4. Chan KY, Zhao FF, Meng S, Demaio AR, Reed C, Theodoratou E, et al. Prevalence of schizophrenia in China between 1990 and 2010. J Glob Health 2015;5:010410


5. Chien IC, Chou YJ, Lin CH, Bih SH, Chou P, Chang HJ. Prevalence and incidence of schizophrenia among national health insurance enrollees in Taiwan, 1996-2001. Psychiatry Clin Neurosci 2004;58:611-618.


6. Soares-Weiser K, Maayan N, Bergman H, Davenport C, Kirkham AJ, Grabowski S, et al. First rank symptoms for schizophrenia. Cochrane Database Syst Rev 2015;1:CD010653


7. Dziwota E, Stepulak MZ, Włoszczak-Szubzda A, Olajossy M. Social functioning and the quality of life of patients diagnosed with schizophrenia. Ann Agric Environ Med 2018;25:50-55.


9. Birnbaum ML, Rizvi AF, Confino J, Correll CU, Kane JM. Role of social media and the Internet in pathways to care for adolescents and young adults with psychotic disorders and non-psychotic mood disorders. Early Interv Psychiatry 2017;11:290-295.

12. Trefflich F, Kalckreuth S, Mergl R, Rummel-Kluge C. Psychiatric patients’ internet use corresponds to the internet use of the general public. Psychiatry Res 2015;226:136-141.


14. Torous J, Keshavan M. The role of social media in schizophrenia: evaluating risks, benefits, and potential. Curr Opin Psychiatry 2016;29:190-195.

15. Lopes LS, Valentini JP, Monteiro TH, Costacurta MCF, Soares LON, Telfar-Barnard L, et al. Problematic social media use and its relationship with depression or anxiety: a systematic review. Cyberpsychol Behav Soc Netw 2022;25:691-702.


22. Cohrs S. Sleep disturbances in patients with schizophrenia: impact and effect of antipsychotics. CNS Drugs 2008;22:939-962.


23. Esan O, Ephraim-Oluwanuga OT. Sleep quality and cognitive impairments in remitted patients with schizophrenia in Nigeria. Encephale 2021;47:401-405.


27. Alonzo R, Hussain J, Stranges S, Anderson KK. Interplay between social media use, sleep quality, and mental health in youth: a systematic review. Sleep Med Rev 2021;56:101414


28. Mohammadbeigi A, Absari R, Valizadeh F, Saadati M, Sharifimoghadam S, Ahmadi A, et al. Sleep quality in medical students; the impact of over-use of mobile cell-phone and social networks. J Res Health Sci 2016;16:46-50.


29. Morgades-Bamba CI, Fuster-Ruizdeapodaca MJ, Molero F. Internalized stigma and its impact on schizophrenia quality of life. Psychol Health Med 2019;24:992-1004.


33. Mannarini S, Taccini F, Sato I, Rossi AA. Understanding stigma toward schizophrenia. Psychiatry Res 2022;318:114970


35. Lien YJ, Chang HA, Kao YC, Tzeng NS, Lu CW, Loh CH. Insight, selfstigma and psychosocial outcomes in schizophrenia: a structural equation modelling approach. Epidemiol Psychiatr Sci 2018;27:176-185.


38. Little RJA. A test of missing completely at random for multivariate data with missing values. J Am Stat Assoc 1988;83:1198-1202.

40. The WHOQOL Group. Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychol Med 1998;28:551-558.


41. Yao G, Chung CW, Yu CF, Wang JD. Development and verification of validity and reliability of the WHOQOL-BREF Taiwan version. J Formos Med Assoc 2002;101:342-351.

44. Lin CY, Li YP, Lin SI, Chen CH. Measurement equivalence across gender and education in the WHOQOL-BREF for community-dwelling elderly Taiwanese. Int Psychogeriatr 2016;28:1375-1382.


45. Lin CY, Hwang JS, Wang WC, Lai WW, Su WC, Wu TY, et al. Psychometric evaluation of the WHOQOL-BREF, Taiwan version, across five kinds of Taiwanese cancer survivors: Rasch analysis and confirmatory factor analysis. J Formos Med Assoc 2019;118:215-222.


46. Su CT, Ng HS, Yang AL, Lin CY. Psychometric evaluation of the Short Form 36 Health Survey (SF-36) and the World Health Organization Quality of Life Scale Brief Version (WHOQOL-BREF) for patients with schizophrenia. Psychol Assess 2014;26:980-989.


47. Buysse DJ, Reynolds CF 3rd, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 1989;28:193-213.


51. Mak WW, Cheung RY. Self-stigma among concealable minorities in Hong Kong: conceptualization and unified measurement. Am J Orthopsychiatry 2010;80:267-281.


53. Chen IH, Chang KC, Chang CW, Huang SW, Potenza MN, Pakpour AH, et al. Temporal associations between problematic use of the internet and self-stigma among people with substance use disorders: a crosslagged model across one year. J Psychiatr Res 2022;156:339-348.


58. Schou Andreassen C, Billieux J, Griffiths MD, Kuss DJ, Demetrovics Z, Mazzoni E, et al. The relationship between addictive use of social media and video games and symptoms of psychiatric disorders: a largescale cross-sectional study. Psychol Addict Behav 2016;30:252-262.


59. Griffiths M. A ‘components’ model of addiction within a biopsychosocial framework. J Subst Use 2005;10:191-197.

67. Chen IH, Strong C, Lin YC, Tsai MC, Leung H, Lin CY, et al. Time invariance of three ultra-brief internet-related instruments: Smartphone Application-Based Addiction Scale (SABAS), Bergen Social Media Addiction Scale (BSMAS), and the nine-item Internet Gaming Disorder Scale - Short Form (IGDS-SF9) (Study Part B). Addict Behav 2020;101:105960


68. Leung H, Pakpour AH, Strong C, Lin YC, Tsai MC, Griffiths MD, et al. Measurement invariance across young adults from Hong Kong and Taiwan among three internet-related addiction scales: Bergen Social Media Addiction Scale (BSMAS), Smartphone Application-Based Addiction Scale (SABAS), and Internet Gaming Disorder Scale-Short Form (IGDS-SF9) (Study Part A). Addict Behav 2020;101:105969


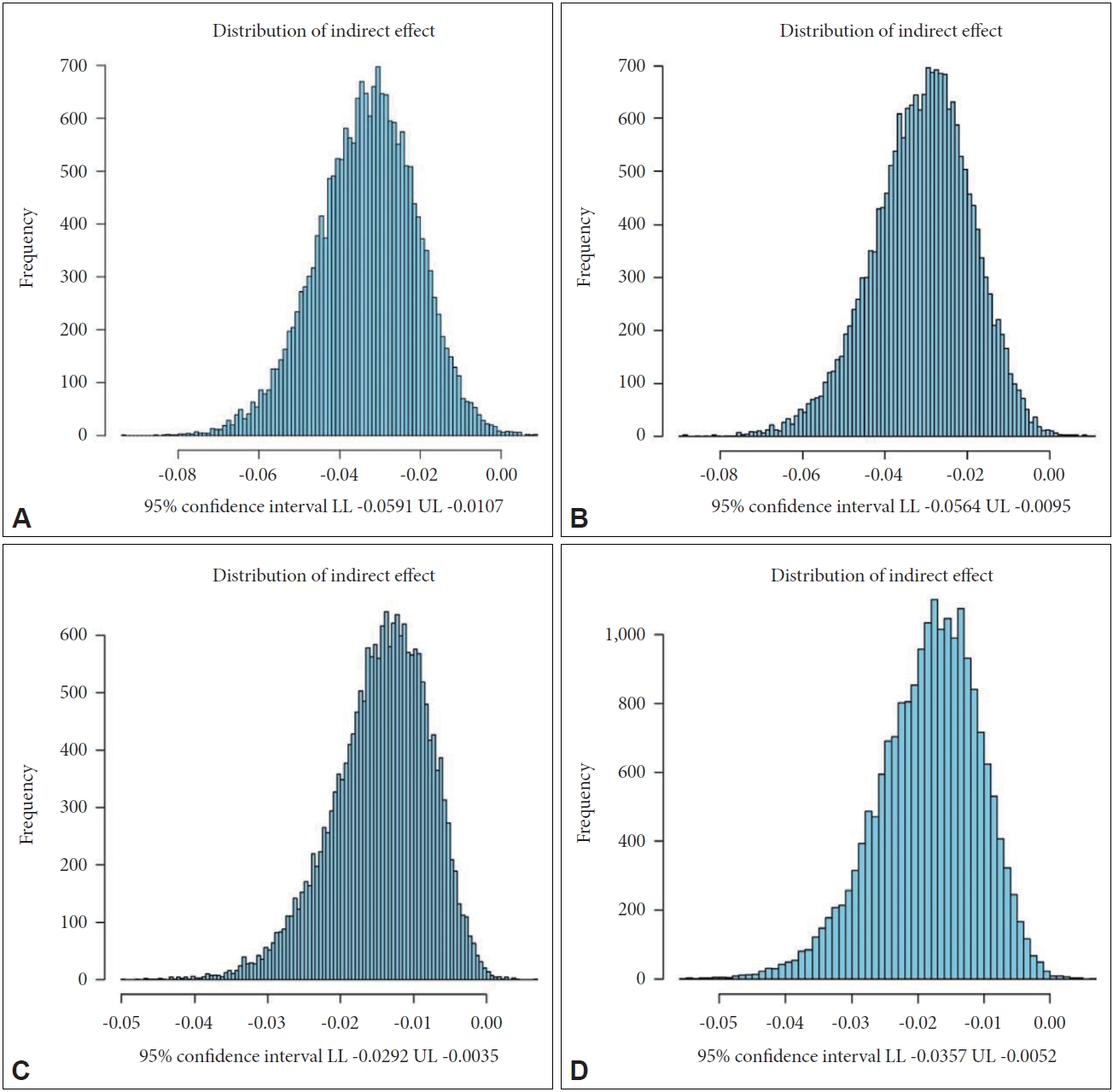
69. Preacher KJ, Selig JP. Advantages of Monte Carlo confidence intervals for indirect effects. Commun Methods Meas 2012;6:77-98.

70. Bauer DJ, Preacher KJ, Gil KM. Conceptualizing and testing random indirect effects and moderated mediation in multilevel models: new procedures and recommendations. Psychol Methods 2006;11:142-163.


71. Xiang YT, Wang CY, Chiu HF, Weng YZ, Bo QJ, Chan SS, et al. Sociodemographic and clinical profiles of paranoid and nonparanoid schizophrenia: a prospective, multicenter study in China. Perspect Psychiatr Care 2011;47:126-130.