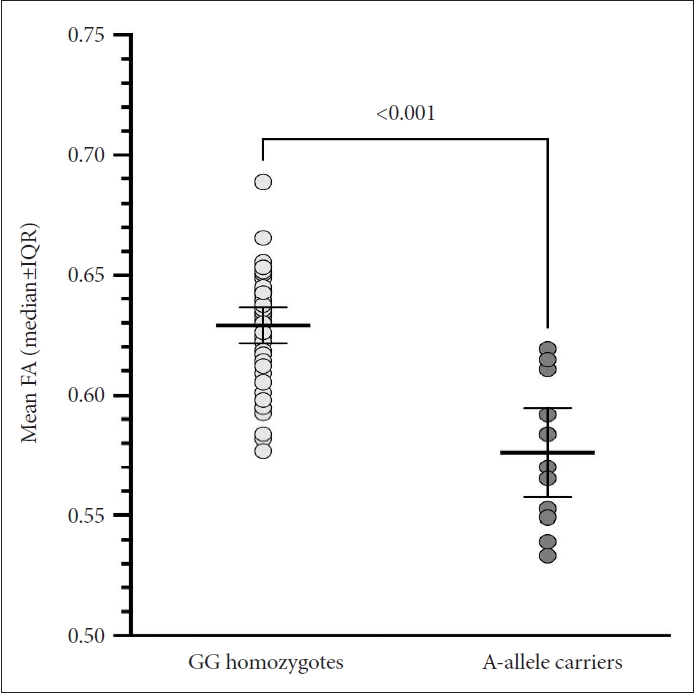
Figure 3.

Table 1.
| GG homozygotes (N=43) | A-allele carriers (N=12) | Statistics | p | |||
|---|---|---|---|---|---|---|
| Sex | χ2=0.422 | 0.530 | ||||
| Male, N (%) | 17 (39.5) | 6 (50.0) | ||||
| Female, N (%) | 26 (60.5) | 6 (50.0) | ||||
| Age (yr) | U=201.5 | 0.249 | ||||
| Mean±SD | 35.2±9.2 | 39.7±10.6 | ||||
| Median (IQR) | 33 (27-43) | 44 (27-47) | ||||
| Education (yr) | U=49.5 | 0.107 | ||||
| Mean±SD | 13.0±2.4 | 11.4±1.3 | ||||
| Median (IQR) | 12 (12-16) | 12 (10-12) | ||||
| Duration of illness (mon) | U=232.0 | 0.589 | ||||
| Mean±SD | 24.5±48.6 | 63.4±97.3 | ||||
| Median (IQR) | 5 (1-36) | 7 (1-117) | ||||
| Intracranial volume (mL) | U=159.0 | 0.231 | ||||
| Mean±SD | 1,472.8±169.8 | 1,535.2±144.5 | ||||
| Median (IQR) | 1,484 (1,331-1,612) | 1,538 (1,408-1,621) | ||||
| Total duration of antipsychotic treatment before MRI scan (d) | U=178.5 | 0.339 | ||||
| Mean±SD | 54.3±218.9 | 8.1±6.3 | ||||
| Median (IQR) | 5 (2-10) | 6 (4-13) | ||||
| Antipsychotic medications (mg/d)* | U=71.5 | 0.553 | ||||
| Mean±SD | 453.6±213.4 | 500.0±167.3 | ||||
| Median (IQR) | 400 (325-600) | 400 (400-650) | ||||
| SAPS composite score† | U=160.0 | 0.285 | ||||
| Mean±SD | 57.6±19.0 | 48.5±15.7 | ||||
| Median (IQR) | 57 (41-68) | 49 (38-64) | ||||
| SAPS subscales† | ||||||
| Hallucination | U=150.5 | 0.194 | ||||
| Mean±SD | 12.5±4.9 | 10.3±4.9 | ||||
| Median (IQR) | 13 (8-16) | 12 (6-14) | ||||
| Delusion | U=163.0 | 0.318 | ||||
| Mean±SD | 19.8±9.3 | 15.9±6.0 | ||||
| Median (IQR) | 20 (12-26) | 15 (13-21) | ||||
| Bizarre behavior | U=176.0 | 0.490 | ||||
| Mean±SD | 9.0±4.9 | 7.9±3.8 | ||||
| Median (IQR) | 9 (7-13) | 8 (5-11) | ||||
| Positive formal thought disorder | U=193.0 | 0.775 | ||||
| Mean±SD | 16.4±6.7 | 14.4±6.9 | ||||
| Median (IQR) | 14 (12-22) | 16 (10-19) | ||||
| SANS composite score† | U=167.5 | 0.373 | ||||
| Mean±SD | 50.6±17.9 | 45.1±18.2 | ||||
| Median (IQR) | 51 (39-63) | 44 (38-55) | ||||
| SANS subscale† | ||||||
| Affective flattening or blunting | U=158.0 | 0.264 | ||||
| Mean±SD | 16.7±7.0 | 13.6±7.2 | ||||
| Median (IQR) | 17 (11-22) | 13 (9-20) | ||||
| Alogia | U=151.5 | 0.203 | ||||
| Mean±SD | 9.6±4.2 | 7.4±5.0 | ||||
| Median (IQR) | 10 (7-13) | 8 (3-11) | ||||
| Avolition-apathy | U=189.0 | 0.702 | ||||
| Mean±SD | 8.3±2.9 | 8.0±2.7 | ||||
| Median (IQR) | 8 (6-10) | 8 (6-10) | ||||
| Anhedonia-asociality | U=196.5 | 0.840 | ||||
| Mean±SD | 11.1±4.8 | 11.5±4.0 | ||||
| Median (IQR) | 12 (8-14) | 11 (10-13) | ||||
| Attention | U=185.0 | 0.631 | ||||
| Mean±SD | 5.0±2.2 | 4.6±2.1 | ||||
| Median (IQR) | 5 (4-7) | 5 (4-6) | ||||
Table 2.
REFERENCES







