 |
 |
- Search
| Psychiatry Investig > Volume 20(12); 2023 > Article |
|
Abstract
Objective
Methods
Results
Conclusion
Notes
Availability of Data and Material
The datasets generated or analyzed during the study are available from the corresponding author on reasonable request.
Conflicts of Interest
The authors have no potential conflicts of interest to disclose.
Author Contributions
Conceptualization: Deuk-Kweon You, Jeoung-Mo Son. Data curation: Deuk-Kweon You, Jeoung-Mo Son. Formal analysis: Deuk-Kweon You. Investigation: Deuk-Kweon You, Jeoung-Mo Son. Methodology: Deuk-Kweon You. Project administration: Tae-Yeon Hwang. Supervision: Tae-Yeon Hwang. Writing—original draft: Deuk-Kweon You. Writing—review & editing: Deuk-Kweon You, Tae-Yeon Hwang.
Funding Statement
This research was supported by a fund (project no. 2022-03) for a research of the Korea Foundation for Suicide Prevention.
ACKNOWLEDGEMENTS
Figure 1.
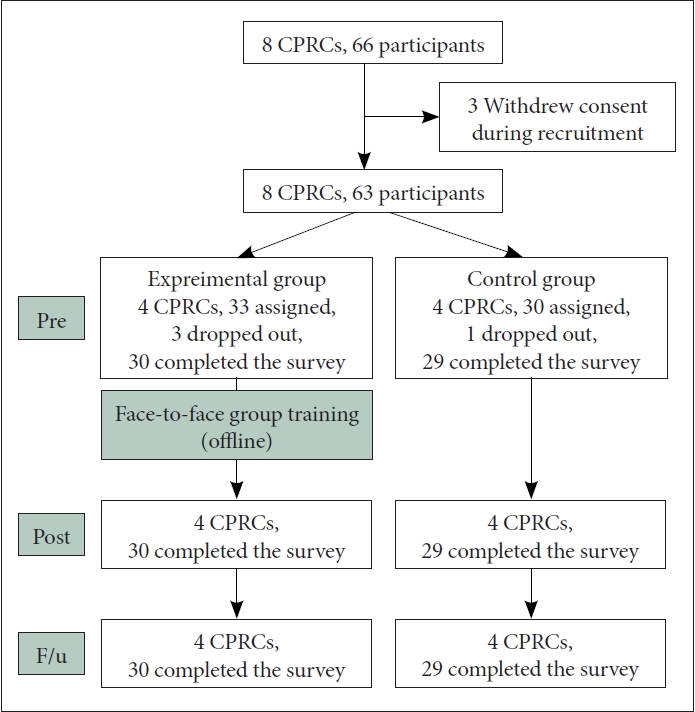
Figure 2.
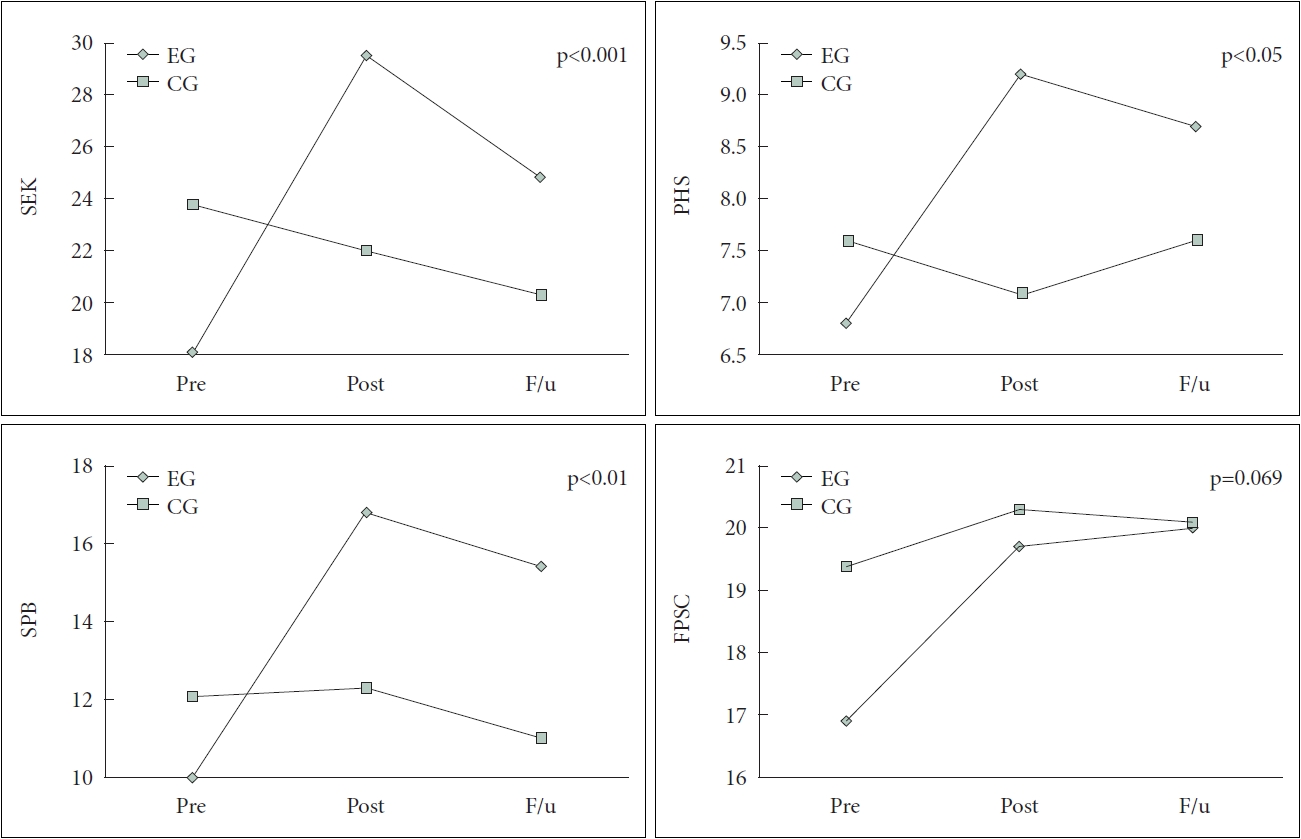
Table 1.
Table 2.
Values are presented number or number (%). χ2: chi-square test. Fisher’s: Fisher’s exact test. PMD, people with mental disorder; SPR, schizophrenia; SAD, schizoaffective disorder; MDD, major depressive disorder; BD, bipolar disorder; ADHD, attention-deficit hyperactivity disorder; CPRC: community psychiatric rehabilitation center
Table 3.
| Variable |
Experimental group (N=30) |
Control group (N=29) |
F Interaction | ||||
|---|---|---|---|---|---|---|---|
| Pre-training | Post-training | F/u | Pre-training | Post-training | F/u | ||
| SEK | 18.13±12.16 | 29.50±10.21 | 24.83±10.71 | 23.83±10.94 | 22.03±11.35 | 20.34±11.16 | 11.72*** |
| ATTS | 44.77±8.35 | 44.13±8.18 | 44.60±7.73 | 45.59±7.93 | 42.76±6.71 | 47.31±8.74 | 1.63 |
| PHS | 6.87±3.85 | 9.20±3.24 | 8.73±3.07 | 7.66±2.27 | 7.14±2.97 | 7.66±2.89 | 3.88* |
| SPB | 10.07±8.41 | 16.83±5.90 | 15.43±6.11 | 12.14±6.34 | 12.34±5.37 | 11.07±6.16 | 6.03** |
| FPSC | 16.97±5.36 | 19.70±4.47 | 20.07±4.57 | 19.45±4.21 | 20.31±3.72 | 20.14±3.99 | 2.73† |
ANOVA, analysis of variance; SPEM-F, suicide prevention education program for families of people with mental disorders; F/u, follow-up; SEK, self-evaluation of knowledge in suicide prevention; ATTS, attitude toward suicide; PHS, preparedness to help; SPB, suicide prevention behavior; FPSC, family problem solving communication
REFERENCES
-
METRICS

-
- 1 Crossref
- Scopus
- 1,270 View
- 37 Download






